What is coeliac disease?
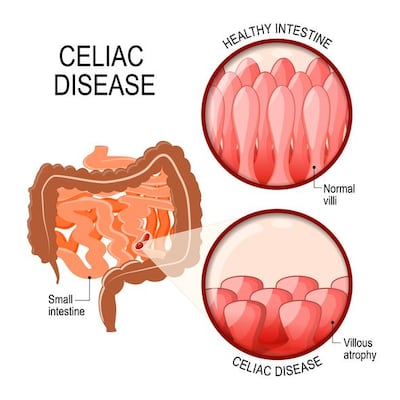
It is an autoimmune disease that causes an adverse reaction in the gut when an affected child eats gluten, damaging the small intestine. This should not be confused with gluten-intolerance, where an individual has a problem digesting gluten and may experience some similar external symptoms but will not have the same internal harm going on.
Wheat, barley and rye all contain gluten so, as you can imagine, it occurs in many common foods such as bread, pasta, biscuits, breakfast cereals, cakes, pizza, etc. But what you might not realise is that gluten can crop up in all sorts of other less obvious, processed foods, such as soups, sauces and chocolate bars.
Is a baby born with it?
Well, a child would certainly have to be born with the gene for it but that doesn’t mean he or she will develop the disease. An estimated 30 per cent of the Irish population carry genes for coeliac disease but it’s thought just over one in 100 actually has it. (We and the Finns are believed to have the highest global prevalence.) Ongoing research has so far failed to identify what triggers the condition – and that may happen in early childhood, the teenage years or not until adulthood.
What are the signs and do they differ, depending on age?
The earliest indications can come when you start to wean a baby, says dietitian Sarah Keogh of Eatwell who works with the Coeliac Society of Ireland. Once you start an infant on solids such as bread and pasta, if the coeliac disease is going to be triggered, you might begin to see looser nappies, more diarrhoea or, conversely, constipation.
“The problem with weaning is you are suddenly bringing in so many different [food] groups, that a change in nappies is quite normal,” she says. “But if the baby is getting a bit cranky, quite lethargic and their nappies have changed quite a lot, especially if there is any coeliac disease in the family, it is definitely something to go to the doctor with.” (If one of the parents has coeliac disease, it is recommended that a child is automatically tested, even if they are not showing symptoms, at age three years, six and nine.)
Slowdown in growth may be an indicator and this can become apparent if children's height and weight are tracked, says GP Dr Eamonn Shanahan, of Farranfore Medical Centre in Co Kerry. "If a child is failing to thrive and not putting on weight adequately, one of the things we would be looking at is that they don't have coeliac disease," he explains. The reaction to gluten affects the absorption of other nutrients in the gut.
Keogh echoes that point and suggests that a warning sign at home would be if your three, four or five year old is still fitting into the same shoes one year on. “It is not unusual for girls who have pains in their tummy to be told it’s anxiety,” she continues. “We have had girls who were sent to child psychologists and it was coeliac disease all the time. That doesn’t happen in boys – boys with pain in their tummy are picked up much quicker.”
For the tweens and early teens, delayed puberty could be another sign, along with bloating, diarrhoea, constipation. Tiredness and severe headaches are other common symptoms.
Is it easily diagnosed?
Well, yes and no. The fact that of the 50,000-plus people in Ireland who are statistically expected to have the disease, only about 15,000 have been diagnosed, indicates how “it is massively missed”, according to Keogh.
The problem is that the symptoms could be due to lots of other things as well so, as Shanahan says, “you need to have it somewhere in your thinking” to suspect it. He says that not only as a GP but also as someone who wasn’t diagnosed with coeliac disease until the age of 54.
“I would have had symptoms going back over the years, with tummy problems.” In hindsight, they were almost certainly due to coeliac disease but he had never been checked for it.
Once coeliac disease is suspected, a simple, two-part blood test is carried out to look for raised levels of the antibodies that an affected person produces in response to gluten. It’s really important you don’t stop giving your child gluten at the first mention of “coeliac”, at least not until the blood tests are completed, otherwise it won’t show up.
A biopsy conducted by a gastroenterologist from the small intestine will confirm the diagnosis but that is not always carried out in children if a doctor is satisfied that their blood test results seem conclusive.
“Part of the problem is that not every gut-related problem is due to coeliac and it is more from the point of view of ruling out other conditions that you would be doing the biopsy, making sure the person doesn’t have some other malabsorption problem,” Shanahan says.
How is the disease treated?
There is no cure and a child will never grow out of it, so it is a matter of managing it for life with a gluten-free diet.
“It is somewhat restricting but not massively restrictive,” says Shanahan. He would always refer a newly diagnosed patient to a dietitian, who will make sure they get a “gluten-free, balanced diet”, with emphasis on the word “balanced”.
“That’s the critical bit. It’s very easy to get an unbalanced diet but, if you are cutting things out of your diet, you have to make sure you are balancing it up somewhere else.”
Keogh, who still sees some children who were not referred on diagnosis by their doctors, says the diet is quite complex to get right. Parents need to bring their child to a Coru-registered dietitian for advice, not only around avoiding gluten but also on consuming sufficient calcium, vitamin D and other nutrients.
“Particularly if they have lost weight, you need to make sure the catch-up growth happens. There is a lot of monitoring for children and it is definitely not a thing you do on your own on the internet.”
Does it basically come down to reading food labels carefully?
Labels are certainly going to be required reading while you get the hang of things and whenever you want to try something new. Thanks to an EU labelling directive, all allergens contained in the ingredients of any pre-packaged food have to be listed.
However, the “may contain” that you see on some, alerting consumers to a risk of cross-contamination, is optional, explains Keogh. So even the most diligent perusal of labels may not ensure avoidance of gluten, if food is tainted at the place of manufacture. Without the right safeguards, cross-contamination is a danger with all food served in any cafe, restaurant or, indeed, private home.
A bit of gluten that fits on a pinhead can cause a reaction and, with severe diarrhoea and dehydration, a young child may have to be hospitalised, she warns.
The Coeliac Society of Ireland maintains a list of packaged food products available in Irish shops that are not only gluten-free but also certified as being without risk of cross-contamination. This essential resource for any family affected by coeliac disease has been harnessed for a user-friendly app, Minding Me Gluten Free, with features such as a barcode scanner for cross-referencing.
To help facilitate safer dining out for those with coeliac disease, restaurants that provide gluten-free food and can stand over their cooking and serving processes as safe are also being incorporated in a listing on the society’s website and app.
Many people say they feel better after going ‘gluten free’, so would we be better off just avoiding it as a family, even if none of us has been diagnosed as coeliac?
As a dietitian, Keogh is firmly against such a practice. “It restricts the diet and you don’t restrict somebody’s diet unless you really need to.”
Apart from the danger of missing out on essential nutrients, “it sets up a very strange relationship with food, which is unnecessary”.
What happens if a child with confirmed coeliac disease does eat gluten?
The reaction varies – at least outwardly. Only about 60 per cent of coeliacs will get sick straight away, according to Keogh. However, even if the other 40 per cent are not throwing up in front of you, the internal damage is still happening, she stresses. There is no such thing as being “slightly coeliac”.
Down the line, in adulthood, untreated coeliac disease is associated with an increased risk of bowel cancer, as well as bone disease, infertility, miscarriage and stillbirth.
Shanahan has never forgotten the case he encountered during his medical training of a woman who had been married for 10 years and had been unable to have children. At the age of 36, she found out she was coeliac, went on a gluten-free diet “and then had four children in four years”.










