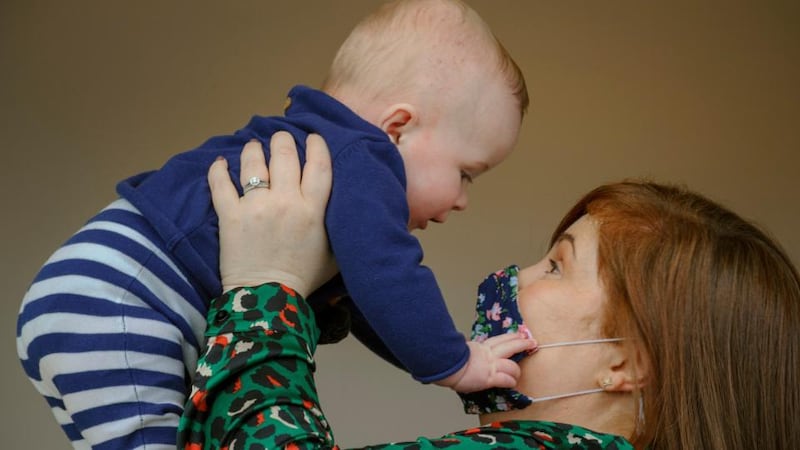
Úna Caroline Haran was born the day the World Health Organisation (WHO) declared a pandemic. She came into the world weighing 3.5kg at 7.47pm on March 11th, just hours after Dr Tedros Adhanom Ghebreyesus called for countries to take "urgent and aggressive action" against coronavirus.
“Ready your hospitals,” the WHO’s director general warned.
Earlier that morning, as her mother, Ruth Cullinane's labour began, Ireland was still trying to cling to the last threads of normality. There had been 10 cases of Covid-19 the previous day, and the morning's news bulletins were full of speculation schools might have to close.
But it was day two of Cheltenham, the public were being reassured that visitor bans at nursing homes were unnecessary, and life seemed like it might be able to carry on without much interruption.
Inside the Rotunda, however, the virus was already shaping the course of Úna’s first hours and days of life. “They decided no partners were allowed into the hospital unless you were in labour,” Cullinane recalls. So while Úna’s father, Fergal, was there for her birth, he had to leave once Cullinane and the baby moved to the post-labour ward.
Over the next 24 hours, “it became clear that the hospital was taking it very seriously. The security staff were getting a lot of grief downstairs from people who were turning up and wanting to come in. I just wanted to get out of there as quickly as I could.”
By Friday, the postnatal ward was emptying out, but the atmosphere was still more of novelty and uncertainty than fear. As Cullinane packed up to go home, “we thought it was just going to last a few weeks.”

Across the city in the National Maternity Hospital at Holles Street, the master of the hospital Dr Shane Higgins and his team, including director of midwifery and nursing, Mary Brosnan, were confronted with the issue of what to do with "a 19th century hospital that isn't fit for social distancing," says Brosnan.
In the space a couple of weeks, recalls Higgins, the hospital’s engineering department and the building team “had to create a space whereby we could look after patients who were either suspected or confirmed cases [of Covid]. So we converted three of our delivery rooms into negative pressure ventilation rooms”, along with the whole gynaecological ward, and rooms in the emergency department. “It meant we could look after 22 patients who were suspected or confirmed [Covid positive], while maintaining a very normal working environment around them.”
The video footage coming out of Italy sent waves of trepidation rolling across the health sector, including the maternity services. "For the first couple of months, I would have noticed a huge amount of fear within the staff that they were going to either contract Covid or pass it on to somebody else or bring it home to a family member," says Brosnan.
Higgins recalls that “we were looking to acquire ventilators from any source possible, so that if we had to start ventilating patients, we could do it. We were training junior doctors in obstetrics to look after machines, so that if patients were being ventilated and we were running low on staff, they could man them. We were just waiting for that tsunami to hit us.”
“We didn’t have a chance to stop for a couple of months and plan it. One morning we woke up in early March, and we were in the middle of the pandemic. We didn’t get a chance to just say, ‘Okay, now we’re going to suspend all births and let us plan this properly.’ So we just muddled along and managed very well,” says Brosnan.
The traffic in and out of the hospital had be reduced dramatically, which meant immediate severe restrictions on visiting. “At one point in time, we had no partner visiting apart from the birth of the baby,” says Higgins.
“We weren’t attempting to be draconian and punitive. We just wanted to make sure that patients were safe. They were vulnerable, they were pregnant, their immunity was compromised. We didn’t know what the risks were to newborn babies at that time. We had to look after them, and make sure that the staff who were looking after them were able to come to work.”
In the first two or three months, Brosnan says, “women were desperately keen to go home early with the fear of contracting the virus in hospital. The length of stay dropped dramatically from March till about June. Women were going home within the first day of having normal birth and on the third day after a c-section.”
'I haven't seen my mother in these last few weeks. I haven't seen my sister. My friends haven't met my baby, because we're being extra careful with my heart condition'
Due to staffing shortages and other issues – there was one day early on when 107 staff were out because they had come into contact with the virus – the rate of inductions rose “slightly” during the height of the restrictions, Higgins says, “but that trend hasn’t continued.”
In the event, the tsunami “thankfully didn’t hit us,” says Higgins. In all, 38 patients of the hospital have so far tested positive. “And of 28 babies born to them – with the others still pregnant – all those babies went home well, with no evidence of any infection,” he says.
Their pride in what staff managed to achieve is immense. But they acknowledge the necessity to prioritise the safety of staff and patients did not come without a significant price. Here, as in many of the other 19 maternity hospitals across the country, women who have been pregnant since March have had to attend most of their appointments alone, without the support of a partner, other than when an exception is made for compassionate reasons.
“We’re doing everything we can to try and get dads and partners back as much a part of this as they can be,” says Higgins.
Visiting guidelines have been eased so that “our current visiting guidelines are that a birth partner is allowed in for the entirety of labour and delivery. Partners are allowed in for a minimum of two hours every day the mum is in hospital. And then there’s unrestricted access to babies that are in the nursery from both parents.” Some aspects of the changes – the introduction of telemedicine for routine appointments – have been positive and will be maintained post-pandemic.
Partners of expectant mothers attending the Rotunda hospital have been permitted to attend the 20 week anomaly scan for the past couple of months. By Christmas, he hopes that partners will be able to come to the 20 week anomaly scan in Holles Street too. (This week, the HSE asked maternity hospitals around the country to allow this to happen.) “We’re acutely aware of how upsetting and distressing it is for partners not to be able to come in.”
The hospital is expecting to become slightly busier after Christmas, with bookings up slightly on previous years. But it’s too early, says Higgins, to predict any kind of pandemic baby boom.
He feels particularly sorry for first-time parents in all of this. “I think they’re the ones who are probably suffering the most. The dad sitting in the car was outside waiting for their partners to come in and have their antenatal appointments or to come in and have their scans. And I just I do I feel enormously sorry for them.”
Among the women in hospital during the first lockdown, most of them alone as they prepared for delivery, there was "a weird sense of camaraderie. You'd share a look across the corridor, or you'd wave, like 'we're all in this together'. We didn't even have to talk. We were all in it together," says Ciara Clancy who gave birth to her first child, Iarla, in April.
She has a heart condition, and so was categorised as high risk, and was scheduled to have a c-section. Towards the end, the baby stopped growing, which meant scans every two to three days – all of them on her own, while her husband Declan waited in the car. “It was horrible. Declan just sat out in the carpark for the two or three hours, with his mind going everywhere.”
After Iarla was born, they spent an hour and a half together as a family, before Declan had to leave. Iarla was four days old before he saw his Dad again, at the door of the hospital.
Declan “missed out on so much. At the time, he didn’t tell me how he felt, because he didn’t want to upset me, but he says now it was the hardest four days of his life. Those first few days of bonding, and cuddles, and getting to know your baby are huge. I sent thousands of photos in those four days.”
Since then, she says, “it’s been so lonely. I’ve got great friends and family who are on the end of the phone no matter what, but like, I haven’t seen my mother in these last few weeks. I haven’t seen my sister. My friends haven’t met my baby, because we’re being extra careful with my heart condition.”
Clancy has had two appointments with public health nurses – one at two weeks, and one at three months. There are no clinics or breastfeeding groups where she can go along and have Iarla weighed. “Other than the doctor for vaccines, nobody has checked up on my baby medical-wise. My next appointment with the public health nurse is not until January. That means it will be nearly six and a half months before anyone’s come to weigh my child.”
Clancy regards herself as “a very resilient person”. Even so, “there’s been so many times where I’ve cried for no reason. It’s not just baby blues – it’s not even wanting to get dressed or get up and do something, because you can’t do anything, you can’t go anywhere. So you’re just in a slump. I know everybody is going through the pandemic, but it’s a bit more heightened with a new baby. You’re at your most vulnerable as a new mother, as a first time mother. I don’t want to sound dramatic, but I think a lot of women will suffer PTSD for what they’ve gone through in the future. When we actually sit down and think about what we’ve been through, it’s going to affect us, it’s going to hurt.”
The first year in a new baby's life can be an isolating and anxious time for the mother, under even the best of circumstances. This year, the loneliness has been particularly acute. Ruth Cullinane, who is a junior doctor specialising in psychiatry, is even more acutely conscious of the impact on women's mental health now.
What she missed most was “support from family and peer support. You do feel really isolated. You’re in your own head all the time. You’re not getting a break from that, because you’re not meeting anyone else and you’re not socialising. I found the first few months really tough.”

The quiet months at home following Úna’s birth gave Cullinane a chance to bond with the baby, but not having face-to-face support was hard. She attended a few breastfeeding groups and saw a lactation consultant via Zoom, but it was challenging.
We normally would see about 70 referrals a week to the perinatal psychiatrist. We would now probably see about 100 referrals a week, so it is quite significantly up
“It’s not the same. You need that human touch . . . It’s definitely been a really, really stressful time, but I’m conscious as well, that other people have had it way worse than me.”
These issues are not just facing Irish women: researchers are noting a global increase in maternal mental health difficulties during the pandemic. Dr Diego Wyszynski is the executive director of the International Registry of Coronavirus Exposure in Pregnancy, a study involving 7,500 women in 65 countries being carried out in co-operation with Harvard University's School of Public Health and his own online resource, Pregistry.
“The results have been thus far pretty outstanding, pretty incredible,” he says. When anxiety and depression are taken together, about 70 per cent of women showed evidence of one or the other. “Before the pandemic, it would be between 10 per cent and 15 per cent. Approximately 40 per cent of the population of pregnant and recently pregnant women had clinical symptoms of post-traumatic stress. Over 50 per cent felt lonely and isolated.”
In the responses to the survey, “many women feel that during the pandemic, they are really lonely . . . This increases the amount of anxiety they feel. They think, am I going to give birth on my own? Is my partner going to be allowed while I’m giving birth? Am I going to be able to see my parents, and my parents to see their grandchild?”
The absence of a partner at antenatal appointments is one of the major stressors, he says. “The reason why hospitals want to keep those loved ones separate is simply because they are trying to prevent the possibility of infection to the people who are in the hospital. However, we know that the mental health consequences of that separation can be, in some cases, devastating. Pregnant women sometimes have been in isolation or in lockdown for weeks, some cases for months. They have been lonely, they [may] have developed clinical symptoms of depression, and now they’re being told that their family member or their loved one cannot be with them,” he says.
It is, he says, “a pandemic within a pandemic.”
At Holles Street, “we definitely have noticed an increase in the numbers of referrals to the perinatal mental health service,” says Brosnan.
“We normally would see about 70 referrals a week to the perinatal psychiatrist. We would now probably see about 100 referrals a week, so it is quite significantly up.”
Some of this is due to “normal anxiety”, the entirely predictable response to these uncertain times. “Then there are the women who do suffer from underlying mental health issues and psychiatric conditions. And they definitely would need more support during their pregnancy. I think for the minority of women who struggled with their mental health, their anxiety levels have been really heightened.”
However, there has been some positive fallout too, Brosnan suggests. “I think for the majority of women, they may have had a more relaxed pregnancy. They may have had their partner working from home; they might not have had the same social pressures to be having the baby shower and all the things that women end up getting consumed within the last couple of months . . . I think if I were to sum it up, I’d say they were extraordinary times.”

The staff in the hospital learned a lot about their own resilience and what they were capable of. “For me, the vast majority of the last nine months have been really good times.”
By the time Fiona Devine went into labour with her second daughter Aoibh, who was born on April 29th, the country was in deep lockdown. In many hospitals, partners were no longer allowed to accompany expectant mothers to scans, or even for the early stages of inductions. "I had to go in on my own to be induced. It was awful."
She passed the time taking photos and sending them to her husband, who was waiting in the car outside. “Once I went into the labour suite, I called him, and he was able to come in, so he was there for the birth. But then you say goodbye again, and that’s it.”
Shortly after her birth, Aoibh was diagnosed with hip dysplasia. Fiona’s husband had already gone home, so she was alone when she got the news. “He got an awful call from me, crying my eyes out.”
Back home with a toddler and a newborn, she found she really missed the support she enjoyed during her first pregnancy. “For my first girl, I did all the baby yoga, breastfeeding support groups – I met women through that, there were a group of four or five of us that all had babies around the same time.”
This time around, there have been no classes, no support groups, no coffees with friends. When she does have an appointment, “everyone has a mask on, and it’s in and out. I have seen my in-laws only twice in the last six months . . . I usually work full time, so I am sad that the time has been spent just surviving rather than thriving.”
The result for her has been that everything “just feels so intense. It feels like you’re on the edge a lot more. Sometimes your mood can be great, but it doesn’t take a lot to tip you over.

“I would definitely consider myself to have pretty strong mental health, but it has been tested. You’re isolated from people physically but mentally as well. Everything that’s going on in other people’s lives is so far removed. I don’t want to use the word depression, it’s like a lack of life. It’s like here we are again, day 5,675. It’s just monotony and survival.”
In common with other women who spoke to The Irish Times, Devine has noticed a big difference in post-birth services, compared to when she had her first daughter.
This was highlighted in a survey carried out last February and March of 3,200 women, 85 per cent of whom reported either a good or very good experience of maternity care. However 15 per cent did not have a good experience, and the period after birth was an area found to be needing improvement. During the pandemic, these services have contracted further, as public health nurses have been redeployed to deal with Covid-19. The HSE said recently that it didn’t know when checks for all children would resume, but that children who are a “priority” are still being examined.
Devine had a single visit from the public health nurse during Aoibh’s first week. “And then that was it. Nothing. I rang them to see when they were coming back, and they said they weren’t doing any regular appointments, but if there’s anything you’re concerned about, you can give them a call. That’s maybe okay for me who has been through it already, but I’d worry they’re going to miss out on things with other people. You need somebody external to check on development.”
Corrinne Hasson and her wife Susan Tierney had their first baby, Eleanor Rose Tierney – they call her Ellie – in the Coombe as Ireland was entering the second Level 5 lockdown.
It was a complicated pregnancy: Ellie was conceived through IVF and Hasson discovered she was suffering from fibroids early on, a very painful condition that meant frequent check-ups, all of them alone. There were times when this was intensely difficult – not just because of what she was going through herself, but because of what she saw other women experiencing.
“I was there one day whenever a lady had gotten a pelvic exam and was told that her baby probably wouldn’t survive, and she didn’t have her partner with her. She was there on her own. I wanted to give her a hug, but you couldn’t do that. It was so hard. There was loads of people getting bad news. I was going through all these tests and exams, and Susan wasn’t there for any of it. I was worried that she wouldn’t be part of any of it. I think that’s a worry with a same sex couple” – ensuring that both will get the chance to bond with the baby.
“So I paid for a private scan with one of the clinics, just because I wanted her to see the baby and hear the heartbeat. They’d say in the hospital, we’ll allow visitors in soon. But Susan isn’t a visitor. She’s our baby’s mother.”
'There have been positives, and I do try to focus on them'
As part of a same sex marriage, she found she had to keep explaining her circumstances to the staff. “Every single person said, ‘Oh it’s a shame your husband can’t be here’. If Susan had been there, they would have seen I was married to a woman. There’s still a lot of assumptions made. Normally things like that don’t bother me” but it underlined how alone she was.
Tierney was there for Ellie’s birth, something they’re both very grateful for. “It was so busy at that time. A couple of women ended up giving birth on the ward the night before I had Ellie, and their partners didn’t make it in at all.”
Back home, with Tierney back at work, Hasson is find breastfeeding hard. “I had no antenatal classes or anything. I went to the consultant every three weeks, go a scan, and that was it. There was no talk of whether I’d like to see a midwife to talk about breastfeeding. So I’ve had to depend on neighbours and some of Susan’s colleagues for hints and tips. I didn’t even know that your milk doesn’t come in for a few days. I remember saying to one of the midwives, ‘She’s trying to feed but there doesn’t seem to be anything there’.”
However, she has had good support from her local public health nurses, one of whom is a lactation consultant. “Ellie had lost a little weight by the first appointment, so they came out again. If she hadn’t lost that bit of weight though, that would have been it,” she says.
Both sets of grandparents have met Ellie only once, in the back garden, during a visit that lasted 15 minutes. “It was nearly worse that they were here. I found it really tough. I just wanted to give her to my mum, but we couldn’t.”
So far, “Ellie has only ever been held by myself or Susan.”
But she feels lucky to live where she does in Dunboyne, Co Meath, where her community has rallied round. "The day after we came home from hospital, our neighbours' daughters got loads of chalk and drew a big massive picture on the road. 'Welcome home, baby Ellie', with a picture of a baby and two women."
Jessica Keith, who is due her first baby next April, looked at all of the restrictions on maternity services during a pandemic and has decided to opt for a home birth instead.
“The first thing I did was start to reach out to other organisations like doula and midwife organisations to learn more about how to figure out what my options are. And through a conversation with a doula she mentioned the prospect of a home birth. Given the circumstances that we’re in, it made a lot of sense to me plan on this route, while understanding that the circumstances may change. For now, that’s the path we’re on.”
She attends the Coombe for scans, where she was advised to go through the National Home Birth scheme operated by the HSE, but she has decided to engage a private midwife.
Her mental health has been good during her pregnancy so far, and she has been able to cocoon away with her husband. But this is still a very strange time to be pregnant.
“You’re in the hospital with women who are pregnant to varying degrees, who are receiving varying degrees of news, who all have masks on and cannot really interact with one another. There’s this feeling in the back of your head, like, please don’t come near me, please don’t come near me. And you’re all going through a very sensitive process on your own. The scary part is what if something is wrong and I’m by myself?”
Asked to put words on the experience of becoming pregnant or giving birth during a pandemic, it’s striking how several of the women interviewed for this article reach for a version of the same form of words. Lots of them mention how lovely it has been to have their partner working remotely. But they feel lonely and isolated, and miss their families and friends. New mothers are experiencing a lot of uncertainty, and second-guessing themselves. At home with a new baby, without even outings to the supermarket feeling unnecessarily risky for many, the days can be very long.
Overall, says Corinne Hasson, "it's been the best and the toughest thing that I've ever done. We were so delighted to find out that we were pregnant, and then in a few weeks, Covid was here. It was tough to be pregnant and to not be able to see your family. Or to able to really see friends. So as much as it's been great, it has been a bit of a lonely time."
For Ciara Clancy, “There have been positives, and I do try to focus on them. It has been lovely. At the same time, I’ve never been more alone, but with my partner, if that makes sense. You need real-life support, you need your family, you need your friends. I don’t think anyone understands if they’re not walking in your shoes. Iarla has been such a light for us, but it’s been a struggle. We’ve both struggled. We feel so isolated, even though we’ve got fantastic support on the phone. It’s been the best and the worst time.”
















