Sometimes, the often overlooked side effects of cancer treatment can cause huge upset for people. For example, many patients struggle through the extreme exhaustion and nausea of chemotherapy but find losing their hair tremendously upsetting.
Similarly with radiotherapy, the short daily sessions of treatment are painless but the tattoo-like body marking necessary to position the patient so the radiation hits the tumour cells at precise locations can be a long-term reminder of the cancer that invaded their bodies.
Now, new high-tech equipment in St Vincent’s Private Hospital (available to private patients and in-patients at St Vincent’s University Hospital) means that these body markings are no longer necessary. And crucially, the scanning devices and cameras connected up to the new surface-guided radiotherapy machines allow more precise treatment.
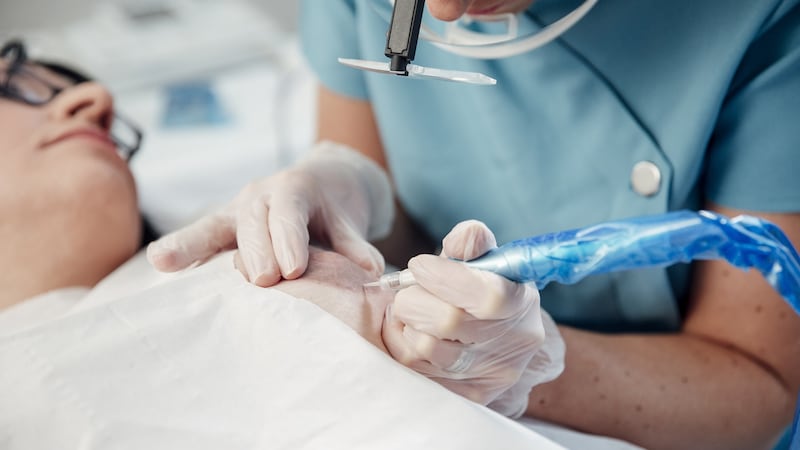
"Patients have a CT planning scan to design their radiotherapy treatment," explains Carol Bagnall, clinical specialist in radiotherapy at St Vincent's Private Hospital. Just before treatment, another CT scan is taken and superimposed on the original scan which has mapped out the location of the organs to treat. A camera also tracks the patient's movement throughout the session, ensuring precise delivery of radiotherapy based on the information from the two scans.
There is real-time imaging of the body while the radiotherapy is being delivered
If the patient moves slightly just before treatment, sneezes or coughs, the equipment is automatically switched off until the patient returns to a position for precise delivery of the radiotherapy beams. This so-called “surface-guided” radiotherapy has eliminated the need for body markings.
"There is real-time imaging of the body while the radiotherapy is being delivered, tracking the movement of the patient in relation to the CT scans," explains Patricia Flanagan, radiotherapy services manager at St Vincent's Private Hospital. The radiotherapy equipment, the plint the patient lies on and even a section of the floor can be moved to position the patient in the most accurate position for treatment.
Dr Gerard McVey, radiation oncologist at St Vincent’s Private Hospital and St Vincent’s University Hospital, explains that 60-65 per cent of patients require radiotherapy. “It is the second most common treatment after surgery and with many women having lumpectomy now instead of mastectomy, radiotherapy reduces the risk of breast cancer returning in the area we treat by 60-70 per cent,” says McVey.
The new radiotherapy equipment is being used for breast cancer patients only at the hospital, who make up about 30 per cent of patients requiring radiotherapy. “We decided to start with breast cancer patients because it can be very emotive for breast cancer patients to have these markings on their bodies. Some patients would have had them removed following treatment but, for others, they were a constant reminder of treatment,” explains Flanagan.
You lie on the bed with your arms over your head. You stay in position . . . and it's over in a few minutes
Fleur Campbell (47) is one of the patients who is having radiotherapy with the new equipment. "There is a lot of fear around cancer treatment and people think radiotherapy will be claustrophobic. But, it's very simple and straightforward. You lie on the bed with your arms over your head. You stay in position. You don't hold your breath and it's over in a few minutes. You don't feel anything while it's happening," explains Campbell, who has just had her 15th radiotherapy treatment, post-surgery and chemotherapy.
According to the latest clinical trials, fewer higher dose treatment with radiotherapy is preferable to more, lower dose sessions as was common practice 10 years ago. “Nothing stays in our body. It’s just like a high energy X-ray,” explains McVey. The side effects of treatment include tiredness for three to four months and a prickly heat rash.
“There is a 1-2 per cent risk of development lung or heart damage [for those with left-sided cancer] but this can take many years after the treatment to manifest itself,” says McVey.












