Psoriasis is a chronic inflammatory skin disease that affects up to 120,000 people in Ireland.
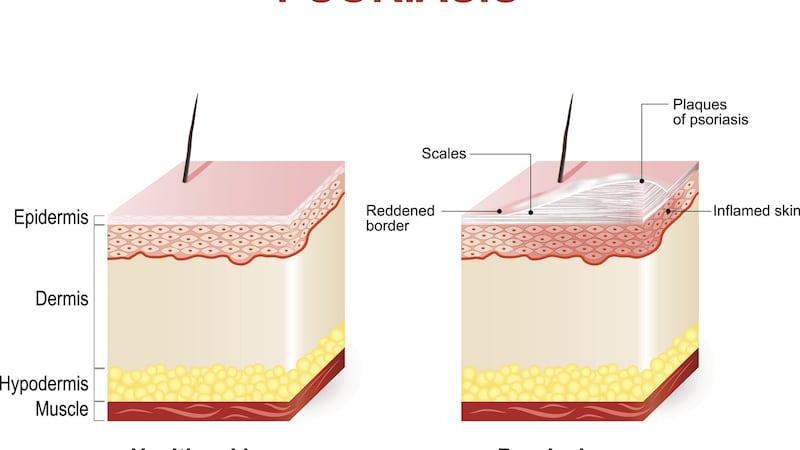
Abnormalities of the immune system in the skin cause the top layer of the skin (epidermis) to grow faster than normal, become red, scaly, itchy and painful – 20 per cent of patients have severe disease and require specialist care.
Psoriasis has been recognised since ancient times and the word is derived from psora the Greek term for itch. It was not distinguished from leprosy until the early 1800s. Indeed, many of those with leprosy mentioned in the bible may have had psoriasis.
Psoriasis causes significant suffering for patients, with impairment in the quality of lives of its sufferers larger than many other chronic diseases and even some cancers. "Psoriasis does not kill but destroys lives," stated Thomas Fitzpatrick, professor of dermatology at Harvard in the 1970s.
Destroyed lives
More recent studies support the destroyed lives concept, but have also shown that patients with severe disease die at a younger age (approximately five years younger) from premature cardiovascular disease. In addition, 30 per cent of patients with psoriasis are more likely to develop an immune-mediated arthritis similar to rheumatoid arthritis which can cause painful, swollen joints and disability.
The good news is that huge progress has been made in psoriasis treatment over the last 15 years.
Highly effective therapies with low risks of serious side-effects have revolutionised patient care. There are now 19 licensed treatments for moderate to severe psoriasis available in Ireland. No one treatment suits all patients, but, in 2019, there are treatments available that can clear or nearly clear almost all patients – even those with the most severe disease. Most patients will require continuous treatment to maintain control of their disease similar to patients with asthma or arthritis, but the evidence is clear, that no patient should have to live with severe psoriasis in Ireland today.
Despite these highly effective therapies available, we still meet patients whose lives have been ruined by this disease. Psoriasis affects all aspects of patients’ lives when severe. It affects education, career choices, relationships and past-times, (swimming pools are a nightmare for people with psoriasis). Patients with severe psoriasis are more likely to have depression, suffer feelings of stigmatisation and contemplate suicide. Younger people suffer most.
Specialist care
The challenge, for the future, concerns access to specialist dermatologist care for these patients. Waiting lists for dermatology care are increasing and are more than three years in many centres. This is due to inadequate consultant numbers in public hospitals, inadequate resourcing of these departments in terms of specialist nurses, clerical staff and IT support, and an exponential rise in referrals to dermatology departments in recent years. These funding issues are seen across all specialties in Ireland and are unlikely to change.
We need to at least have an honest debate about resourcing a system that allows earlier access for patients with inflammatory skin disease to appropriate services so that they can obtain effective therapies and care. General practitioners are not resourced nor trained to deal with these patients.
The concept that services are cheaper and more cost-effective when delivered in a primary care setting is not true for dermatology and studies have shown that early access to specialist dermatology care is cheaper than having patients with inflammatory skin diseases managed in primary care. Dermatology as a specialty is not expensive in terms of in-patient hospital care and is a very cost-effective way of improving the lives of many patients with psoriasis and other inflammatory skin diseases.
Our hope for the future is that all patients with severe psoriasis in Ireland can access appropriately the highly effective therapies that are available in 2019.
– Prof Brian Kirby is a consultant dermatologist at St Vincent's University Hospital and full clinical professor at the Charles Institute of Dermatology, University College Dublin. This Saturday, he is co-organising the annual Psoriasis Shout Out at Dundrum Town Centre. See Health Board









