Information and arguments surrounding vaccinations for teenagers and adults seem to be everywhere these days. Two in particular – the HPV vaccine for teenage girls and the flu vaccine for adults – are continuously mentioned in the media, on posters in the chemist and in online forums, while the pertussis vaccine for pregnant women is increasingly a part of public discourse.
The CervicalCheck scandal, with cervical cancer’s link to human papillomavirus (HPV), the late Emma Mhic Mhathúna’s participation in the Health Service Executive’s campaign for the vaccine and Minister for Health Simon Harris’s announcement that money from the new budget will help fund gender-neutral vaccination, have all brought discussions regarding the HPV vaccine to the fore.
Meanwhile, the uptake for the annual flu vaccines has increased over the years, and the onset of the colder weather means that the public are once again encouraged to get it.

A lesser discussed but none-the-less crucial vaccine is the one for pertussis, or whooping cough. Although this is part of routine childhood vaccinations, pregnant women are now being encouraged to get this vaccine again during their second or third trimesters in order to protect their babies from infection – although it is not always readily available.
But amidst all the discussions and buzzwords and Facebook posts, determining the basic information one needs to know can prove difficult – what are the vaccines and what are their links to the diseases they are designed to prevent?
Who should get them? Why? And what are the risks if we don’t get them? Or the side effects if we do?
HUMAN PAPILLOMAVIRUS (HPV)
Before we examine the HPV vaccine, it is helpful to take a step back and look at the information about HPV, the virus that the vaccine targets.
HPV infection is the most common sexually transmitted infection – in fact, 90 per cent of us will acquire a HPV infection at some point in our lives, according to Dr Máirín Ryan, Hiqa’s deputy chief executive and director of health technology assessment. Most of us will clear the infection spontaneously, but the concern for the five-10 per cent of us who do not, is its link with cancer, as a sustained HPV infection is associated with a range of cancers.
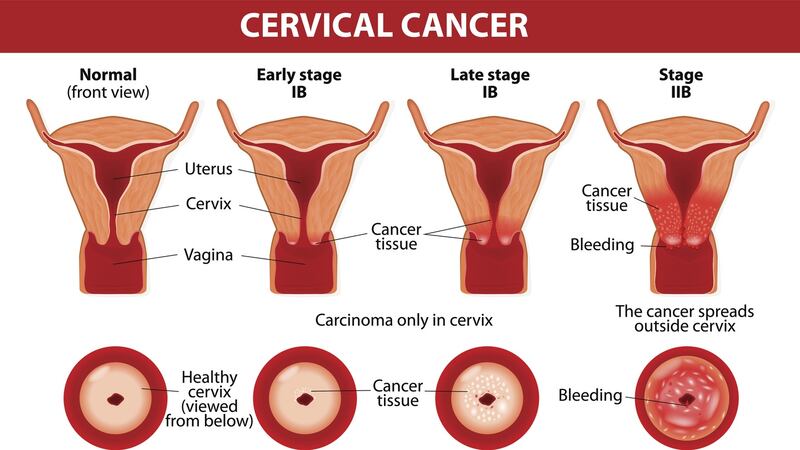
Dr Ryan says women carry the greatest burden in relation to HPV, as the most commonly associated cancer with the virus is cervical cancer.
According to the HSE, more than 6,500 women need hospital treatment for pre-cancer of the cervix every year in Ireland, while 300 get cervical cancer, and 90 women die from it annually.
Other types of cancer associated with the infection include vulval, rectal, penal and head and neck cancers – in 2011, Michael Douglas notoriously attributed his throat cancer to having oral sex with his wife, Catherine Zeta Jones (he has since apologised for the inaccurate – and mortifying – comments).
Along with these types of cancer, the HPV virus also causes anal and genital warts, of which there are about 3,500 cases diagnosed per year in Ireland.
Benefits of the HPV vaccine
According to Dr Ryan, studies show the HPV vaccine is 80-98 per cent effective in preventing HPV infection and HPV-related diseases. However, data on actual cases of cervical cancer are not yet available, as most national vaccination programmes are about 10 years old (ours began eight years ago) and the period between infection and presenting with cervical cancer can be up to 20 years.
There are both individual benefits and larger, population-wide benefits to HPV vaccination, according to Dr Ryan: “When you vaccinate a person, they themselves are protected, but when you vaccinate a substantial proportion of the population, the levels of circulating virus in the population decreases to such a level that everybody gets the benefit.”
Prof Mary Horgan, a consultant physician in infectious diseases and internal medicine at Cork University Hospital, concurs: "If someone told us we could take a tablet to prevent cancer, nobody would have an issue. The HPV vaccine has a long track record. It's proven to be safe, and it's proven to be effective."
The HPV national vaccination programme for girls
A routine HSE school HPV vaccination programme began in May 2010, for girls in their first year of secondary school (or those who were 12 years old and in special schools or homeschooled). The vaccine, which protects against seven out of 10 cervical cancers, is provided free of charge to the pupils by teams from the local health offices, who visit the schools.
In September 2018, the HSE reported an increase in HPV vaccination rates, with provisional national uptake levels at 65 per cent. This figure represented a significant increase in uptake, as the national uptake dropped to 51 per cent in the 2016/2017 academic year, due in part to negative online comments and campaigns from anti-vaccinators. However, the latest figure still falls well under the HSE’s target for the uptake of at least 80 per cent.
Gender-neutral HPV vaccination
On October 9th, Mr Harris announced that some of the new funding allotted to the Department of Health in this year's budget will go towards extending the HPV vaccine to boys. This announcement comes on foot of Mr Harris' request that Hiqa conduct a health technology assessment (HTA) into the evidence and cost-effectiveness relating to the provision of gender-neutral HPV vaccinations. The Minister requested this HTA on foot of recommendations from the National Immunisation Advisory Committee that boys be included in the HPV vaccination programme. With the public consultation complete, Hiqa is expected to submit its final recommendation to the department in November.

Mr Harris has indicated that, subject to a favourable recommendation from Hiqa, the Government will seek to extend this vaccine to boys as well as girls as a priority, and the new funding will help to facilitate this in 2019.
Dr Ryan says, while providing boys with the HPV vaccination will obviously help them on an individual level, it will also benefit women later in life by boosting the immunity of the population as a whole.
Hiqa’s review also evaluated the safety of the HPV vaccine, and found that while mild side effects such as redness and soreness at the site of injection are common, there are no serious negative side effects.
HPV vaccine for women
Women who did not receive the HPV vaccine in school can get it through one of the Dublin Well Woman Centre clinics or through their GP.
Dr Shirley McQuade, medical director of the Dublin Well Woman Centre, said they offer women the HPV 9 vaccine. This is similar to the vaccine provided through the HSE school programme, but has been available in Ireland for just 18 months, and offers protection against 90 per cent of cervical cancers. There's also no upper age limit, so women of any age can get it and benefit from the protection it provides.
There’s a catch, though. There is currently no programme in place enabling women to get the vaccine, which means we must pay for it ourselves. Each jab costs €200, and you get three jabs over the course of six months, meaning a woman must pay €600 out of pocket, plus the costs to administer the jabs.
Women in Ireland get their first smear test at the age of 25. As the school HPV vaccination programme began only eight years ago, Dr McQuade and her colleagues are still seeing women who have not yet benefited from the vaccine – but that will change in a few years.

“I see the other end of things, where the 25- to 29-year-olds are coming in for their first smear test, and many have high-grade changes going on [with their cervical tissue],” says Dr McQuade. “In the next couple of years, we’re going to start meeting the 25-year-olds having their first smear tests who’ve been vaccinated for HPV. Hopefully, we’ll start seeing a difference.”
Long-term investment in healthcare
Consultant physician Prof Mary Horgan, who is also president of the Royal College of Physicians Ireland, said the HPV vaccination is a crucial part of long-term investment in women’s healthcare.
“The HPV vaccine prevents something that may happen in 10 or 20 years’ time, which will avoid an overstretched healthcare system, and people becoming ill in the future,” said Prof Horgan.
“That’s how we should be running our health services – we should not be thinking about putting bandages on problems that happen now, but thinking long term, having a vision for women’s health, and thinking about the long-term gain. Investing now in HPV vaccination will be hugely beneficial to our population in the future.”
THE FLU VACCINATION
Another vaccine that receives a great deal of attention, particularly around this time of year, is the flu jab which children and adults alike can get.
Many employers are now recognising the negative effect that illness, particularly in the winter months, has on their workforces and are providing the flu vaccine to their employees.
And although the vaccination cannot always prevent someone from getting influenza – due to the constant mutations of the disease – it can go a long way towards both prevention and protection, according to Prof Karina Butler, consultant paediatrician and chair of the National Immunisation Advisory Committee.

She warns that the flu vaccine specifically targets influenza, whose onset is swift and whose symptoms include aches throughout the body, fever and the feeling of being completely wiped out. It does not ward off illnesses which might be commonly referred to as the flu, such as head colds.
On foot of predictions from the World Health Organisation, this winter's flu vaccine contains protection against three strains of flu virus. The flu vaccine is not a live virus, which means it stimulates your immune system without giving you the flu, although people can experience some soreness in their arms just after they get their jab.
"The influenza virus is a particularly challenging virus to develop a vaccine for, because it's a virus that has the capacity to drift and shift, in that it can change its genetic material from year to year," says Prof Butler, who is also UCD clinical professor of paediatrics and infectious diseases specialist at Our Lady's Children's Hospital Crumlin and Temple Street hospital.
“What you’re trying to do is to get what might be a protective response against what is a common part of the virus that will be less likely to shift, but you are also trying to anticipate which of the strains are the ones that are going to be circulating in any given year, and to try to protect against that.”
Who should get the flu vaccine?
While the HSE recommends that everyone gets the flu vaccine, vulnerable groups are particularly encouraged to do so. These groups include people who are 65 years or older, those living with a long-term health condition, women who are pregnant, healthcare workers and carers, those living in a long-term residential care and those who regularly come into contact with pigs, poultry or waterfowl.
People within these high-risk categories, as well as those with Medical or GP visit cards, can get the flu vaccine free of charge, although there may be a consultation fee. Adults can get the vaccine through a pharmacist, GP or occupational health centre, while children should get them through their GP.
Preventing other diseases
Getting the flu vaccine can not only protect you from influenza, it can also protect you, your children and other people in your life from other bacterial infections, including meningitis.
“You might get the flu, and get over it, but the flu makes you more susceptible then to getting a serious bacterial infection,” says Prof Butler. “So we often see the flu as the forerunner to pneumonia, and the same with meningitis. Every time we get a series of flu, we see an upsurge in meningococcal infection.”
PERTUSSIS VACCINE FOR PREGNANT WOMEN
In line with HSE recommendations, Prof Butler says mothers who get the pertussis (whooping cough) vaccination during pregnancy can protect their newborns from the disease. Although babies receive the jab themselves at two, four and six months of age, contracting the disease before they are fully immunised can have very serious consequences.
Although whooping cough has been largely eradicated thanks to immunisation, there are still several dozen cases each year, mostly in babies less than six months of age, according to the HSE. In 2015, there were 117 cases of pertussis, up from 73 cases in 2014. In 2012, two babies died as a result of the disease.
The way to protect young babies from this is for pregnant mothers to get immunised during the latter part of the second trimester or the early part of the third, says Prof Butler.
“Pertussis is different to flu, in that it is a bacterial infection,” she says. “It used to be called the 100 days cough because when you got it, it stuck around. For everyone who is beyond the first year of life, it’s unpleasant and uncomfortable, and can cause significant lung damage, but, in general, it’s not life threatening. But where it does threaten life is for young babies, particularly in the first six months of life.”
Everyone in Ireland is vaccinated for the whooping cough as babies, but adults can still contract the disease, even if it manifests itself as a mild cough – but then we can pass it on to others, including newborns who have not yet had their vaccines.
“For young babies, pertussis can cause them to stop breathing, and it can cause very severe pneumonia that really doesn’t respond that well to treatment at all,” said Prof Butler. “The way to protect these infants is to vaccinate the mothers, to boost the immunity that they have, so they will have their antibody level that are passed with all their other antibodies to the babies, so that the babies are protected.”
Problems with provision
But according to Prof Butler, getting the pertussis vaccine, or Tdap, may not be as easy as one would think. “The vaccine is provided by the National Vaccination Office,” she says. “But there has been no agreed pathway for how the vaccine is to be delivered, so there’s been no agreement with the GPs to deliver it, or contract arrangements made. And traditionally, obstetricians don’t see it as their role, or the maternity services, to offer vaccines. And therein lies the rub.”
A spokeswoman for the Department of Health said that, since September, 2013, the HSE has provided the Tdap vaccine to GPs for pregnant women free of charge. However, administration fees have not been agreed, which means that women are liable for the administration fee.








