The impact of the Troubles on the mental health of those who lived through it was often less visible or understood during the conflict than the more obvious physical injuries.
However, as some of the stigma which previously stilted conversations around mental health has faded, it is an issue which is slowly coming out into the open, as Northern Ireland grapples with its long-lasting psychological scars.
A 2011 study by Ulster University found that Northern Ireland has the highest recorded rate of post-traumatic stress disorder of any studied country in the world.
The region also continues to have the highest suicide rate in the UK or Ireland, with about 18 suicides per 100,000 people in the population compared with nine suicides in England or eight in the Republic of Ireland, according to official government figures.
Use of diazepam, medication often prescribed to treat depression or anxiety, in Northern Ireland vastly outstrips its use in other parts of the UK, with people in the region being five times more likely to be prescribed it than people living in England.
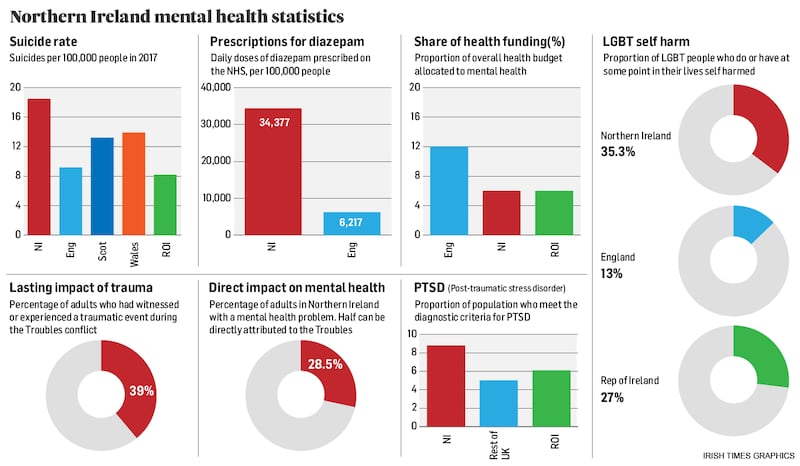
Despite this, public spending on mental health is far lower in Northern Ireland than the rest of the UK. In England, some 12 per cent of the health budget is spent on mental health, compared with just 6 per cent in Northern Ireland.
Siobhán O’Neill, an academic at Ulster University, says service provision for people who need support is often sub par.
“There is no overarching mental health strategy to drive provision in a systematic manner. There are huge waiting lists for services, and the provision of early intervention services for young people is particularly poor,” she says. “People in Northern Ireland wait longer for treatment for mental illness and their conditions invariably worsen.”
She says this has been further hampered by the ongoing lack of a government at Stormont, which has not sat since January 2017, as in the absence of ministerial approval, a much-anticipated suicide prevention scheme has been put on hold.
Survivor
Jonathan Ganesh is a survivor of the 1996 IRA bombing in London’s Docklands, in which two people were killed and hundreds more were injured. He now runs the Docklands Victims Association to support those affected and says several of the injured have since taken their own lives due to the trauma they suffered.
“A vast number of victims have developed severe PTSD or other mental health disorders. We have been very concerned with the number of victims that have taken their own lives and others that have been sectioned under the Mental Health Act.”
There was undoubtedly a domino impact of devastation
Ganesh feels the UK government has failed to acknowledge how common trauma is for survivors of atrocities and instead considers it to be “a private matter which must be resolved by the victims themselves” rather than an issue which would merit specific strategic government support.
“Support provided by the Victims Survivors Service in Northern Ireland is totally inadequate as it does not address the needs of the victims and their families with mental health disorders. This inadequate care has aggravated conditions such as PTSD and other mental health disorders as a consequence”. He adds that many survivors also continue to feel “stigma” about accessing support services related to mental health.
Ernie Wilson, whose son James died by suicide in 1989 after being badly traumatised by an IRA attack, began campaigning earlier this year for an official register of Troubles-related suicides to be created in a bid to highlight the issue.
Kenny Donaldson, director of services at the South East Fermanagh Foundation which supports victims of Troubles-related violence, is among those who have backed Wilson’s call.
Donaldson says that of 62 deaths in the conflict in which his charity has supported witnesses or affected family members, he is aware of 14 suicides “directly” connected to the trauma of those murders. “There was undoubtedly a domino impact of devastation. The true number of lives stolen as a result of ‘the Troubles’ is several times greater than the [official death toll],” he says.
“PTSD, profuse anxiety, chronic depression are amongst conditions experienced and there have in fact been a number of suicides down the years by surviving family members and/or those who were themselves directly physically or psychologically injured.”
Donaldson says that many survivors and victims’ families who try to find help can be surprised to find the services they seek aren’t there: “The experience down the years is that there is a lack of acute healthcare support for those suffering mental health-related trauma issues.”
Unaddressed anxiety
Meanwhile, O’Neill says the conflict-related trauma continues to affect the generation born after the Troubles ended, as they can “inherit” unaddressed anxiety and depression from their older relatives.
“Research shows that mental illness and trauma exposure in parents and grandparents increases the risk of mental illness in the next generation, mainly through the impact on parenting behaviour, and economic factors,” she says. “We now have a generation of young people who have been raised in environments and families who have had these difficulties, and in communities who suffer the legacy of the Troubles.”
Research has also indicated that trauma can be transmitted in pregnancy, also impacting on new generations, she says. “There is emerging evidence of a possible biological trauma transmission whereby a parent’s response to trauma alters the genetic factors that influence a child’s stress reactivity, which in turn can influence the likelihood of mental illness in response to stress.”
She says that to break the cycle, urgent intervention is needed to address mental health issues in communities most directly affected by the conflict.
But O’Neill is not optimistic of this happening, saying she doesn’t have confidence in the level of interest or awareness Northern Ireland’s politicians have about the issue.
“A top-down approach would drive the sort of systematic change and the funding of evidence-based practices that are shown to reduce mental illness and suicide rates in other places. However, I remain pessimistic about the commitment of our political leaders in relation to mental health.”











