I woke one January morning, 33 years ago, and knew immediately something was different. As I stretched in the bed, I realised I had not been woken by somebody pulling me out of a sleep I wanted to stay in.
The clock said 11.10am, a whole 10 hours of sleep.
I had gone to bed at 1.30am after a game of Monopoly with my flatmates – a miracle after the previous five weeks and three days. I felt brilliant and full of anticipation. The deadline for registering a birth was six weeks postpartum, and this was the second last day until the cut-off point. Busy day ahead.
I swung out of bed and walked the few paces to my baby’s cot. She was still asleep, but I would have a quick peek before I went to the loo. I had a full bladder, and breasts that were like bricks they were so full of milk.
I remember some of the images but I did not remember the emotions for many years. I blocked the feelings to protect. Even now, as I write, I am trying not to cry – crying will impede my vision and therefore, my typing.
My baby, Stephany, was dead.
I knew straightaway she was gone and as I instinctively picked her up I knew she had been dead for hours. Her body was like a board – all of the soft limbs and the head, that normally needed supporting, stayed stiffly in her sleep position, like a rigid plastic dolly.
I put her, face up now, on my still-warm bed. The horror of the rigidity came in full force as she retained her sleeping on the tummy pose. I patted her, checking.The patting was like playing a drum. There was a bounce off her skin, she had begun to bloat after the stiffening of rigor mortis. She was blue and purple, not vividly coloured but not the soft pink and cream she should have been. Cold to touch. Very cold. Emotions of horror and fear.
Bless EastEnders
I was never a fan of soaps, but my flatmates were avid watchers of both EastEnders and Coronation Street and these programmes had filtered into my life. Ali and Sue Osman, characters in EastEnders , had a cot death storyline during my pregnancy. My flatmates had worried I would be upset by this, but I reassured them: "Not a bother, not something that should worry me."
So thank you EastEnders. I firmly believe you saved my sanity.
- You had prepared me so I knew what this was.
- You had told me it was not my fault.
- You had warned me the police would arrive on my doorstep.
- You forewarned me that a lot of people would find this kind of death really difficult to deal with.
- You had made it easier – if something like that can be made easier.
I had now been on my own for about 10 minutes. I did not cry but I did moan. I could hear this noise, not realising that it was me. When I became aware of my keening I thought: “ I need to tell someone, I need someone to help me with this.”

Emotions of fear and horror, but I am also very calm. On some form of autopilot, I made my way next door – we had no phone. My neighbour opened his door after a lot of knocking. I asked could I use his phone and told him why. He was shaken, but brought me in. Inviting me to sit, he offered several types of illegal drugs and whiskey from his coffee table array. I refused all and made my call.
I did not dial 999.
This was not an emergency.
She was dead already.
I knew a doctor had to confirm death so I called my GP. He came quickly; from a busy London surgery that did not do house calls. My neighbour came back to my flat with me. I had moved and talked and walked. I had told two people. I finally had a pee.
My neighbour went into my bedroom while I was in the loo and I came out to find him in a very distressed state. He was a drunk and a drug addict – not a neighbour we would go to for a cup of sugar. He had tried to help me, but now he was beginning to unravel. So I minded him.
Kettle on. Two very young and nervous bobbies arrived. If I had not known the protocol, their arrival would have freaked me out. Were they checking up on me to see if I had done something terrible? I know now that of course they were because terrible things do happen and sometimes people do hurt babies.
Because they were so obviously ill at ease I looked after them.
Would they like a cup of tea? Yes.
Would they like to see the baby? Yes.
It was only at this point that I went back into my bedroom and saw Stephany again. I went to touch her, to pick her up. They told me not to. For years I wished that I had wrapped her in a blanket and held her until I had to let her go.
The young policemen asked was I alone? Did I want to call someone? So we trooped back to the phone – one policeman, my neighbour and me. Bless the bobby, he sat at a drug-laden table and never said a word about the amount of product on the table and the weighing scales. (My neighbour was more than just an addict.)
The phone call was tough. My flatmate, Ann, worked at the same company as my brother’s girlfriend Suzanne. I asked to speak to rock-solid-in-a-crisis Suzanne, but the receptionist misheard and put me through to Ann. She was not a girl you related news like this to over the phone. From memory I think I said, “there is something wrong with the baby”. This was to soften the blow, but, somehow, Ann knew immediately.
Endless screaming down the phone, my neighbour started getting agitated again, I put down the phone. Back to my home with just the police. Tea and then the GP arrived with another man. This man explains he is a coroner who is involved in cot death research. Would I mind if he attended? Of course not. I was comforted that she was going to be looked after properly. He was utterly professional and very compassionate. The GP and the young policemen were not in the same league at all.
I will hear her screaming nightmares for many nights and I do not want that
Lots of questions: sleep position, heating on or off, smoker or nonsmoker, time of putting to sleep, time of discovery, had I moved her, had she been ill, feeding method and pattern, other people in the flat, type of delivery... gently put and I knew that Sue and Ali from EastEnders had had to do this, so I knew I had to do it too.
Another knock at the door.
Ann and Suzanne. Suzanne straight to me to embrace, but Ann headed for my bedroom. We broke a barely started hug and instinctively lunged for her and pulled her back. We both knew what would happen if Ann saw Stephany, but I also had the extreme disadvantage of knowing just how horrific my poor dead baby looked. The thought flashed in – I will hear her screaming nightmares for many nights and I do not want that. For her, for me. We physically struggle with Ann. Shouting, distress, but not mine. Ann is not left alone. Suzanne’s hug had triggered the rise of tears which quenched immediately as we intercepted Ann.
The coroner and GP are finished and tell me it is time to take Stephany away. Yes, I know there has to be a postmortem. EastEnders. But does she have to go so soon? I do not hold her before she goes. I want to but I am very conscious of managing the Ann situation. Better to let Stephany go and mind Ann. Would they have let me hold her? I pull back the blanket she is wrapped in as the coroner holds her. I look and ask them to mind her.
Where is she going?
The local hospital. Good, not too far away. They take her carry cot and bedding.
Blurred gaps now.
I do not cry. More people come. Family, friends.
Huge gaps.
Huge crowd that night. Drinking. Not much for me. Very uncomfortable breasts. My brother has made other calls and finds out what needs to be done.
What do I want to do?
Home. To Ireland. I am not really connected to any of this.
Home
On the Friday morning we went to the registry office – myself, Ann, Suzanne, and Stephany’s father, Ray, and my brother, Mark, – to register a birth and a death.
There was a long queue of other new mums with their small babies, including several I had met during my pregnancy. “How are you? Where is baby? What have you called her?”
Blank, completely unable to respond. I do not want to frighten any of these women or spoil this significant moment for them. Mark turns and opens some doors and tells us to go into one that is empty. Retreat, relief. Saves me from unravelling. While he goes and finds someone to explain the awkward queueing situation to, we wait in what turns out to be a wedding ceremony room. Red carpet, red velvet, plush, totally bizarre. Ray jokingly asks would we not get married while we are here. Nobody laughs. Mark comes back with a lovely registrar who has understood the need for some queue jumping. We push through the crowds of mothers and babies on the way out, armed with the paperwork.

I need a birth cert to get a death cert and I need a death cert to get Stephany transported home. We are flying the next day to Shannon. All of the organising is done by other people: flights, liasing with coroners and funeral directors. I know now that there is a huge amount to do to arrange a funeral and an added load for inter-country transport of a body.
People protect me by doing all of this. Thank you. Other people also paid all the bills. Thank you.
A visit to the funeral parlour in the evening. Not good. At some point I was asked for a set of clothes for Stephany. She is wearing them now, but the tiny hat barely covers the wound on the forehead, the postmortem examination of the brain. Mark breaks and I cannot stay without him. I do not know who else is there. I only remember Mark. I needed longer.
More blank time, blurred images. Saturday morning is an early start. I shower, dress and apply some eyeliner at the mirror in the livingroom, an odd thing to do but I follow my routines. Lots of people are there, despite the early hour. All these miserable faces I can see in the mirror. All of my family are travelling home and several friends too. Other friends are coming to the airport.
Someone says that I can have another baby. To comfort me? Shocked faces from the others. I am angry, so angry with that person for years to come. On the way to the airport Tony puts on a tape to fill the silence. Christy Moore dirges on about death, dying, dead. Tony flusters, apologises, swears, shuts off the tape. I feel a terrible hilarity rising in me, but it never surfaces, it snaps in two somewhere on its journey and is replaced by a surge of love for poor Tony and his bad tape choice.
Maggie P sits beside me in the car. She presses something into my hand and says something about “help”. I discover much later that it is £200, which was a lot of money back then. The way-bill for transporting Stephany in the hold of the plane was £67. I still have that bill. I was not happy she would be on her own in the hold.
A funeral, a burial. Mistakes are made. I am numb and shutting down. Help and services are limited. I do not ask and I do not receive.
Why I'm writing
Why do I write this now? Because I can. I have cried. I wish I could have cried back then. I did some crying, but always on my own. I also write because I want you to know how to avoid my mistakes.
Lullaby Trust and ONS reported 1,388 cot death babies in England and Wales (for every 1,000 births, 2.1 babies died) in 1986. The numbers peaked in 1988 with a rate of 2.3, meaning 1,593 babies died. There were 219 cot deaths in 2016 with a rate of 0.31 .
In Ireland, the National Paediatric Mortality Register (NPMR) registered 152 cot death babies in 1986 , but that figure was 20 in 2015 . (Figures for 2016 and 2017 are provisional only and are 17 and 12 respectively.) An extraordinary decrease in a misery making event both here and in the UK but still far too many.
Stephany slept on her tummy. Sleep your baby on their back. I smoked (much reduced but still smoked) during my pregnancy and in my baby’s home. In truth, myself and my two flatmates smoked with Stephany in the room and sometimes there was a fug of smoke. Find a way to stop smoking in pregnancy. If you smoke after your child is born, go outside.

There is a whole other list of dos and don’ts – the following are from the website of the HSE in conjunction with the NPMR. These measures reduce the risk of cot death, but the cause is still an unknown.
- Don't smoke during pregnancy
- Don't smoke or allow anyone to smoke in the home or in the car
- Always place your baby on their back to sleep
- The safest place for your baby to sleep at night is in a cot in your room
- Place baby with their feet to the foot of the cot
- Make sure the baby's head stays uncovered when asleep
- Don't let your baby get too hot
- Keep the cot free of soft objects and anything loose or fluffy
Firstlight (helpline 1850 391 391) are the Irish cot death advisory and counselling service. Cot death is also known as Sudden Infant Death Syndrome (SIDS). Firstlight are part funded by Tusla, but the majority of their financial needs are met through fundraising. They funded the provision of prevention and aftercare support literature when supplies ran out during the recent recession.
Get counselling
I did not get counselling for 15 years. Starting counselling too soon could be counterproductive if a grieving parent is too raw. Starting too late was extremely detrimental for me. A cot death is a severe trauma. It is the unexpected, unexplainable death of a baby. A baby you are in love with. Hormones are raging.
You put your baby to sleep.
Your baby never wakes up.
Impossible to understand.
It’s incredibly hard for your friends and family to assist you with your grief. Especially as I did not know how to let anyone in and I found it impossible to ask for help.
When I had counselling it took many, many weeks for me to cry. Then I began to have flashes of events that I had completely blocked out. As the counsellor guided me through those terrible times, she also began to probe for the emotions that were attached to them.
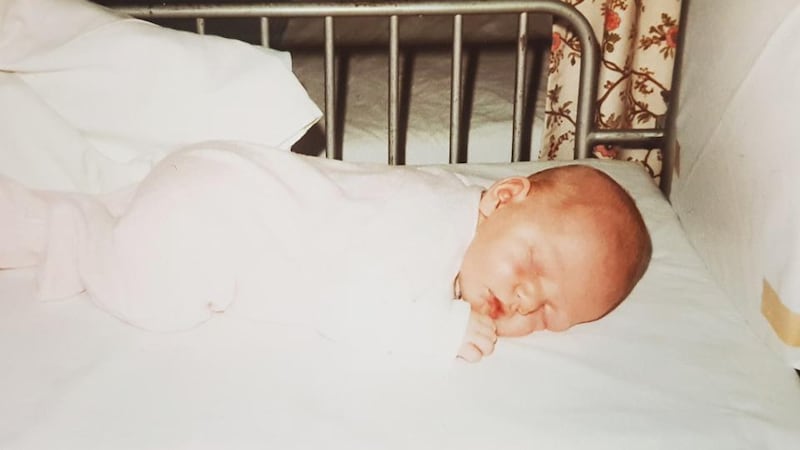
A really good illustration of the importance of dealing with trauma was when I found myself back in my bedroom on January 23rd, 1986. As I talked through the initial events the emotions also triggered. I was suddenly physically in that room with my baby. A true flashback and I was incredibly frightened in that room. Again. The vision I met was horrifying. I was terrified I was on my own with a horribly disfigured baby. Blocking and burying all of this had caused huge problems for me and earlier counselling might have avoided the layering of untreated grief and anger on top of significant trauma.
Rediscovering those minutes before I found company with my neighbour was an emptying of fear and a massive rush of empathy for myself. Of course, I did not cope – I was only 21 years of age, how in the hell would I have known how to mind myself, how to understand these extreme emotions and events.
As for that idiot who said I could have another baby...
Counselling in 2001 transported me back to that moment.
It was me.
I said it to try to lighten the bleak faces around me. I could see them all in the mirror as I did my makeup. Some of them looked shocked, but not because one of them had said it. It was me, but I had blocked this memory. It was that pivotal revelation about my level of blocking that led me to delve in as deeply as I could.
I still have gaps. Not everything dredged up. The church? The graveyard? The wake? I began to heal during the therapy process. Slowly but I never was as I would have been if this event had never happened.
Firstlight offer an understanding “walk beside you” support which is guided by the bereaved parent(s) with one-to-one counselling available when and if appropriate. They also set up group support if desired at a later stage. And their services are free.
So the numbers of deaths have decreased hugely, and the advice for parents-to-be and help for bereaved parents has improved.
But the trauma for those who experience this awfulness has probably not altered much.


















