Prader-Willi syndrome (PWS) is one of those rare genetic disorders you often only discover when you meet someone with the condition. There are about 100 people in Ireland living with PWS, but the wide range of symptoms and behaviours associated with the condition means that these individuals need very particular medical and social care throughout their lives.
It is for these reasons that the Prader Willi Syndrome Association Ireland (PWSAI) recently launched the first national survey of the needs of people with PWS.
“PWS typically causes low muscle tone, restricted growth, learning difficulties, problem behaviours and a chronic sense of hunger that can lead to excessive eating and life-threatening obesity,” says Anthony Carr, chairperson of PWSAI and father of Lauren (9), who has PWS.
As children with PWS grow into adults, other medical and psychiatric problems can arise, including scoliosis, seizures, sleep apnoea, gastro-intestinal, hormonal and skin problems, depression, anxiety and psychosis.
We had 107 medical and therapeutic appointments in the first year of Henry's life
“It is recognised as one of the most medically complex syndromes to live with and care for by medical professionals – and there is no cure,” says Carr.
The hallmark characteristic of PWS is hyperphagia, an insatiable appetite or drive to get food. This means that access to food must be restricted (including locking kitchens and no money to buy food) for people with PWS.
“People with PWS need what’s called psychological food security – they need to know what they’ll eat, how much and when, but also that they have no hope of getting food anywhere else at any other time. So they can’t scavenge, manipulate or argue for food,” explains Jane Cox, whose daughter Laura has PWS. People with PWS need between 50 and 80 per cent of the calorific intake recommended for their age group.

At the launch of the survey of the needs of people with PWS, parents and siblings spoke honestly and frankly about the difficulties they face getting adequate therapies and support services.
Rory Tierney, whose son Henry (4) has PWS, says that the day he was born was the saddest day of his life.
“We had 107 medical and therapeutic appointments in the first year of Henry’s life,” he says. “We read everything looking for a cure and we’ve had to fight for speech and language therapy, occupational therapy and preschool supports. Most people see a happy, quiet boy, but I’m scared for the future.”
PWS survey
Prof Louise Gallagher, chair of child and adolescent psychiatry at Trinity College Dublin, was the lead researcher on the PWS survey carried out with the National Children’s Hospital, Tallaght.
“There are five to six children born every year in Ireland with PWS. We hope this survey will help the PWSAI campaign for better health and educational services. There is a significant emotional trauma, stress and anxiety on parents if they aren’t given services specifically geared towards PWS. There is also an impact on siblings because parents have less time to be available to them,” she says.
Ann O’Neill, whose son Oisin (13) has PWS, says that family, friends and neighbours all work hard to support Oisin.
Living with PWS has put a huge strain on our lives
“His siblings are the Prader-Willi police in terms of preventing his access to food]. We tell them that Prader-Willi is not Oisin’s fault, it’s not our fault or anyone’s fault.”
Prader-Willi syndrome is the result of a genetic disorder on chromosome 15.
At each developmental stage, there are specific challenges. Jane Cox says that for her daughter Laura (18), the transition from special school to adult services was extremely stressful.
“Laura’s mental health deteriorated over the last two years and I’ve been on carer’s leave from my job as a teacher in a special school. Living with PWS has put a huge strain on our lives. My husband and I can no longer go on holiday together or even go out to dinner as a family,” explains Cox.
The survey found that 60 per cent of families with a teenager with PWS and 75 per cent of families with an adult with PWS have no access to respite services. Only 6 per cent of those caring for young children with PWS have access to respite care. Families with an adult or child with PWS are now calling for more Government-funded respite services.
Finding full-time PWS-specific accommodation for adults with PWS is also extremely difficult. Currently, there is accommodation for six people with PWS but the survey has found that 16 people with PWS will require accommodation in the next five years.
What families of people with PWS now need is for those words of support to be turned into action
Elisha Doyle says that the physical and mental health of her sister Bernie Nolan (27) has deteriorated since she returned from a PWS-specific facility to live in a residential setting in Ireland that is not dedicated to PWS.
Diabetic medication
“She has put on weight and her diabetic medication has increased. She is obsessed with medications and attends the out-of-hours doctors weekly, constantly seeking pain relief. Her skin-picking are cries for help going unheard.”
Minister for Health Simon Harris, who attended the launch of the survey of the needs of people with PWS, says he is committed to “breaking down the barriers of ignorance of the condition in the health services” and promised “a road map for delivery of services for children with PWS”.

What families of people with PWS now need is for those words of support to be turned into action. The PWSAI is specifically calling for more respite places, three new residential centres for those reaching adulthood and the appointment of a consultant psychiatrist who specialises in intellectual disability and rare disorders.
What the rest of us need is greater understanding of the stresses faced by families with a child or adult with disorders like PWS – and offers of practical help to those who are struggling to cope.
Case study: Ted, Jane and Laura Cox
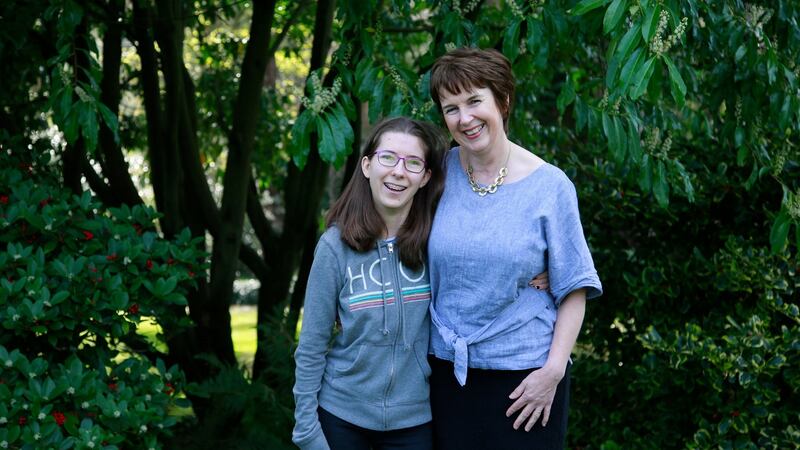
Ted and Jane Cox’s daughter Laura (18) was diagnosed with Prader-Willi syndrome (PWS) when she was three months old.
“She was an extremely floppy baby. She was a poor feeder and had difficulty latching on to the breast,” explains Jane.
“Laura spent four months of her first year in hospital and she was on oxygen at all times until she was 10 months old.”
Laura Cox attended a special preschool until she was six and then went to mainstream school until she was 14 with the support of a special needs assistant. She went to a special school from age 14-18. “Laura has a mild intellectual disability. She has tremendous verbal skills and reads for pleasure but her maths ability is senior infants’ class level,” explains Jane.
As with many children with PWS, Laura has many medical issues including gastro reflux, low thyroid function, a congenital heart problem and spinal abnormalities (scoliosis and kyphosis).
“Like many other families, we waited a year beyond the optimum time for spinal surgery.”
While Laura coped reasonably well as a child, she became more anxious as a teenager. Transitioning from secondary school to adult day services has been extremely stressful for Laura.
“Laura’s mental health deteriorated in the last two years. I have been on carer’s leave from my job as a teacher since June 2016. Living with PWS has put a huge strain on our lives,” Jane says. “My husband and I can no longer go on holiday together or even go out to dinner as a family.”
In the short term, “we long for some overnight respite to get a rest from the gruelling routine and to spend a little uninterrupted , time with our other young adult children. Through no fault of her own, Laura’s needs are always immediate and paramount.”
Longer term, Jane Cox would like to see Laura move into a community house with Prader-willi-specific care.
Case study: Jackie, Des and Fianna McHugh

Jackie McHugh speaks about life with her daughter, Fianna (4) who has Prader-Willi syndrome.
Jackie and Des McHugh’s second daughter was born at 35 weeks by emergency Caesarean section, following early labour. “She was a very quiet baby with poor muscle tone which affected her swallow and eating muscles. Three weeks later, we were told she had Prader-Willi syndrome.”
Jackie McHugh wouldn’t recommend new parents google PWS, as “you get every horror story about over-eating and skin-picking”.
She says that luckily for her, two of her friends had seen a documentary on PWS with children running around and playing, which was a relief to her.
Fianna had to be fed small amounts every two hours for her first six months.
“She didn’t cry. We only had little gurgles. She was like a quiet little doll.She only began to make sounds when she started to take solid foods,” explains Jackie.
Fianna McHugh attends the Prader-Willi clinic in Tallaght Hospital for treatment with endocrinologist Edna Roche. She also receives physiotherapy, occupational therapy, play therapy and speech and language therapy.
She was diagnosed with sleep apnoea following two sleep studies in Tallaght Hospital when she was just over two years old. Since then, she has been wearing a mask at night time to keep her breathing controlled.
Fixated behaviours – including a stronger interest in food – have started to appear.
“It’s harder to distract Fianna now when she wants food. Routines around food have to be harshly enforced as she only needs two-thirds of what other children her age need due to her slow metabolism.”
Jackie is keen to point out that Fianna’s older sister Molly (6) is a very empathic and supportive child. “She loves her little sister .”
Fianna is currently in a mainstream playschool and the McHugh family hope she will start mainstream primary school in September 2018 with the support of a special needs assistant.
“Often, I think the focus is on Prader-Willi so much. Fianna is a happy little girl who is so full of affection who happens to have Prader-Willi syndrome.”











