1970 was the year of the Arms Trial, escalating violence in the North, and a six-month bank strike. Apollo 13 told Houston it had a problem. Nixon came to visit. And Dana was singing about "all kinds of everything".
Many of the year’s health stories, however, seem all too topical a half century later: rows about hospital sites and sizes; protests about pay and conditions; the private versus public care debate; concerns about cervical smear tests; and promised – but unfulfilled – reforms.
As the year began, an influenza outbreak was on the wane. Front-page reports on New Year’s Day flagged a potential new vaccine, but confirmed eight further deaths. Doctors predicted that between 30-40 per cent of the population would become ill.
January finally saw the first 12 patients admitted to the new St Vincent's Hospital at Elm Park, Dublin. Talks about moving the hospital from St Stephen's Green had begun in 1934! Officially opened in November, it was the largest new teaching hospital to be commissioned, in Ireland or Britain, since the second World War.
Under the recommendations of the Fitzgerald Report on hospital services, St Vincent's became the regional hospital for Dublin's southside; "with another hospital, on the site of the Mater, to be its equivalent on the northside. Two general hospitals are also planned: one at Blanchardstown and the other on the site of St Kevin's hospital between Inchicore and Rialto. All the other city hospitals were to be phased out."
However, by February, there was: “a large body of opinion that has grave misgivings about the size of the Mater Hospital site”, with some Dublin architects suggesting that there “is not sufficient room to build the hospital, while allowing for ancillary services and such facilities as car-parking space”.
Meanwhile, after 30 years in the pipeline, draft plans for a 550-bed regional hospital at Wilton in Cork were completed in February. "Cork's medical services have suffered from a far greater inadequacy of buildings even than those in Dublin," wrote our medical correspondent.
Hospital developments were taking place in tandem with the implementation of the Health Act, 1970, which allowed then tánaiste and minister for health Erskine Childers to make radical changes throughout the country's health services.
Controversial proposal
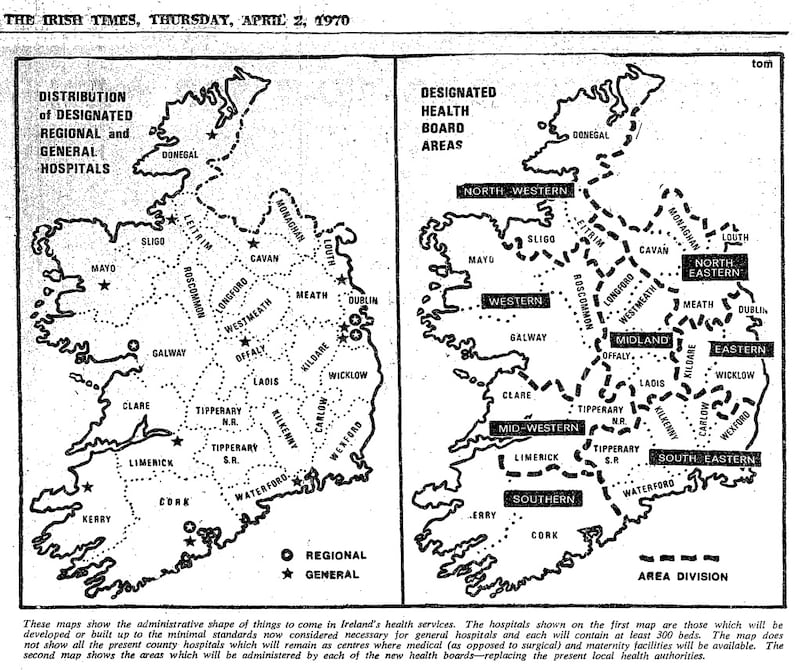
Those changes included the division of the country into eight Health Boards – instead of 27 health authorities. One controversial proposal was to limit surgical services to nine hospitals outside of the university centres of Dublin, Cork and Galway. Only medical and maternity services would be available at county hospitals, but surgeons and “super specialists” would travel to outpatient departments.
Objections were inevitable, such as the resolution passed by the Irish Medical Association at its April AGM, which "deplores any proposal to reduce hospital facilities in Wexford". In an interview with health correspondent David Nowlan, Childers rejected suggestions the reforms would cause rural decay. "Local hospitals can, ought and will still be used for convalescence," he said. "The travelling around the country of teams of consultants for out-patient sessions is of far more importance than the retention of a surgeon in a particular local hospital."
The minister’s vision included a helicopter ambulance service for remote areas, hostels for old people to live in, day-care facilities for psychiatric patients, and a new pre-school health service, which was piloted in October with health checks for six-month-old babies. A reduction in the length of hospital stays was also high on his priorities. This may have been prompted by reading Maeve Binchy’s February discourse on her gall-bladder operation, which featured a three-week convalescence, surrounded by gin-swilling visitors.
The continued expansion of services came at a cost. The March prize fund for the 119th Irish Hospital Sweepstake surpassed £2 million, but in April the Dáil heard “there were now no reserves in the Hospitals’ Trust Fund. Its current income from sweepstakes was not sufficient to meet commitments . . .” Expenditure on health services had increased from £18.5 million in 1958/59 to £61 million in 1969/70.

‘Wholesale exploitation’
The reforms sparked other debates. In the Seanad, Fianna Fáil’s Bernard McGlinchey warned there was nothing to prevent the “wholesale exploitation of the Irish medical service”. The only solution, he insisted, was not to allow private beds, or specialist’s private rooms, in local authority hospitals. “When we reached the day that specialists were paid a salary and did not depend on private patients, then and only then could we say that we had a fair medical service. In this country, if a medical card-holder wished to avail himself of clinical service he was placed on a waiting list for two, three or four months. If a person wished to pay the specialist in a private capacity that appointment could be arranged within one week, Was this a just system?”
The present conditions of service for young doctors in Irish hospitals are so unattractive that they would prefer to emigrate than to stay at home
Another criticism levied at the Department of Health, this time by the Irish Cancer Society, was its failure to introduce a smear-testing service. And in April, a new national service for "pap smears" was launched at St Luke's Hospital, Rathgar. It offered free equipment and laboratory facilities "to all G.P.s who care to apply, so that every woman in the country can be tested at minimum cost or no cost at all . . . Results come back within a week, or in country areas it might take a fortnight."
In May, a long-running dispute with the country's junior hospital doctors, over salaries and working conditions, culminated in strike notice. One key demand was that they "should not be expected to work more than 70 hours in any one week. (At present many of them work between 100 and 140 hours a week if time 'on call' is taken into consideration.) According to Dr Noel Reilly of the IMA, "the present conditions of service for young doctors in Irish hospitals are so unattractive that they would prefer to emigrate than to stay at home".
It is inevitable that we will meet opposition to some very sound ideas on healthy living because they will clash with established interests
An interim agreement included salary increases, and a working party to consider the conditions of junior hospital medical staff, their career structures, and postgraduate education.
1970 was a “year of militancy” for nurses, who marched in protest for the first time. They were looking for improvements in basic salaries, staffing levels, conditions and pensions. They also protested at delays in implementing a 40-hour working week, and patient conditions in hospitals.

In March, the Medico-Social Research Board's main concern was to stop the dead being buried without a doctor's or coroner's certificate. Its director, Dr Geoffrey Dean, said the board also needed to act as a medium for publicity about healthy living: "The great dangers to health of cigarette smoking and the need to curtail the advertising of cigarettes and alcohol, weight control and the restriction of the amount of animal fat in the diet, exercise, etc. It is inevitable that we will meet opposition to some very sound ideas on healthy living because they will clash with established interests."
One such clash occurred when managing director of Bord Bainne Joseph McGough persistently interrupted a meeting, trying to prevent Dr Risteard Mulcahy, chairman of the Irish Heart Foundation, speaking about possible links between animal fats and coronary disease.
Cigarette and alcohol advertising
Cigarette and alcohol advertising was still a feature of this paper, while in February, the minister for health told the Dáil that compelling tobacco manufacturers to carry a warning on packets about the dangers of lung cancer, bronchitis and heart disease "would have little or no practical effect". However, in June, the World Health Organisation cited packet warnings, and elimination of advertising as measures to stop tobacco use. And the chairman of the National Working Committee on Drugs, Dr Karl Mullen, declared that cannabis smoking was "not as injurious as cigarettes", or "as bad as drinking, which is the greatest evil in this country".
In February, Dr Mullen described Ireland’s drug problem as “still a minor one”. There were two main groups who abused drugs. The teenagers of the first group were mainly underprivileged socially and educationally. There were about 70 hard drug takers in the country, the majority being under 20 years of age. The second group, he said, were the “quasi-intellectuals who smoked cannabis and were of higher social class. They had no law-breaking tendencies and rarely came under the notice of the gardaí.”
According to Dr Dean of the Medico-Social Research Board, a much more serious aspect of drug abuse, was “the taking of barbiturates and tranquillisers under prescription from doctors. Enough barbiturates and tranquillisers had been prescribed in the Republic of Ireland last year – 36 million doses in all – to supply 12 per cent of the total population with these drugs three times a day for the year.”
In September, The Sixth World Congress of Cardiology “favoured a slow and cautious continuation” of heart transplant procedures – 170 cases of heart transplantation had now taken place worldwide, though fewer than 25 patients had survived.
It is not generally appreciated in Ireland that bad oral health and hygiene are socially unacceptable in many European countries and in the <a class="search" href='javascript:window.parent.actionEventData({$contentId:"7.1213540", $action:"view", $target:"work"})' polopoly:contentid="7.1213540" polopoly:searchtag="tag_location">United State</a>s
And in August, after much debate, the 24th World Medical Assembly passed "the Declaration of Oslo", a statement on therapeutic abortion in: "Circumstances which bring the vital interests of mother into conflict with the vital interests of her unborn child . . ." Dr Phillip Cawley, representing the IMA, supported the statement. The fact there was unlikely to be any liberalisation of the abortion law in Ireland "did not mean that Irish doctors were unconcerned in this matter", he said. "The fact was that Irish women who wanted abortions were likely to go to Britain where it was available to them and all of these women would be the patients of Irish doctors."
Contraception
Contraception also featured regularly in the news. In April, legal correspondent David Goldberg described the law on contraceptives as "a pathetic pretence", following reports that Customs and Excise officials had seized packages of spermicidal creams sent from Britain. "Spermicides are essential in the use of diaphragms as a contraceptive device; while the diaphragms themselves are getting through, spermicides have not."
In theory contraceptives – including the pill – could be prescribed by doctors on medical grounds, but the law prevented their import and sale. However, even therapeutic contraception was not a reality for many Irish women. In October, Prof WF O'Dwyer of Jervis Street Hospital called for a "realistic family planning service" to save mothers who "should not, medically speaking, be allowed to become pregnant again". And in December, the newly formed Irish Family Planning Association sought the repeal of laws against contraception "on the grounds that they are repugnant to the United Nations declaration on the subject".
Other 50-year-old health stories include a warning that Irish smiles were repelling tourists, "as a regrettably high proportion of these smiles were ravaged with disease". "It is not generally appreciated in Ireland that bad oral health and hygiene are socially unacceptable in many European countries and in the United States, " dental surgeon EJ Little told students from Shannon's College of Hotel Management.
The disabled parking symbol was also issued for the first time, to members of the Irish Wheelchair Association, allowing some privileges – at the discretion of gardaí – for parking in no-parking zones, and "to park at parking meters without having to insert the normal fees".
Other topics occupying our health correspondent included: the launch of a vaccine against German measles – rubella – which would reduce still-births and birth defects; a ban on the use of cyclamates – artificial sweeteners – in food and drink; and skin reactions to modern “biological detergents” .
This topic was also taken up by the Irish Housewives’ Association in a Letter to the Editor: “We have had reports of severe skin complains as a consequence of immersing hands in water containing enzyme washing powder.” Calling for further research from manufacturers, the authors urged housewives to wear rubber gloves.
Finally, taoiseach Jack Lynch was among the statesmen and industrialists who contributed to research for a new book – "the first of its kind" – on Human Circadian Rhythms, co-authored by Professor Conroy of the RCSI. "The book gives detailed reactions from a number of people on how they felt after travelling long distances, crossing the date-line – by air – and the effect of disorientation on business executives from such journeys and their decision-making abilities."










