It's just after lunch time and Mayah Power, the youngest patient in the National Rehabilitation Hospital (NRH), is lifting toys with her left hand and passing them to her right. Her eyebrows are furrowed, her lips pursed. Her eyes are focused on the task with laser-like precision.
The action is easy for most children, but for the three year old it is monumental. She previously had little to no movement in her left limbs as a result of two strokes she suffered more than a year ago.
“My husband and her were rolling around on the grass and her face was drooping and she couldn’t walk or speak. Straight away we knew it was the sign of a stroke but we never thought that would have happened to her at that age,” says her mother Kayleigh.
"The first one she had was an ischemic attack and then five days later she had a proper stroke. That's when they rushed her up to Crumlin. "
“It just came out of the blue,” she adds.
It’s a “long road to recovery” but they are beginning to see signs of progress. “Before we came up here, she was not using her hand whatsoever . . . the second or third week here, I started to notice a difference in Mayah. She would hold a pen in her left hand, which she had never done before,” Kayleigh says.
Mayah is one of more than a hundred patients receiving rehabilitative care in the Dún Laoghaire hospital's new "state of the art" facilities which opened in June.

The Dublin hospital decanted from its old building to the new one mid-pandemic. However, the opening of one unit, which is specifically for people with the most severe brain damage, has been delayed, due to staffing shortages.
"We just don't have the staff to open it . . . It was a bad time [mid-pandemic] to look for a major tranche of nursing staff in particular," says clinical director Prof Mark Delargy.
The €100 million development includes 120 single, ensuite rooms, integrated therapy services, a hydrotherapy pool and sports facilities.
Built on lands owned by the Sisters of Mercy, but which are in the final stages of being transferred to the State, it is phase one of a larger development project. By the time all three phases are complete, there will be 240 rehabilitative beds.
Prof Delargy says it took a long time to get to this point. First proposed in the 1970s, it fell victim to two economic downturns.
“We re-gathered ourselves and re-budgeted. We changed from a building which was going to be twice this size. We decided it would be prudent to try and develop the services we needed for the country in stages,” he explains.

The NRH also sold land it owned, putting the money it received from that sale towards the new hospital building, amounting to roughly one-tenth of the total cost.
The old building, which had been in use for 60 years, was “not fit for purpose”, he says.
Asked if the final 240 beds will be enough to meet national demand, Prof Delargy’s answer is simple: No, it’s not. “We do need a fully-fledged substantial unit, particularly in Cork,” he admits.
The old building required them to reduce the number of patients it could accept in order to adhere to social distancing on shared wards. But the hospital has remained Covid-free. “Covid in the building would have killed a lot of the rehabilitation. We had to keep it out.”
Despite the curtailing of visitors to patients undergoing rehab at the facility due to Covid-19, many remain upbeat.
Michael Keogh, who has a mild brain injury and had his right leg amputated in February, makes it his mission to keep other patients positive during their recovery.
Sitting in his room, in front of pictures of his two daughters Amelia and Ayda, the 34 year old says the car crash in which he sustained his injuries has given him a new outlook on life.
“I was in a coma for 28 days. They had given me 72 hours to live, but I pulled through, thank God. I broke my two legs, broke ribs and cheekbone and I had a bleed to the brain which weakened my left side,” he explains.
“I count myself lucky every day that I’m alive. I’ve got a second chance at life. There are a couple of lads here who are very down so I try and cheer them up a small bit. I think it’s important to remember that your life is not over.”
He worked as an electrician prior to the accident, but says he now has an opportunity to reinvent himself. “I might have to go back to college and do a computer course. My options are open. I can start over again. I got a second chance at life so I’d like to help people out. I’d like to do talks about road safety and cars and drink and everything. I would love to help people,” he adds.
The Cork man lost a lot in the accident, but not his sense of humour. “It’s like a little chicken wing,” he says laughing, lifting the amputated limb up from his wheelchair. “For a while, I think I thought it was going to grow back.”
Being able to speak to other people in similar circumstances is one of the biggest benefits of being in hospital, Mr Keogh says. It’s a sentiment that fellow patient Deirdre O’Connor shares. The former teacher (32), who has a mild brain injury following surgery, believes leaving that camaraderie when discharged will be difficult.
“We get through it with patient and peer support. When you come here nobody is, like, ‘poor you’. In here we’re not the minority, we’re the majority. But when you go outside, you’re going to be the minority and you need to understand and take it,” she says.

Between 550 and 600 patients pass through the hospital annually on an inpatient and day-patient basis. The initial stringent Covid-19 restrictions increased its waiting list to around 300, but the hospital has brought it back down to 280 in the intervening months.
The waiting list generally ranges from between two and six months, but there are some “outliers”, who could be waiting for up to a year. This is a situation which, Prof Delargy says, is wrong. “We are shamed by that.”

Brian Colleran misses visits due to Covid-19 restrictions. The 33 year old, who is paralysed, is in hospital with a pressure sore and is on bed rest. The only human interaction he has is with hospital staff, who turn him over from side to side every three hours.
How does he keep himself occupied? “I have football. There’s football all day Saturday, all day Sunday, two matches on Monday, football on Tuesday night, football on Wednesday. I’ll watch all of the matches.”
When social media erupted with outrage to the news the GAA championships could proceed under Level 5 restrictions, Mr Colleran breathed a sigh of relief. “I was delighted. It gives me something to watch.”
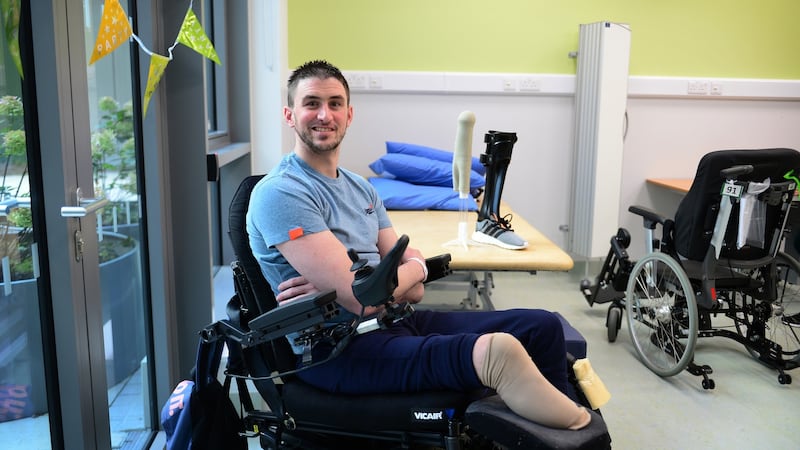
Barry O'Sullivan (52) is a bilateral amputee and lost his fingers after contracting septicaemia in February. After he finishes an archery session at the hospital, he laughs and shrugs helplessly: "I'm almost as bad as I used to be."
Irrespective of his self-deprecating comments, he has come a long way since he arrived at Cork University Hospital in septic shock in February.
“I was home all day chopping wood on the Sunday before I was in hospital. Three days later, I was in a coma.” His voice is surprised, like he still can’t believe how it all happened. “It was a frightening thing that it could come on so quickly with no warning.”
He says being in a coma was the “worst experience of my life”, comparing it to a dream-like state.
“For the first week, before Covid hit, my family were around me and they all thought I was dying. They expected me to die. That’s what the prognosis was. I was screaming for help, or trying to, but I knew my mouth was full of cables and tubes and things,” he explains.
“When the voices disappeared, when they stopped being allowed to come in, in my dream they had all been killed. When I woke up, I was experiencing what’s called ICU delirium. I thought the doctors were experimenting on me, trying to kill me and all that sort of thing.”
After getting through that, rehabilitation is nothing in comparison. He has relearned how to drive using prosthetic legs, is working on his stamina for standing and is trying to improve the movement in his hands.
“The fingers are almost a bigger hurdle because I can get prosthetic feet but I’m a person who does an awful lot with my hands, so although I still have quite a bit of function, that’s never going to be the same.”

When patients are asked what keeps them going during difficult days here, their answers are the same: they want to regain some semblance of normality.
Mr O’Sullivan is no different, though he knows the initial move home will pose challenges. “I know when I go home . . . it’s where I’m going to meet my limitations. The things you used to like doing but can’t do anymore or won’t be able to do for a while at least. My aim is to get back to all of that,” he says.
“What’s motivating me is the need to get back to my life. The need to overcome this. I knew I had to stay focused and get back on my feet. For me, that becomes all consuming.”



















