The Health Information and Quality Authority (Hiqa) national patient survey maps out the journey Irish patients take when they are admitted to hospital. What makes this survey especially useful is the prominence given to patient’s own narratives and what they reveal about the health service.
Patients who were discharged from one of 40 acute public hospitals in May and spent at least 24 hours in hospital participated in the survey. Some 13,700 people responded from all parts of Ireland; they identified eight major areas of the patient journey that need improvement.
Unsurprisingly, hospital emergency departments come top of the list. But there were also significant deficits in areas such as the communication of test results and the availability of staff to discuss patients and relatives’ concerns.
Emergency department (ED) experience:
“Waiting time in the emergency department is terrible and unacceptable. One doctor on duty is unsafe for both patients and doctors.”
While there are many comments praising ED staff on their heroic work in abysmal conditions, some 70 per cent of respondents who came into hospital through the emergency department said they waited longer than the target time of six hours before being admitted to a ward. This represents a very real threat to patient safety.
Patient communication on the wards:
“I feel it would be very important to have a better support system to talk about the fears and worries I had due to my serious condition. No one had time.” Almost half of those surveyed said they could not always find a member of hospital staff to talk to about their worries and fears. While the chronic understaffing in Irish hospitals is the main reason for this finding, not having your fears listened to as a patient is a significant deficit that must be addressed.
Discharge from hospital:
“ Before leaving the hospital I wish I had been given a printed sheet with all the information I should know for aftercare once I got home.” Some 46 per cent of those surveyed said they were not given any written or printed information about what they should or should not do after leaving hospital. This is not rocket science and could be quickly remedied by the HSE.
The bridge between hospital and home:
“I had major surgery and was naive about the level of care and the effects that the medication would have when I went home. I live alone and I felt this could have been explained better.”
Some 43 per cent said they did not receive sufficient information to manage their condition after they were discharged from hospital. Again this is unacceptable and increases the likelihood of someone needing unnecessary readmission to hospital.
Information for family members:
“Keep patient and family more informed about what’s going on. My children felt that they were told nothing and constantly had to ask.”
Just over four in 10 people said their families or people close to them did not always have sufficient opportunities to talk to a doctor. While some instances of perceived poor communication with family members may reflect patient confidentiality, where patients request that relatives are kept in the loop, this must be facilitated.
More time, please, doctor:
“The time the doctors spent at the bedside was far too quick. Sometimes I would be half asleep and miss what I was being told so I was left feeling rushed and anxious. I know the doctors are busy but a bit more time would have made understanding what I was being told easier.”
Forty per cent of those surveyed said they did not always have enough time to discuss their care and treatment with a doctor. There is clearly a need for doctors to listen more and spend more time interacting on a one-to-one basis on the wards.
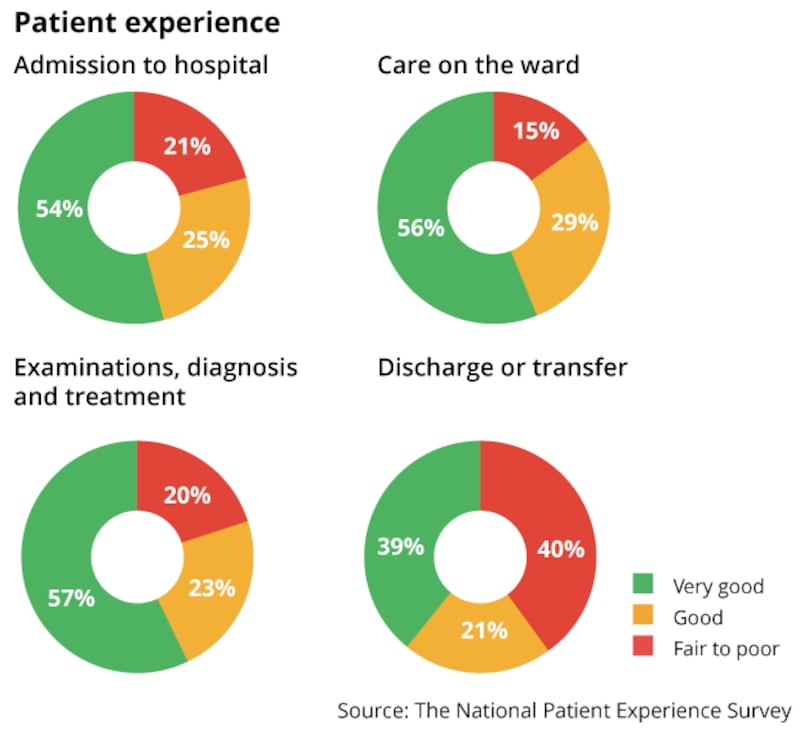
While the main purpose of the exercise is for Hiqa to identify areas of patient care that can be improved, it is important to acknowledge the high levels of overall satisfaction expressed by patients for healthcare professionals in the survey. With the exception of their transfer of care and discharge, more than 80 per cent of people rated their care in acute public hospitals as good or very good.










