Half of all patients in Irish hospitals say they have trouble finding staff members to talk to about their “worries and fears” over treatment, a major new survey has found.
Thousands more claim they are not told about potential side effects of medication or the “danger signals” to watch out for when they go home.
A comprehensive new study, the first of its kind in Ireland, measured the experiences of almost 14,000 patients across 40 hospitals.
Carried out by the county’s health authorities in conjunction with the Health Information and Quality Authority (Hiqa) and the Patient Focus advocacy group, it seeks to measure how people feel about their time in care, with feedback expected to help inform future policy.
The National Patient Experience Survey, published on Monday, is a detailed examination of patient experiences as they navigate the hospital system – from entering emergency departments, to undergoing treatment and eventually being discharged.
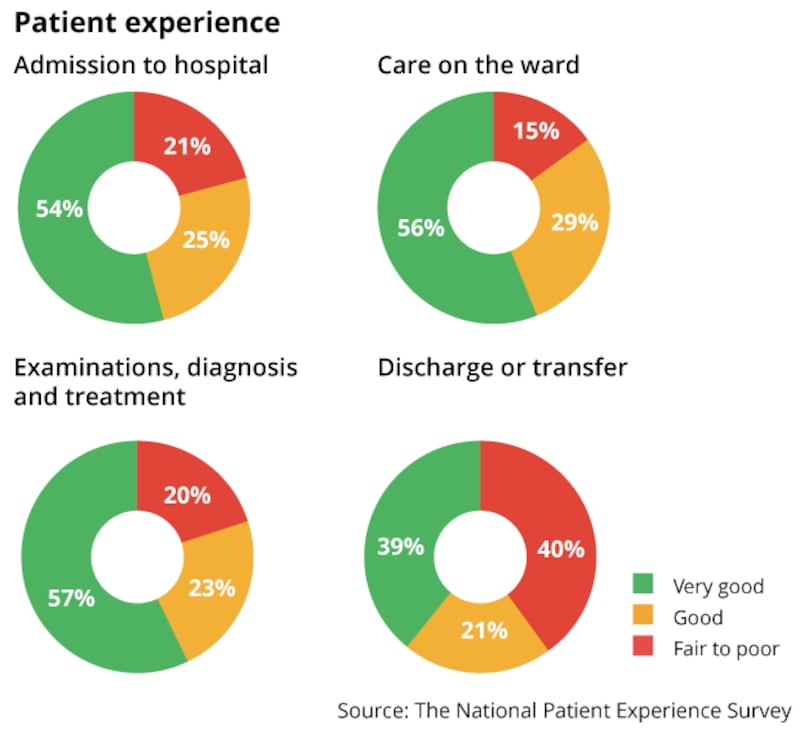
Overall, 54 per cent of people said they had a very good experience and 30 per cent a good experience, with a minority of 16 per cent rating their time in care as fair to poor.
‘Exceptional’
The survey response rate of 51 per cent of patients, aged 18 and over who spent more than 24 hours in hospital last May, is considered “exceptional” by international standards.
However, while feedback was broadly positive, much of the report highlights shortfalls in the system.
Some 70 per cent of people said they had to wait for more than six hours for admission to a ward, while 40 per cent felt they hadn’t enough time to discuss their care with a doctor.
Positive experience types that scored highly included people’s feelings of being treated with respect and dignity in emergency departments, levels of privacy, receiving clear answers from medical staff, having confidence and trust in staff, and responses regarding hospital cleanliness and pain management.
However, there were negative comments from people left on trolleys. One patient said: “The dignity in the A&E department was a disgrace. [I was] left on a trolley to be examined on a corridor with absolutely no privacy at 77 years of age.”
Men were more likely to have had a good overall experience than women while the 18 to 35 age group were the least likely to give positive feedback.
Areas identified as needing improvement included patient involvement in decisions about their care on which one in three respondents complained.
Respect and dignity
The vast majority of people (79 per cent) had a very good or good experience on admission while 96 per cent said they were always or sometimes treated with respect and dignity in the emergency department.
However, just 30 per cent of people said they were admitted to a ward within the target waiting time of six hours and 241 people (3 per cent) said they waited 48 hours or more.
“People aged 18-35 years of age were least likely to be admitted to a ward within the target waiting time of six hours,” the report noted.
When it came to the quality of care received on wards, the majority (85 per cent) said they had a very good or good experience.
Almost one-third (31 per cent) rated their food as either “fair or poor”.
Those aged 50 years and younger reported more negative experiences of their time on the ward than older people, but most appeared happy with levels of cleanliness.
“A very large number of comments praised the competency of doctors and nurses,” the report said.
“However, people were less positive about the amount of time allocated to talk about their treatment, and their involvement in making decisions about their care. This suggests that care was not as patient-centred as it should be.”
Some people also felt more nurses were needed and that they were overworked.
Hospital discharges proved to be the lowest-rated stage of care with only 60 per cent saying they had a very good or good experience.








