We’ve all heard of people who have had shingles but unless we’ve experienced it ourselves, many of us don’t know what it entails or, indeed, how painful it can be.
Approximately 10,000 people get shingles every year in Ireland, with two-thirds of those cases occurring in those over the age of 50.
The varicella zoster virus, which causes shingles and chickenpox, stays dormant in your body even after symptoms go away. So, although it is not very common, people can and do suffer with it on more than one occasion, with recurrence being more likely in those with long-lasting pain during the first episode of shingles, people who are immunocompromised and older age groups. There also seems to be a greater likelihood of recurrence in women.
The first signs of shingles can be a tingling or painful feeling in an area of skin, a headache or feeling generally unwell, as Senator Gerry Horkan can attest. “I realised that I had shingles on the Sunday of the bank holiday weekend in August, 2020. I felt what I thought was muscle strain in the few days before, but thought that maybe I had stretched awkwardly or strained myself cutting the grass – and thought the pain would go away. But that Sunday morning when I looked in the mirror and saw a big rash, I realised it was a bit more than just muscle strain. It felt like a stinging pain and was very uncomfortable, making it hard to sleep or relax as I just couldn’t stop thinking about it.
READ MORE
“So, I went to VHI Swiftcare in Dundrum, where I was diagnosed with shingles, something I knew very little about – but I now know that it’s basically a recurrence of chickenpox which lies dormant. I was prescribed with medication to treat the constant pain and the rash which blisters over time, and also the longer-term nerve pain (post-herpetic neuralgia) – this has probably been the worst, as it’s hard not knowing if it will go ever go away.”

The 52-year-old says that before being diagnosed himself, he had assumed that the condition only affected the elderly or people who were already sick and he feels that a bout of coronavirus weakened his immune system and left him susceptible to shingles. And he spent several months on medication afterwards. “I think I got Covid in January 2020, long before people were talking about it, as I had a severe cold/flu with a temperature, I lost my sense of taste and I felt exhausted. This was during the general election campaign and I think it possibly weakened my immune system, giving the shingles a chance to strike – apparently, it tends to hit people who are already weakened in some other way.
“Once diagnosed, I took the course of medication as prescribed – I don’t know how much it helped, but I presume I was better taking it than not. I was also prescribed Lyrica/Pregabalin – the medication for nerve pain which was in the news recently. It is prescribed for people with long-term pain and has been used for those experiencing severe pain from surgery and other issues. But it’s highly addictive and I felt a kind of a brain fog, so didn’t like it at all. It was also mentioned that it can cause suicidal ideation but thankfully I didn’t have that.
“I stayed on it until November, but could have stayed on it for as long as I wanted as my doctor was happy to prescribe it if I felt I needed it. I reduced my dosage faster than possibly recommended as I felt that the increased pain was better than the side effects of staying on the medication.”
The senator says life in 2020 was strange due to the recurring lockdowns brought about by Covid, but the diagnosis of shingles made it even more so. Today, he still feels some pain associated with the illness and would advise others to learn all they can about it and not to assume that it won’t happen to them. “Thankfully, when I had shingles, I wasn’t in public life at the time so was able to rest and hope that the pain would eventually go away.
“The rash resolved itself after around a month or two, but the nerve pain went on for a long time – even now, over 3½ years later, I still have pain on that side of my body and am sure it is a long-term effect of shingles.
[ Shingles vaccine too expensive for routine immunisation, regulator findsOpens in new window ]
“I would advise people to familiarise themselves with the symptoms as, if I had realised earlier, the medication may have had a greater chance to deal with the shingles before it took hold. I would also encourage people to consider the shingles vaccine, something I had never heard of, as I believe it is very effective.
“I wouldn’t wish shingles on anyone and prevention is better than cure. I have asked the Minister for Health to make the vaccine available without charge, which is not the case currently. It would avoid the cost of the retroviral drugs but also keep people healthy and in the workforce as opposed to being sick with potentially further complications as a result of a weakened immune system.”
Some general tips for managing the symptoms of shingles include:
- Keeping the rash clean and dry to reduce the risk of infection.
- Wearing comfortable, loose-fitting clothing.
- Using a cool compress and/or soothing creams or lotions a few times a day.
- Taking painkillers and/or anti-itch medication as recommended by your healthcare professional.
About shingles
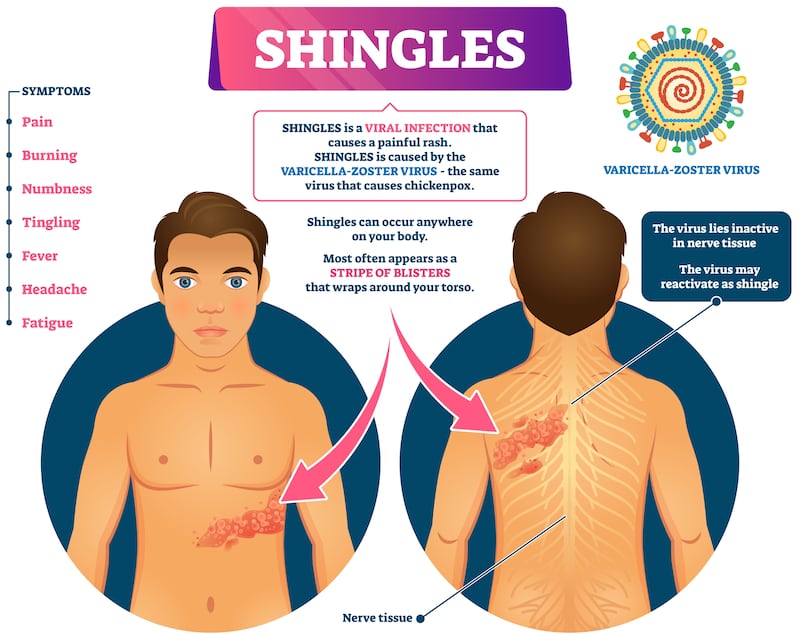
- Shingles, also known as herpes zoster, is a condition that often presents as a painful rash.
- It is caused by the reactivation of the Varicella zoster virus, the same virus that causes chickenpox. After a person gets chickenpox, the virus stays dormant inside the body for life, usually not causing any problems or symptoms until older age.
- Our immune system naturally weakens as we get older, this may allow the usually inactive virus to reactivate, causing shingles.
- If you had chickenpox as a child, you can develop shingles, most likely, much later in life. The chickenpox virus remains dormant in the body and, as our immune system naturally weakens over time as we age, this may allow the usually inactive virus to reactivate, causing shingles.
- There is a one-in-three lifetime risk of the dormant varicella zoster virus reactivating and causing shingles typically in people over 50 years of age or those with a weakened immune system.
- If you have any concerns, seek medical advice from your GP.

















