It has been 23 years since Frenchman Jean-Pierre Bars attended a job interview in Greenwich, Connecticut, for a restaurant manager position. Sitting across the table was a Longford woman – Maria Harte. She was the financial controller of a large hotel restaurant chain.
These immigrants, sitting across the table from each other, were looking for the promise of America.
“I really fell for her the first day,” Jean-Pierre says. “My brother was waiting for me outside. I told him, ‘keep me away from her as much as possible because she is going to be the one’. I got it all, I got the job, I got the girl and four years later we were married, pregnant and I opened the restaurant.”
In 1999, Chez Jean-Pierre opened in the upmarket town of Stamford, Connecticut north of New York City. Life was good. Chez Jean-Pierre did well and was listed in Zagat, the guide to the best restaurants in the United States.
Maria completed her MBA and got a job as a financial analyst for a firm in Greenwich. The couple had their second child and then a third, but there was a spectre hanging over the family.
Maria’s father Eugene, a well-known publican, died in his 40s in the 1980s. It was assumed he passed away from early onset Parkinson’s disease, but then Maria’s sister Brigid began to develop similar symptoms in her 40s.
Parkinson’s is not hereditary, but an illness called Pallido Ponto Nigral Degeneration (PPND) is. Anyone who inherits the gene has a 50-50 chance of developing PPND. It affects the brain’s ability to produce the tau protein, which supports nerve cells in parts of the brain. The patient exhibits symptoms similar to Alzheimer’s or Parkinson’s disease, but the root causes are different.
PPND is progressive and debilitating. It is also extraordinarily rare. About a dozen people in the world have the condition. Eight years ago, Maria started to exhibit the symptoms, slowly at first. “It’s a very sneaky illness. It’s not like you wake up one day and you have a fever,” Jean-Pierre remembered. “You start to not remember things. Things don’t move as they used to.”
Maria became tired and incoherent. She could no longer drive. Jean-Pierre drove her to work and then returned to his restaurant business.
Then she stopped working.
Something had to give.
America, a great country when you are on your uppers, is a cold place for the ill
Paris-based Brigid, an arts curator who was described by the writer Anne Haverty as being "extraordinarily beautiful", died in February 2012.
When Maria's diagnosis came, she wanted to return to her family in Ireland.
America, a great country when you are on your uppers, is a cold place for the ill.
“She understood the gravity of the illness. She said that if she had five to eight years to live that she would like to move back to Ireland,” said Jean-Pierre.
The family moved to a house beside a lake in Glasson outside Athlone in 2013, near where her father had run the the Dog and Duck pub.
Jean-Pierre hoped to set up a B&B business, but caring for his wife is all consuming. Their three boys, 18, 14 and 9½, are at school and busy with rowing, soccer and rugby. The youngest does not remember his mother being well.
Life goes on, as it must.
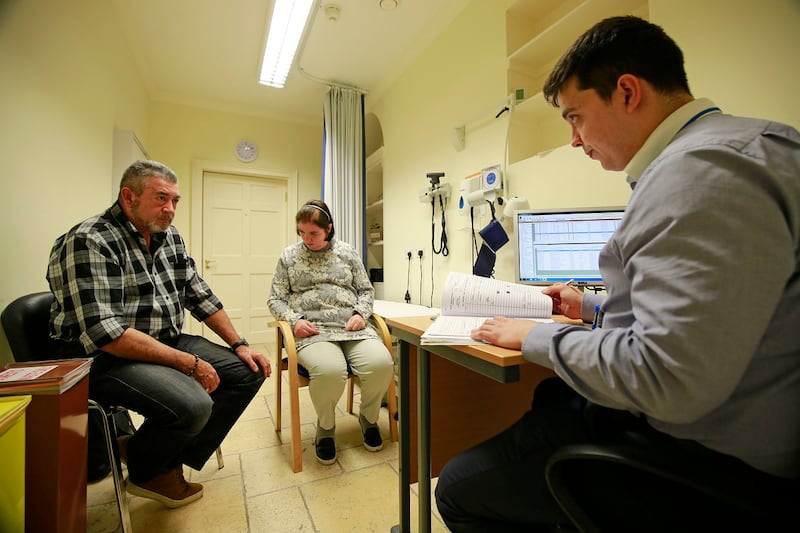
Since being diagnosed, Maria has rediscovered her faith. A priest comes to the house twice a week for Mass. She wears a Virgin Mary pendant on her visit to the Dublin Neurological Institute.
Sitting in small office of the basement of the institute, Jean-Pierre squeezes his wife’s hand and puts a band in her hair.
Progressive illness
The couple visit the institute twice a year hoping a treatment will be found to stop or reverse the progressive illness.
“For me, it is trying to find more explanations on how to deal with it. Are there any new trials?” Jean-Pierre says. “Now we are thinking of the children. We’ll have to see what the future holds for them, always hoping that something will come to us.”
Jean-Pierre says his wife’s loss of memory is particularly galling for a couple who had so many good times together.
“Maria remembers what happened six or seven years ago accurately, but everything from the last five minutes she will not remember. Even the good things she does not remember. Two minutes later, it is gone. Just to see her happy, I tell her good news 20 times.”
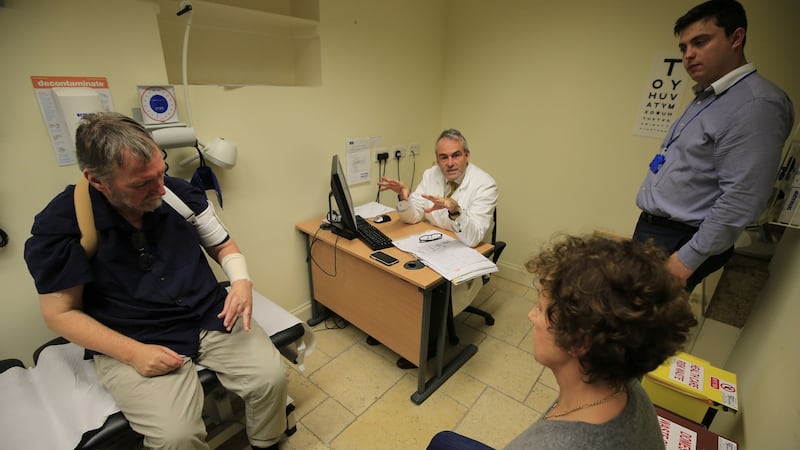
"How did you explain Donald Trump to her?" responds Prof Tim Lynch, the founder and clinical director of the institute.
He founded the institute in 2008 when he discovered he did not have enough space in the Mater hospital for his neurological patients. At the time, they were being seen in a portacabin at the rear of the hospital.
The institute was opened by former president Mary McAleese at a cost of €3.4 million, much of it from philanthropic sources, including a donation from the Athlone-based Élan Corporation.
Lynch has a word or a witticism for everyone. He explains at length the nature of a patient’s illness and the treatments where there are ones available.
“I try to be as positive as possible. I try to retain a sense of humour. You can’t be flippant by any means. People are often dealing with terrible disorders and we often don’t have specific treatments. You can have a bit of a laugh and a bit of fun at the same time because that is all we are doing for them.”
Some of the neurological conditions he treats are among the most insidious diseases. Dementia and Alzheimer’s disease have confounded the billions of dollars spent on them by pharmaceutical companies.
An ageing population means neurological conditions are no longer solely the preserve of the unlucky few. Most young people today have a reasonable expectation of living until they are 85. If they do, 40 per cent will develop Alzheimer’s. The rest will be directly impacted by somebody close to them who will have the disease.

Optimism
Still, he remains an optimist. It helps, he says, especially, when you are a neurologist. “You cure nothing in medicine, with rare exceptions,” he says. “Unfortunately, these neurological problems, Parkinson, Alzheimer’s, Basal Syndrome, we don’t have a cure yet. The tools to understand the brain have only been addressed in the last 10 years.”
The institute is on four floors over the basement of a handsome old red brick Georgian building at 57 Eccles Street opposite the Mater Private hospital.
If you were to build a neurological institute from scratch, you might not build one like this for people with often limited mobility, but a few discreet lifts built into the fabric of this listed building means everything works well.
Patients wait in a large drawing room.
How is the institute funded? 'On a wing and a prayer'
In the corner, Pauline Johnson, a music teacher, plays a piano. Patients are invited to learn or to play. Often, either activity is a sign of rehabilitation.
People look at the grand surroundings and assume it is a private clinic, but, as Prof Lynch points out many times, it is a charity.
Access is not determined by means. Private and public patients get treated the same.
How is the institute funded? “On a wing and a prayer,” says Lynch. They treat 5,500 patients every year. There are 10 staff, including five clinical nurse specialists.
Private donations
Many of the staff, including Lynch, have their salaries paid for by the Mater Hospital. The balance, approximately €500,000 a year, is fundraised mostly from private donations, legacies and a golf classic every September.
It is a hybrid model that has been pioneered in the United States and really works, he claims. “Strangely, in Ireland we haven’t done that. Are you public or are you private and never the twain shall meet? It always struck me as kind of illogical.”
He would like to set up similar neurological institutes in other parts of the country. The demographics demand it, though neurology is under-resourced in Ireland. He is looking for public donations.
“You get best value for your money and excellence in quality of healthcare,” he adds. “We have been able to lower the length of stay for patients with a neurological problem in the Mater by three days.”
In a sun-filled annex overlooking the institute’s urban garden, patients are receiving their infusions.
Not all neurological conditions are untreatable.
There has been undeniable progress in the treatment of many difficult conditions.

Louise Cunningham (32), a mother-of-three, is receiving her infusion of Tysabri, a monoclonal antibody developed initially by Élan which has had a transformational impact on patients with the relapsing-remitting form of Multiple Sclerosis (MS).
Tysabri has cut the number of relapses and the severity of the ones that occur. It has made a big difference to the lives of MS patients who are responsive to it.
“It makes me live a normal life with my children. I can get up and get on with everything,” she says.
Another receiving an infusion is Seán Manning from Finglas who suffers from neuropathy which causes stiffness and reduces mobility significantly.
Different antibodies
Manning visits the institute monthly to avail of the treatment. He whiles away his time looking at the bees in the institute garden. This treatment consists of a mixture of different antibodies delivered through an intravenous drip. Neuropathy can be a debilitating, insidious illness which leaves the patient unable to dress themselves or do a lot of those finicky things we take for granted. The ability to do the simple things the rest of us take for granted is often all neurological patients desire.

“It has got me back that I can do practically everything for myself and by myself. It’s marvellous stuff,” he says.
The institute puts a big emphasis on education to help patients understand their condition and the treatments they are receiving. Lynch spends his time cajoling his patients to participate in clinical trials.
“As stated I am an optimist,” he says, “however we have had a series of trials for neurodegenerative disease (AD and PD) in recent years and although they failed we have learned a bit more each time.”
He believes an effective treatment for Alzheimer’s disease and Parkinson’s disease will be found, citing a recent successful trial in Spinal Muscular Atrophy (a lethal form of Motor Neuron Disease – MND – in children).
“Hopefully, we will start delaying and offsetting some of these diseases. It is remarkable that you have a therapy that can stop and reverse a disease in children. How long it is going to last we don’t now, but it is an important chink in the armour. We will start delaying and hopefully offsetting some of these diseases.”
He is even hopeful the gene which has caused so much heartache to the Harte family can be turned off.
"We have a collaboration with a group in Australia, " says Lynch. "We are hopeful that we can come up with ways of shutting down the abnormal gene, leaving the normal gene that she (Maria) has from her mother.
“It is possible to do that in animal models. We’re not that far from a mouse or a rat.”










