For decades, the State has been in a demographic sweet spot. Among the raw fuels for Ireland’s economic catch-up phase, which stretched from the early 1990s to the end of the Celtic Tiger, was a favourable age profile.
Irish birth rates remained high well into the 1980s, much longer than other European countries, meaning there is a large cohort of working-age people in the population. What’s more, emigration trends in the 1960s and 1970s mean that many Irish-born people in old age don’t live in the State, shielding the exchequer from the associated spending pressures of their ageing.

But now, Ireland is getting older. And that process will force hard choices.
Ireland’s ageing problem will exert more spending pressure on the already cash-strapped health service, asking it to make long-term, difficult strategic decisions – and get these big calls right.
What are the best ways to care for vulnerable older people? How can families ensure they are financially protected? Can Ireland avoid the scandals and institutionalisation of the past? How can the State pay for this ageing time bomb? There are few easy answers available to the difficult questions it poses.
Only one thing is certain: today’s workers will age and retire, and live longer thereafter; this prompts the fundamental question: are we ready for Ireland to age?
Demographics
Ireland at present is a “young” country, but the number of older people will soar in the years ahead. The Economic and Social Research Institute (ESRI), in a report in 2017, projected that by 2030 the population aged 80 or above would increase by between 89 per cent and 94 per cent.
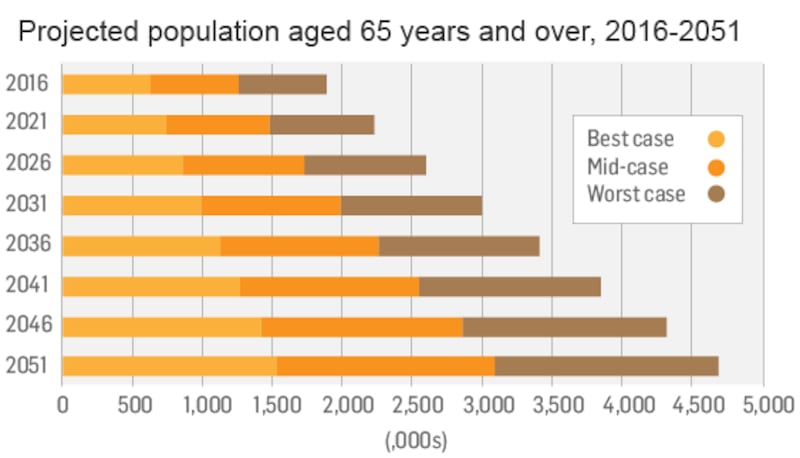
A spending review by the Department of Public Expenditure found that by 2031 more than a quarter of a million inhabitants in the State will be aged over 80 years. Central Statistics Office (CSO) figures predict that those aged 65 years and over will increase significantly from a level of 629,800 in 2016 to potentially nearly 1.6 million by 2051.
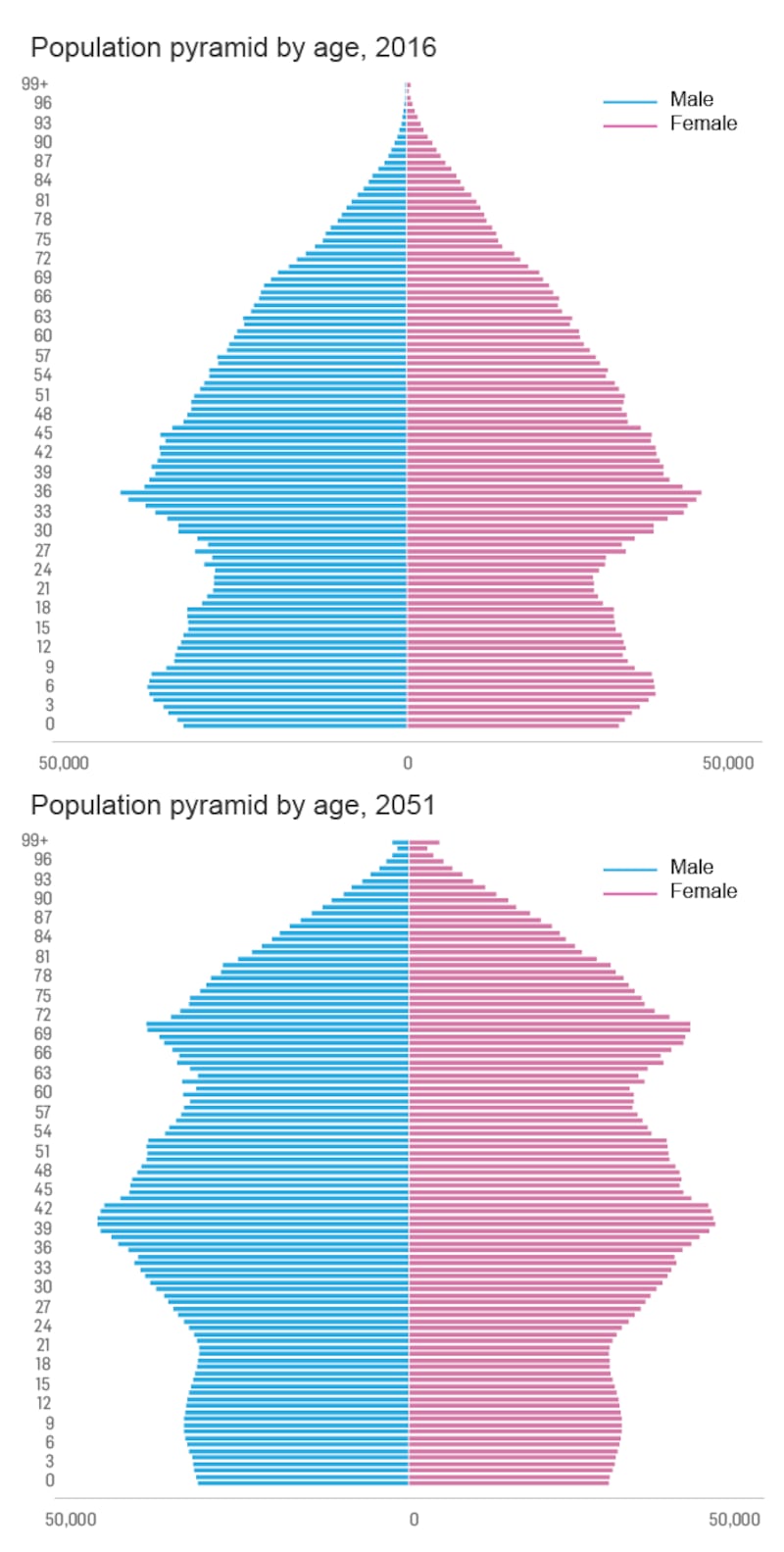
And official projections suggest that the favourable ratios between younger and older persons experienced over recent years will be reversed in the decades ahead.
In 2016 there were just over a million young people in the 0-14 age category, compared with just under 630,000 aged over 65. However, this picture will be turned on its head by 2031 under all scenarios envisaged. “The excess will increase steadily towards 2051, at which stage it is projected that there will be between 496,600 and 691,800 more older people than younger people,” the CSO found.
Impact of change
This shift will have considerable implications both in terms of public policy, for the health service and for the Government’s finances in the years ahead.
According to the ESRI, demand in the residential long-term care sector, which covers nursing homes, is projected to increase by up to 54 per cent, “posing challenges for providers, for the regulatory authorities and for the exchequer to ensure that an appropriate standard of care and level of funding for care is provided for these vulnerable residents with intense care needs”.
In the home help sector, demand for home help is projected to rise by 48 per cent; demand for publicly-financed home care packages will rise by 66 per cent. There will be pressure on other services, such as pharmacies, acute hospitals and occupational therapists.
All this is playing out against the backdrop of a model of health service provision that has chronically struggled to provide adequate, on-budget care. This “will give rise to demand for additional expenditure, capital investment and expanded staffing and will have major implications for capacity planning, workforce planning and training”.
Ireland already spends billions on older people; about €3.6 billion was spent on the ongoing provision of long-term residential care, 78 per cent of it by the State, in 2014. Health Service Executive (HSE) non-capital expenditure on the care of older persons was €1.57 billion in 2015, and with tens of thousands more people set to enter into the older cohorts of the population, those spending pressures will become more acute.
“Additional investment will be required in most forms of care to meet the needs of a rapidly growing and ageing population,” the ESRI warned in 2017.
A fair deal?
The most high-profile State policy for this kind of care is the Nursing Home Support Scheme – more commonly known as Fair Deal.
This year the State will spend close to €1 billion on long-term residential care for more than 23,000 older people under the scheme. However, Fair Deal is also facing financial pressures.
The budget for the scheme this year is €985.8 million, an increase of €24.3 million over the previous year. However, in May the HSE’s top-level performance oversight group raised alarm that the cost of operating the Fair Deal scheme was €5.676 million ahead of the level projected.
It is understood that financial forecasts suggest that the overrun in the Fair Deal scheme will reach about €16 million by the end of the year. It is considered likely that the Government will have to provide additional funding as part of a supplementary estimate in the autumn.
There are also concerns that waiting times for a nursing home place under the Fair Deal scheme are increasing significantly. Official figures given to Fianna Fáil on foot of a parliamentary question have revealed that the number of older people waiting for a Fair Deal nursing home place jumped from 729 to 846 in three weeks this summer.
Delays in approving Fair Deal applications can have significant knock-on effects across the health system, leading to higher numbers of delayed discharges from acute hospitals – people whose acute hospital care has been completed. This in turn can drive up waiting lists and larger numbers on trolleys in hospital emergency departments waiting for admission to a bed.
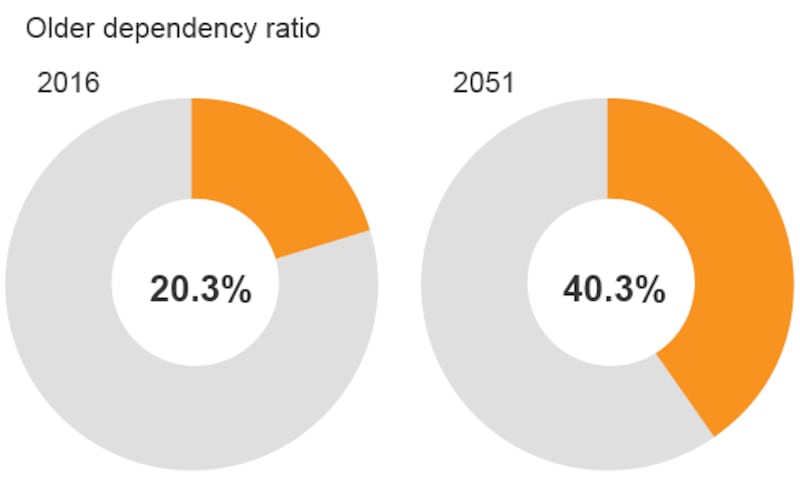
A spending review carried out in 2017 found that Fair Deal had shown itself to be financially sustainable. However, it warned of potential developments that could jeopardise the sustainability of the scheme in the future.
One of these is the amount that the State pays to private nursing homes under the scheme. The private sector provides about 18,000 nursing home beds under the scheme, with about 5,000 public beds also available.
The Department of Public Expenditure spending review in 2017 maintained that not only were the average costs of public beds more than 1.5 times the cost of a private bed, but this gap had also widened over the previous three years. It maintained that the average monthly cost of care was €4,161 in private nursing homes and €6,427 in public nursing homes.
It suggested that this could possibly be due to public nursing homes dealing with people requiring more complex care. However, private nursing home operators contended that the current funding model was jeopardising the sustainability of the sector.
The representative body Nursing Homes Ireland criticises different payments to private and public hospitals, and has argued that the fee system “must be clear, logical, rational, fair, transparent”.
A review of pricing under the Fair Deal scheme is currently being considered by the Department of Health. One of its main recommendations is expected to be a new system of graded payments to nursing homes based on the dependency of the resident.
A changing model
To deal with the future changes and the increased demands that these will bring about, the Government’s strategy is to move away from relying mainly on Fair Deal and existing home support arrangements.
“If you do what you always did, you will get what you always got,” the Minister of State at the Department of Health Jim Daly said last week. Daly said that while he did not see a “doomsday situation” as a result of a growing older population, there were challenges to be managed.
In essence the Government’s proposals centre on reducing reliance on long-term nursing home care and expanding home care support arrangements, with additional funding likely being generated by a financial contribution from recipients.
The Government is also looking at housing and healthcare initiatives to offer more choice to older people than just long-term residential care. Daly said that not everyone needed a 24-hour, nurse-led clinical environment.
Experts argue that shunting older people into out-of-town nursing homes has poor outcomes in terms of physical and mental health, and is undesirable from a town planning point of view. Mick Bradley, an Irish architect with the Danish firm Zeso, has worked on innovative housing schemes that enable people to age in their communities.
“I don’t accept the idea that life ends when you retire. The current generation won’t even retire in the same ways we retire. There’s going to be a group that is healthier, will live longer, and be conscious of what life they want to live,” he says.
“It’s about having a much more optimistic vision of what can be achieved later in life. And that can be achieved by not shuffling people off when they hit 70.”
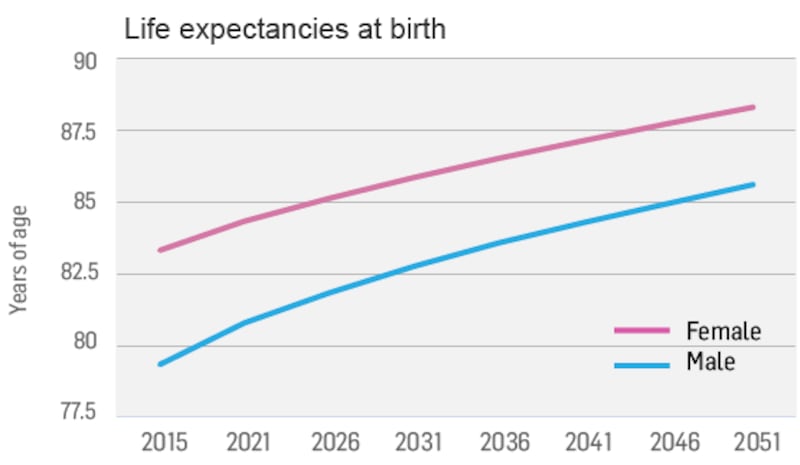
The Department of Health and the Department of Housing are working on developing a policy framework under which the Government could facilitate housing care for older people to deal with the increased pressures that will emerge as the older population grows.
In the meantime, the existing services for older people are facing considerable strain.
The HSE has a budget this year of just over €445 million to provide about 18 million hours of home support services to 53,000 people. Such services are either delivered by home helps directly employed by the HSE or by voluntary and private providers who have formal arrangements with the HSE.
At the end of June, HSE chief executive Paul Reid told the organisation’s board that the “level of demand cannot be met within the resource available”. At the end of April there were 6,310 people who had been assessed but who were waiting for funding for the provision of home support services. Reid said this included 4,646 new clients and 1,664 existing clients who needed additional services.
Providing services to encourage and facilitate older people to remain at home, including daycare facilities and meals on wheels, is not only considered to be beneficial to their own wellbeing, it is also far more cost effective for the State.
A bed in a public hospital can cost about €1,000 per day, and facilities taken up by those no longer requiring acute care add to waiting lists for treatment.
A place in a nursing home under the Fair Deal scheme will cost about €42,000 on average per year. While home supports may be more financially efficient, the rising costs have prompted questions on whether the current model can continue in the longer term.
Last summer. the Department of Public Expenditure specifically raised the issue of whether older people should have to pay some of the cost of home services themselves. It pointed to a report by the Health Research Board in 2017, which looked at home care arrangements in place in four European countries – Germany, Sweden, the Netherlands and Scotland – where patients contribute directly or through insurance.
“This contrasts sharply with Ireland’s case, where applicants are subject to a medical assessment but no means test. Moreover, in Ireland no flat-rate contributions are required for home care and most targeted services.”
The Department of Public Expenditure paper said the absence of cost-sharing arrangements for home care services, “raises questions on [their] financial sustainability”. The department’s findings have made their way over the last year to the heart of Government.
Daly said the introduction of a co-payment scheme for home supports was being given “active consideration”. Any such initiative is likely to come in tandem with an overall statutory scheme for the funding and regulation of home care which is likely to be announced at the start of next year.
Gaps in regulation
If Ireland is to shift the emphasis on ageing to the home, and in the community, top regulators want reassurances that they will be given powers to do their job effectively.
Phelim Quinn, chief executive of the Health Inspection and Quality Authority, tells The Irish Times that the toolkit available to his team “needs to change and it needs to change quite significantly”. The shift to home care, which is largely unregulated, would move “huge chunks” of older people beyond the regulator’s powers, he warns.
“There are vulnerabilities right across that spectrum, and we believe government needs to act to ensure they put safeguards in there,” he says. “We need to be thinking about that now, rather than later.”
He also calls on the Government to introduce legislation on adult safeguarding, which he says the State currently lacks. Introducing such laws would provide a further barrier to many of the financial, physical, psychological and sexual abuses older people are vulnerable to, he says.
He says there is a gap in the regulatory framework when it comes to safeguarding. “We work in the absence of any form of legislative framework for adult safeguarding in Ireland.”
“What we’ve got is a greater number of people entering health and social care services that are specifically vulnerable. I believe that is a huge challenge for the State and also a huge challenge for us as a regulator,” he said.
Whether the State can deliver high-quality, good-value care for a growing segment of the population remains to be seen.











