A normality of sorts is beginning to return to life at Mater Misericordiae University Hospital, in north Dublin. In the intensive care unit, or ICU, the machines that keep patients alive hum, beep and whirr. It is June 4th. Three consultants on the morning shift have their usual “corridor conversation” check-in, ahead of their formal ward rounds at 7.30am. Someone at the nurse’s station offers to make her colleague a bowl of porridge.
In the relative quiet of R4, one of the 18 glass-walled rooms on the ward, Alan O’Connor feels like he has just won the lottery. His 15-year-old son Glyn, the youngest person in ICU, has spoken a few words. Yesterday, he wiggled his toes.
Glyn was admitted on the Sunday in a critical condition after a farming accident the previous afternoon. Since then, he has spent nearly 15 hours in the operating theatre. “You’re a great man,” Alan is telling Glyn. He looks up from his son’s face, blinking in disbelief. “He’s an absolute miracle.”

There’s a sense on the ward that nobody is quite ready to use the word “relief”. The acute phase of the Covid-19 pandemic has abated, even if the virus hasn’t gone away. There are reminders everywhere of the lingering threat: in the omnipresent hand sanitiser units, the signs, masks and soft swish of the PPE staff don to enter into one of the five rooms occupied by patients with Covid-19.
Still, over the last couple of weeks, there has been a shift in focus back towards “the non-Covid patients”, says Dr Colman O’Loughlin, consultant in intensive care medicine. “We’ve people from 15 years of age, right up to 80 years of age, coming in with a huge range of problems.”
Most of the 70 ICU beds secured in the early days of planning for the pandemic – almost doubling the combined capacity of the ICU and high-dependency unit – were not mobilised. Of the more than 800 Covid-19 patients treated in the Mater hospital, 52 ended up in ICU. Unless there is a second surge in the autumn, those extra beds won’t now be needed. Whatever relief is there is also tinged with concern about the ongoing medical, psychological and social fallout from the lockdown. The crisis has almost passed. The new normal is here. But nobody is yet sure what that will mean for staff, patients and society.
The ICU consultant
“A lot has been unveiled by this crisis,” says O’Loughlin. “It’s going to take a long time to get back to what we think will be a new normality, but it will be very different I think.”
He was on call last night – there was just one call, at 11pm – and arrived at the hospital before 7am to begin the day shift. “At any given time, we probably have around 30 to 34 patients between the two units,” he says. There are 30 patients here today. “So it’s business as usual, as much as possible. Covid is a diversion. But there’s a world of other stuff that will not go away, ever.”
The early weeks of the crisis were a rollercoaster of fear and anxiety. “The anxiety levels peaked when our first staff member was tested positive. People were visibly very upset, people were crying. I don’t ever think I’ll forget that.”
The staff member became seriously ill and was ultimately admitted as a patient to ICU. “We’re used to dealing with very difficult, very emotional scenarios. But when it’s ourselves, when it’s our own staff members – our very core – being attacked by this virus, it is difficult,” says O’Loughlin.
“The confidence curve just nosedived. The strength that the intensive care teams showed at that time was just extraordinary. They didn’t run away and they didn’t hide. They stood up and were counted.”
The first staff member who became ill recovered in time, and others got sick, but most were able to stay at home. Gradually, staff at the Mater and their colleagues around the world began to learn more about this frightening new virus. Even in the most severe influenza epidemics, “we wouldn’t see anything like the severity of the lung injury. This is a level of disease we’ve never seen before.”

Now with the numbers of sick falling, the attention of the staff at the Mater is turning to the consequences of lockdown; what O’Loughlin calls “the collateral damage”. He cites symptoms of bowel cancers and heart complaints that have been ignored, or “older people coming in with appendicitis that they haven’t got seen because [they think] ‘it’s just a tummy bug’ ”.
Other parts of the hospital were “a ghost town” at times during the peak of the crisis. “You could have played five-a-side soccer down in the emergency department . . . There were days when maybe five or six people turned up. Normally, you’re talking up to 250 a day, or 80,000 people a year. Those patients didn’t go away; they just came later. And that’s what we’re dealing with now.”
The return to normal medicine is “the next huge problem that we’re preparing for – more so than a second surge of Covid”. He’s worried also about “the psychological effects of lockdown”. In ICU “we’re seeing far more than normal self-harm injuries. Patients who just couldn’t cope with social isolation. They just about have the ability to cope when things are normal. When you take away their normality from them, their ability to cope can just disappear.”
Some of those who have been admitted to ICU with self-harm injuries had previously diagnosed mental health conditions. But others did not.
O’Loughlin applauds the job the public health experts and the public themselves did during the lockdown. But he hopes never to see it again. “My children never want to see it again.”
The ICU patient: Glyn O’Connor and his father, Alan
Glyn O’Connor is hooked up to monitors and oxygen, conscious but not fully alert. Beside him, his father, Alan, looks shellshocked.
Four days earlier, Glyn was on a farm in Cappoquin, Co Waterford, taking stones from a field and throwing them into a loader that was being pulled by a tractor. "I don't know the exact happenings, but Glyn tripped up and fell under the wheels of the loader. They basically went straight over his body and broke his ribs, pelvis, lower spine and his femur." His lungs were punctured.
“I got a phone call from my nephew who was with him. I was in the field within two, three minutes . . . By the time I got to the field, Glyn was coughing up blood.”
He was transferred to Cork University Hospital by air ambulance and Alan followed. “They said you need to get someone here. He may not make it.” Five hours later, at midnight, a doctor came out to see Alan on the bench where he was trying to get some sleep. “They said to me, ‘he’s still here.’ ”
The following day, Sunday, Glyn was transferred to the Mater for the first of several surgeries to stop the internal bleeding. Further surgeries to stabilise his pelvis and lower lumbar spine followed on Tuesday. Alan and his partner Treasa Gough haven't left his side since.
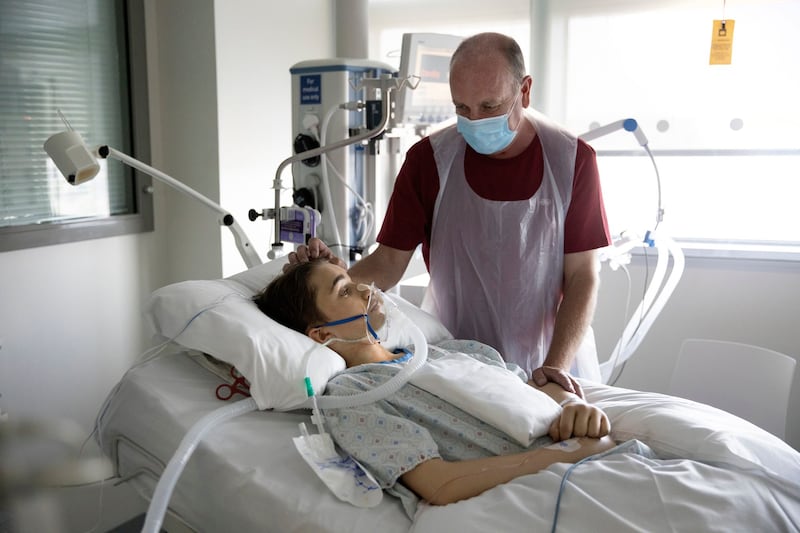
“Yesterday was Wednesday. He woke up and wiggled his toes. That was the most fabulous feeling, you know. It’s all you ever ask for. Every day this week has been a lottery win for me. The legs were the worry, and suddenly he’s moving his toes. Today, he’s talking to me.” He used to give out to Glyn for being on his PlayStation; now, he says, he’d love nothing more now than to see him back on his PlayStation.
I ask about Glyn being able to move his toes, and immediately, there is movement at the foot of his bed. “He’s moving his toes for you.”
Glyn says something to his father. Alan leans in and listens intently. “He’s a bit uncomfortable,” he says. We leave and a nurses arrives – each patient in ICU has one-to-one nursing care – to settle him.
I speak to Alan and Treasa again a week after our first conversation. Ten days after Glyn’s accident he is out of ICU, into the spinal unit where is having physiotherapy, is fully alert and remembering everything.
They believe that, in a sense, the Covid-19 crisis saved Glyn’s life. It meant there was no delay on the emergency services and it allowed him to move through the hospital system much more quickly. It meant that “people who didn’t need to be in hospital weren’t there. The accident was horrific, but the timing was lucky. His luck started two seconds after the accident,” says Alan.
“If the accident had happened before coronavirus, the ICU units would have been up the walls,” Treasa says.

“It’s very interesting to hear that perspective,” says O’Loughlin. “The support service they needed arrived quicker. The hospital journey for them was very, very smooth and there were no barriers to admission. Sometimes we see it in from the other side – that things get delayed, not by unnecessary precautions, but when more timely precautions could have been taken.”
Glyn’s mother, who died when he was two, was also looking out for her son, Alan says. “I was saying prayers to her to keep him, to leave him here with us. And he’s still here. He’s coming home . . . They’re miracle workers here. They saved this boy.”
The recoving Covid-19 nurse
ICU nurse Bindu Sam Cherian was contacted by the Health Service Executive to tell her that she had been exposed to Covid-19 at work. She didn't need to wait for the results of the swab to know she had it. The same night, she developed a high fever. Within a week, her husband and four children were sick too. "It was difficult, it was scary. Always I was thinking of how to get back to work, because my colleagues needed me."
The first week of the illness “was incredibly painful. Coughing, very strenuous coughing. Fever that would not subside except for a few hours. We had sleepless nights, sitting up coughing all through the night.”

She was frightened for herself, her husband and her children. “Being an ICU nurse, you think of the worst. I was thinking of all the signs and symptoms, and I was watching them like a hawk.”
But her children mostly suffered from aches, pains and loss of taste and appetite.
Her colleagues, neighbours and church group rallied, leaving food on the doorstep. “This made us think like everybody is supporting us. We all are in this together. The whole world is suffering. And we will all overcome this.”
Now, after a month back at work on the ICU ward, she still gets breathless if she tries to stand for too long while she’s talking. Was she scared? “Yes. I was scared. And I think I’m one of the few lucky ones who managed to be isolated at home and recover.”
The infectious disease doctors
Matthew Blair, an infectious disease registrar, takes us into the isolation unit at the Mater, which is serving as one of three Covid wards. There are six isolation beds here, which in normal times would be reserved for patients with disease like tuberculosis and ebola.
Blair explains that every time he goes into a patient’s room, he has to don a full new set of PPE, putting it on outside the negative pressure doors, and waiting for a green light to signal that he can enter.
“And then after seeing the patient, there’s an exit room where you doff the PPE and wash hands and then you can leave here. So that adds on an extra 10 minutes to your consultation. You’re certainly able to see less patients than you would.
“Initially I remember seeing my first Covid patient and certainly I was quite nervous and extremely careful.” Now, it’s “muscle memory”.
What does he think the biggest misconception about Covid-19 is? “I would be slow to say that this is a mild disease,” he says carefully. “I’ve seen enough cases of young people, healthy people with quite severe illness, progressing to critical illness and requiring intensive care.”

The pandemic has meant "a lot of long hours for quite a number of weeks and months now" for everyone at the hospital, says Jonathan McGrath, an infectious diseases doctor on another Covid ward. "All we've been doing is going to work, going back home, and repeating, since very early March."
He is the doctor who admitted the first patient to the Mater. Alongside the inevitable exhaustion, there’s a sense of “worthwhile purpose . . . a specific goal in mind for everybody across the hospital” that keeps the staff going.
What has made Covid-19 more frightening than other infectious diseases is that “it was a moving target. It was a challenge, but also an opportunity to learn as you go with it.”
The volunteers
Around midday, the buzzer goes on the door that leads into the ICU units. Today's food delivery from the Feed the Heroes initiative is here. There are scones, salads, curries and pastas from Hanleys Clean Meals, brought in by husband-and-wife team Andy and Catherine McEntee, who are on the road delivering food to hospitals seven days a week. "This is our third hospital today," says Andy.
Kay Winters, who is part of the hospital administration staff, crosses paths with them in the hall with another delivery – her's is from Microsoft. It is a selection of stews and vegetarian meals.

The Feed the Heroes initiative is finishing up the day after we meet, and when it does it will have served up 185,000 meals to hospital workers and raised €1.3 million in donations. “In the beginning this gave such a lift to the hospital. Now it’s nearly become normal. Everything becomes normal after a while,” Winters grins. “They’ll miss it.”
The psychiatrist
"I wouldn't say it's normal yet, but certainly, we've adapted," says consultant psychiatrist and clinical director for the approved centre for psychiatry at the Mater, Guy Molyneux.
The lockdown has hit areas like Dublin’s north inner city hardest, he says, and the homeless population is the most severely affected. “We have noticed over the last two months an increase in admissions [to the psychiatry unit] of people with homelessness. Quite often, it’s just that they’re not coping with the fact that they’re so restricted.
“There’s not a lot to do in the inner city, and they’re not even meant to be walking around that much; they’re meant to be staying in the hostel. We’re finding that people are coming into hospital feeling suicidal, or with psychosis as a consequence of increased drug misuse.”

He is concerned about the mental health impact of the “loneliness, isolation and anxiety” across society in general. But he acknowledges the dilemma at the heart of the public health response.
“We’re all aware of the fact that lockdown is having an impact on people’s mental health. But we’re also aware that Covid-19 is a very significant illness that not only can make people very sick, but can kill them. Already the patient cohort that I’m involved in are at risk of dying 20 years earlier than other people in the community.”
The oncology nurse manager
"Staff come in for breakfast, lunch and dinner. They don't circulate around the hospital. They don't socialise with other staff." Tracey Fitzpatrick, nurse manager at the cancer directorate is describing the "lockdown within a lockdown" on the 32-bed St Vincent's ward. Here, as everywhere, we sanitise hands and change our masks for new ones but as an extra precaution she asks us to leave our bags outside the ward.
One of the things she is finding tough is not being able to give patients a hug. “We’re so used to being able to use touch, to put an arm on somebody, sometimes in celebration of good news, and sometimes in a reassuring way to express empathy to them.”
This period has been “a time in my career when I’ve learned a lot about myself. I’ve learned how resilient I can be. I’ve learned that I can be frightened. And I’ve learned to rely on other people.”
The oncologist
Prof Michaela Higgins meets us via Zoom, because she can't be in the hospital today. She is at home awaiting the result of a Covid screening, after she came down with a sore throat which she suspected was hayfever. "I'm doing the right thing, which is to err on the side of caution." (She emails later to deliver the happy news that she is Covid-19-free.)
Back in March, to protect patients, the entire chemotherapy day patient service was transferred over a weekend to a separate building across the street, which is normally home to the nursing training centre. “We spoke to portering, security, pharmacy, cleaning, catering, and everybody said right, ‘how do we do it?’ They came in on their days off and literally wheeled chairs across Eccles Street,” says Higgins.
In the beginning, “we thought this would be a short, sharp shock . . . a three-month period of a very overwhelmed system. Now, as the weeks and months go by, we’re learning that this is something we have to manage for quite a period of time.”

Two months on, “we have continued to treat over 40 patients a day, from Monday to Friday. They’re getting their chemotherapy treatments, they’re really relieved that their cancer care is continuing. And as I sit here today, no new patient coming in for treatment has picked up Covid-19 . . . Many of our new patients are relieved. They come in and say, ‘oh, I am so glad I thought you wouldn’t treat me.’ We’re able to say, of course, we will look after you.
“We are still here. We’re still working. You will be treated for your cancer. We might look a little different, but you will still get your care.”
Services may have to be flexed up and down again if a second surge comes in winter. “But I’m not frightened at all. I know that we’ve got this.”
The cancer patient
Charles O’Connor is in for his treatment for his lung cancer today. He has been coping well with the double whammy of chemo and lockdown – if anything, it has made lockdown easier.
“I have a large garden, so I’m quite entertained in my own little cocooned world. We’re getting through it quite well. The effects of chemo are tough enough, that even if you had a normal situation, I don’t think I’d be up to much.”

He has surprised himself by how well he’s taking his diagnosis. “I can’t believe that I have a terminal illness. And that’s why I’m kind of functioning so well.”
What he’s most looking forward to when he gets out the other side of all this is a game of golf. “If I could get the energy back, I’d love to get out for a game of golf. And I think socialising with my family, being able to have friends up or just have meals together again. That’s all really.”
The social worker
In her office downstairs in the Mater, principal medical social worker Amanda Casey describes the very particular challenge of providing end-of-life care to patients during a global pandemic. "Obviously with Covid, end-of-life care has become much, much more difficult."
Limitations to visitor numbers means that patients – even those who don’t have Covid-19 – are not able to have their families with them during the end stages. Sometimes, “one family member, if they are in full PPE [might] have permission to come in”, but it isn’t always possible to make that happen during a patient’s final hours.
So nursing staff are stepping in, doing what they can to make sure someone is with the patient when they die. “It makes a massive difference to the person at home who gets the call if someone can say, ‘I was there’.”
Casey’s team have also been setting patients up with donated digital devices, so they can connect with family via Zoom, Skype or WhatsApp. “One of the biggest fears that [family members] have is they can’t physically see the person. You can say, ‘yeah, she slept well’ or ‘she ate today’ or ‘she is a bit weaker today’, but not being able to physically be there with someone, I think, must be terrifying. So at least if they’re able to physically see them; it’s some way to making it feel real . . . At least it’s giving people the opportunity to maybe say their goodbyes.”
For the patient too, no matter how unwell they are, “just being able to hear the voice of their spouse, being able to talk to them and reminisce with them, has an impact on the person in the hospital, makes them calmer and more at peace. Being able to bear witness to that is really, really profound.”

















