The photo I didn’t take is the one still etched on my mind. The day before I photograph life on the Covid-19 front line in St Vincent’s University Hospital in Dublin, I meet key members of the team, including the head of the emergency department, assistant director of nursing and an emergency department consultant, when suddenly they all fall silent.
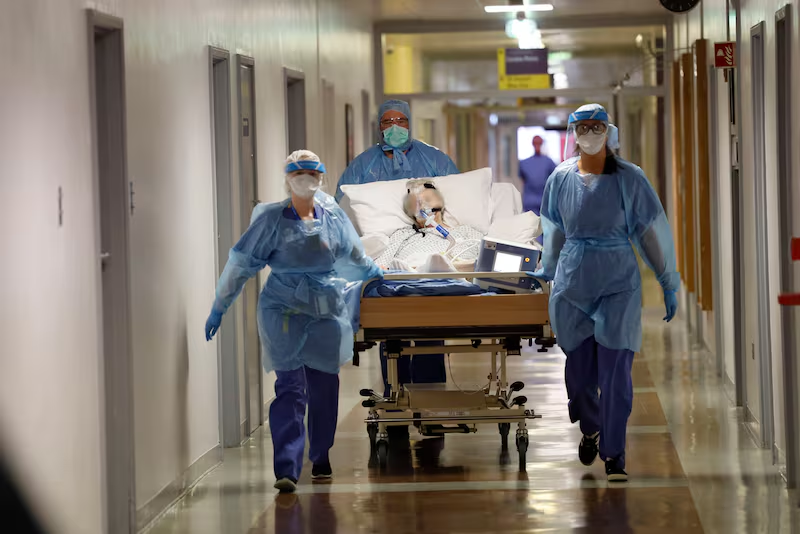
Five medical staff, in what look like spacesuits, cross the main atrium of the hospital pushing a bed with a patient who has Covid-19. The middle-aged man is fitted with a total face ventilation shield. He is upright but slumped. We stop speaking. Some of us hold our breath. For a moment it looks like a scene from a science-fiction movie. They pass and we exhale. He could be any one of us; this virus can affect anyone and respects no one.
Like most hospitals around Ireland, St Vincent's has had to transform rapidly over the past six weeks. After the first Covid-19 patients arrived at the hospital, the emergency department was divided in two. Overnight, partitions were built, offices requisitioned and converted, waiting rooms became storerooms for personal protective equipment (PPE) and equipment for the intensive care unit (ICU).
"Six weeks ago, normality as we knew it evaporated," says Prof John Ryan, head of the emergency department. As the weeks passed and the threat of a surge grew, "we built the tent outside the emergency department, but happily we have not had to use it as much as we thought. We can't relax just yet; the threat is going to exist for some time."
The visual difference between the two emergency department streams is stark. Covid-19 patients are treated by staff in full PPE. They are assessed, treated and then admitted to a special Covid-19 ward.
"It can be distressing for patients to see people wearing gowns, face masks and visors"
According to HSE figures (released at 8pm on Tuesday, April 21st), of the country's 770 confirmed cases of Covid-19 requiring treatment in acute hospitals, 61 were at St Vincent's. Thirteen patients with confirmed Covid-19 were in critical care units in the hospital. A further 28 patients were being treated at St Vincent's with suspected Covid-19 and were awaiting test results.
It's 6.20 am and there are four ambulances outside the emergency department. A paramedic in PPE escorts a patient to the Covid-19 door of the triage tent. David Menzies, consultant in emergency medicine, who is part of a community rapid response team, says "it can be distressing for patients to see people wearing gowns, face masks and visors", but he stresses that the care they receive is of the same standard as before the crisis.
For the medical personnel, working under a layer of plastic brings its own difficulties. Ambulance teams must wear full PPE while carrying out an extensive deep clean of the interior of ambulances and all equipment after carrying each patient – a physically demanding job even without the restrictions of PPE.



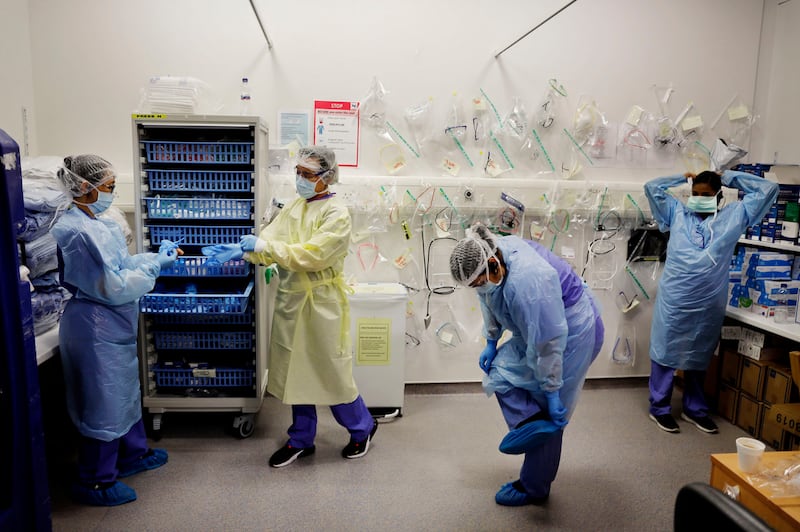
At 7.20am I meet Nessa O’Hurley, assistant director of nursing in the emergency department, and the incoming staff as they start 12-hour shifts in the Covid-19 section. They explain the strict procedures for putting on and taking off PPE, and point out which zones are considered to be clean and which are potentially contaminated. PPE can be a barrier as they seek to comfort and reassure their patients, they say. The masks hide their smiles, make it hard for patients to hear what they’re saying and the plastic is oppressively hot to work under.
Due to infection control, there are no chairs to sit on and there is no water for staff consumption allowed within the Covid-19 zone. Despite this, the atmosphere is convivial, and there is no sense they’re about to enter a Covid-19 space.
The 8am Covid team meeting, attended by consultants, nursing, bed management, infection prevention and control, and other relevant staff, takes place in the main lecture hall. The staff socially distance across the hall, their blue scrubs standing out against the vivid red chairs as the discussion focuses on the effectiveness of various treatments against the virus, a run-through of patients admitted on the previous shift and any updates relevant to Covid-19 international research trials. Throughout the hospital, social distancing continues: tables are limited to two people in the canteen, and all chairs have been decommissioned in public spaces.
No visits to Covid-19 wards are allowed. At 11.15am I meet Louise Morgan, principal medical social worker, who explains the newly established support line for Covid-19 patients and their relatives. Morgan's team ensures information on a patient's progress is passed to one designated relative, and they also provide virtual visiting via video calls on iPads.
Bags of essential items for patients can be dropped to the hospital, but any item entering a Covid-19 space must be quarantined for seven days before it can come out again. Even sheets of paper must be quarantined after leaving a Covid-19 ward, so all patients’ notes must remain outside.
A buddy system is in place so that tired staff make no mistakes in removing their protective equipment
Karen Screene, clinical nurse manager of St Monica's Ward, explains the one-way system for entering and exiting Covid-19 wards. PPE is put on within the initial clean zone, which includes the doctor's office. Proceeding past this area is only allowed in full PPE. When staff are exiting the ward, they remove their PPE just inside the exit door. A buddy system is in place so that tired staff make no mistakes in removing their protective equipment in order to prevent transmission of the virus from the outer surface of the PPE.
The exit door is then opened from the outside, to prevent contact with the inner door, ensuring a clean exit from the ward.
After she puts on her PPE, and before disappearing into the Covid-19 ward, healthcare assistant Lorena Domingo calls out to us: "We're going now, we're going to the war."

According to Screene, where possible, special arrangements for visits are made for relatives in end-of-life situations, and religious beliefs are catered for by the hospital’s chaplaincy service, “within the guidelines and restrictions of the HSE”. Chaplains have been trained in infection prevention and control, and attend to the needs of patients using PPE.
It’s a misconception that Covid-19 patients are all elderly, Screene says. People “from their 20s up to 90s have been in here”. There is no predictable pattern to the disease: “Some people come in and can be very independent [throughout their stay], others walk in the door and become sick very quickly.”
Just before midday, patient Tommy Doran (58) from Blackrock in Dublin speaks to me from his bed on St Monica's ward using my iPhone, which is sealed in a plastic bag and is subsequently disinfected three times before I can reclaim it.
Prior to his positive Covid-19 test result he didn’t have major symptoms, but all that changed. Breathlessly, he describes his symptoms of severe headaches, high temperatures, shakes and shivers.
“No cough or respiratory problem, but at night-time I found it hard to my catch my breath and I also had aches and pains in my bones.
“Each day you think that you are going to be okay, but then in the afternoon you start to get the shivers again, and start coughing and the temperature goes up. It’s strange coming into a hospital and not seeing visitors, everybody is in PPE and it’s very quiet.”
(Doran is subsequently discharged and is recovering well at home.)
The transfer of Covid-19 patients within the hospital is a process akin to a military manoeuvre, involving masked security guards, alongside porters, medical and cleaning staff in full PPE. At 12.30pm I meet clinical nurse manager Aoife Waldron, who is the non-invasive ventilation co-ordinator that day. She describes the transfer process: "Security staff walk ahead of the transport team, clearing the route of all obstacles and people. The cleaning staff follow behind, deep-cleaning the area and the surfaces in confined spaces, such as lifts."
Anything the HSE has allocated to us, we are taking as a bonus. It's the existing supply chain from our main suppliers which is keeping us going
Security officer John Sheridan tells me of a recent day where 57 patient transports took place within the hospital, and his personal pedometer recorded 22,000 steps.
At 1.16pm, and from a distance, I observe a coffin being removed by funeral directors from the morgue to their waiting van. It is a lonely process, with none of the family that would usually be present.
Just after 2pm, I visit the procurement team in the hospital basement, passing the clinical engineering department, where testing of high-spec cardiac monitors and ventilators from China is under way.
I imagine the Defence Forces delivering truckloads of Chinese PPE to the hospital, but according to head of procurement Michael Sullivan "anything the HSE has allocated to us, we are taking as a bonus. It's the existing supply chain from our main suppliers which is keeping us going."
“There has been a lot of innovation from small to medium-sized Irish companies, who have been able to help supply us, like a window blind manufacturer in Derry, Bloc Blinds, who are now producing 12,000 face visors per hour and supplying at cost.”
The hospital's regular suppliers have maintained pricing and supply chains and allowed them to increase volume, he says. "We've been able to use the HSE's supplies as a buffer, but so far we haven't run short on anything. We have been able to help some of the other hospitals [within the Ireland East Hospital Group, which includes the Mater and National Maternity Hospital] when they run short."
Supply chain manager Marcella Coyne says: "Our existing suppliers could sell to any other company at a much higher price, particularly isolation gowns – where we're seeing massive requests on price – but they've kept them at the pre-existing price and kept us in supply."
“One of the things we’re seeing,” O’Sullivan adds “is a huge amount of opportunists out there – basically, people trying to make a quick buck.”
At 3.02pm I visit the staff Covid-19 test centre. Since mid-March, the hospital has offered Covid-19 testing to any of its 3,000 staff who have become symptomatic, according to manager Breege Screene. The staff test centre, with two testing rooms, is open seven days a week and conducts up to 40 tests a day. Staff are offered a test on the day they experience symptoms, and results are usually back within 24-48 hours. Screene says: "Staff are nervous. We have sadly heard of deaths in the health service both here in Ireland and in other countries, and that is worrying for staff." The hospital would not disclose the number of staff it has tested, nor the number of confirmed staff cases of Covid-19.
At 3.33pm clinical psychologist Paul D’Alton tells me that due to Covid-19, traditional face-to-face patient psychological assessments and therapy are now being done online and over the phone. This has given the department the capacity to offer additional supports to staff, known as “psychological first aid”. “Due to social distancing there are much less ‘How’s it going?’ type informal corridor conversations.” These are the social supports that normally buffer people against stress and anxiety, he says.
A face mask covers her smile, but there is joy in her eyes as she throws her hands in the air and walks towards her two sons
According to Angela Smith, director of quality and patient safety, some staff have found themselves "self-distancing from family members, moving into their own bedroom … withholding hugs from partners and little ones, not wanting to have brought [Covid-19] home unintentionally."
At 5.05pm I meet paramedic Keith Butler, a member of the ambulance staff. The last time he saw his mother, Mary, was 2½ weeks earlier, when he drove her from Ballinteer to the St Vincent's emergency department in his ambulance. She had recently returned from Spain and had started to show symptoms of Covid-19. Her condition worsened and she spent four days in ICU. She is now well again, and I meet Keith and his brother Simon as they wait outside the hospital for her discharge. Eventually she emerges from the building. A face mask covers her smile, but there is joy in her eyes as she throws her hands in the air and walks towards her two sons.
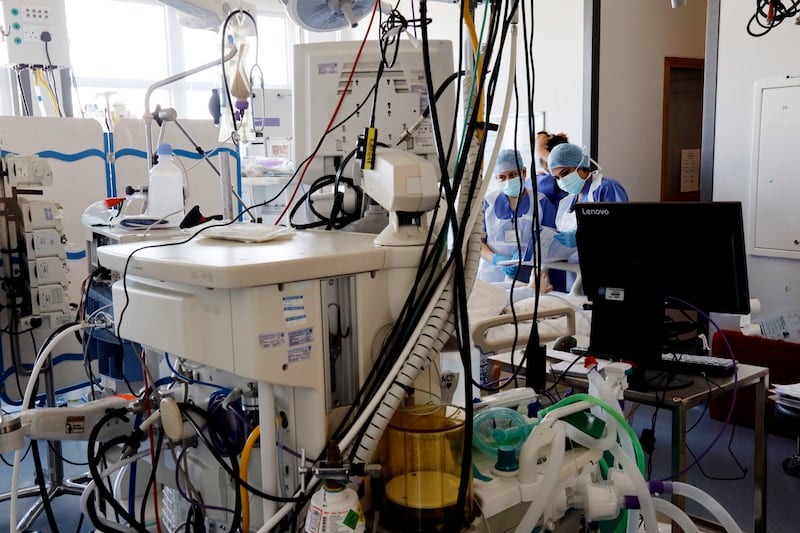
Since March, departments across the hospital have been divided into Covid-19 and non-Covid sections. That segregation was especially crucial in ICU.
Head of ICU Michael O’Dwyer shows me some operating theatres that have been repurposed to hold two ICU beds each, for patients on ventilators attached to anaesthesia machines. They are currently being used for non-Covid-19 patients.
Similarly the post-anaesthetic care unit has been repurposed and is standing by, ready for Covid-19 patient ICU use. There are plans to develop further surge capacity, O’Dwyer says, and routine non-Covid-19 services such as oncology, haematology and some surgery have been moved to St Vincent’s Private Hospital in line with the State deal to lease private hospitals for HSE use during the Covid-19 crisis.
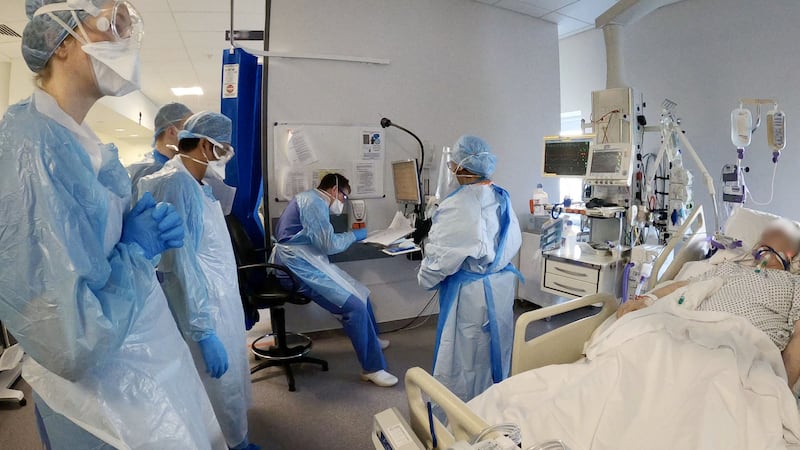
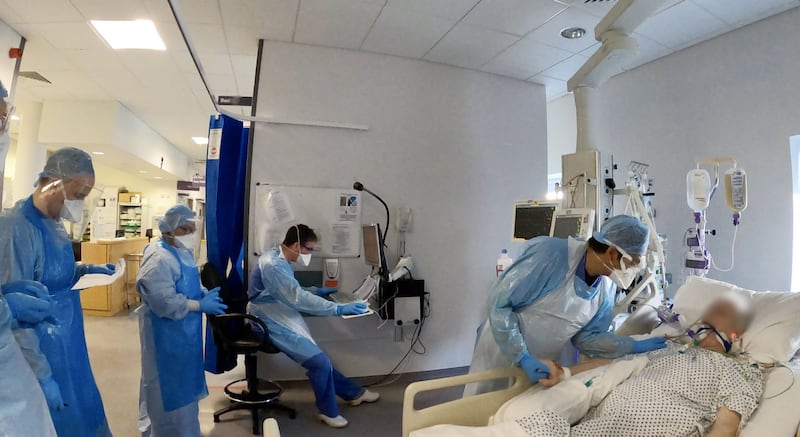
No non-essential medical staff are allowed to enter a Covid-19 ICU. So I wait outside, while ICU staff wear a small camera to show us what they see on a daily basis. The ICU is where the battle for life is at its most intense, and these photographs show the people on the front line and the personal risk they take every day. It may be disturbing for us to see people fighting for their lives, but it is comforting to see there are teams of people fighting on their behalf to beat the virus, too. And it’s heartening to know impossible choices as to who gets a ventilator have not had to be made, yet.
Thank you to all the staff at St Vincent’s University Hospital, including Angela Smyth, director of quality and patient safety, and Ina Foley, head of communications, for their assistance with this report



















