In his second article for ‘The Irish Times’, Conor Lane, a young Irishman who was diagnosed with a rare cancer in London, writes about the major surgery that saved his life.
On February 1st last, I was in a London hospital ward, wearing a gown, having surgical lines drawn on my back and waiting to be rolled into theatre.
My operation had been scheduled eight months after I received a diagnosis of Ewing’s sarcoma, an extremely rare cancer more commonly found in children and teenagers. That night, I expected to be cancer-free.
I was 25 years old and had been working as a paid intern for CNN World Sport in London when my shocking diagnosis had come out of nowhere. I had experienced some persistent but minor chest pain and an X-ray revealed a “massive pleural-based right lower zone mass”, with urgent respiratory response required.

A frantic few weeks of tests and scans ensued, and on June 1st last, I began aggressive chemotherapy at the Macmillan Centre of University College London Hospital (UCLH), followed by radiotherapy, to shrink the 15cm (6in) tumour in my chest.
Now I was in the Princess Alexandra Ward at the Royal Brompton Hospital, ready to have what was left of the tumour removed. I was anxious but not afraid and had been mentally preparing for the discomfort and pain. But at the 11th hour, a sombre-looking surgeon told me the last thing I wanted to hear: my surgery had to be cancelled.
"Four weeks?" I heard my mother ask. Mr Simon Jordan, consultant cardiothoracic surgeon and chair of the cancer team, nodded. He stood at the bottom of my bed and carefully explained that my CT scan had revealed inflammation on my right lung (pneumonitis), caused by the radiotherapy I'd completed in November. There was too great a risk of infection for him to carry out the surgery that day because if I got infected, they would likely have to go back in for a second surgery.

Up to that point, I had endured 11 rounds of aggressive chemotherapy, which caused baldness, loss of appetite, fatigue, mucositis (painful throat inflammation), fevers, regular trips to A&E in the middle of the night, seven blood transfusions to boost my red blood cell counts and a mental fuzziness that patients sometimes refer to as “chemo brain”.
The radiotherapy had produced a horrible cough that lasted for two months. Enough was enough. It was time to get the tumour, which had shrunk to one-third of its original size, out of my chest.
But instead of having my surgery, I left hospital with my mother, disheartened, and with a sickly feeling. I completely trusted the decision of my multi-disciplinary team, but I was frustrated.
Little did I know that a bigger shock was to come just two days later when I saw Prof Jeremy Whelan, consultant medical oncologist at the UCLH Macmillan Centre. Having been in charge of my case from the outset, he knew better than anyone about what should happen next.

“We’re suspending your treatment, Conor,” Prof Whelan said, while I contemplated what that meant. I would not be having any more chemo. It was hard to process. Surgery cancelled, chemo suspended. What was going on?
If my surgery had proceeded, I was supposed to have had three more “maintenance” chemos over the next nine weeks, a fact that I had accepted. It was a bittersweet moment. On one hand, I was suddenly free from this toxin and on the other, I was caught off-guard and very concerned. What were the repercussions of not completing the original treatment plan?
Good prognosis group
He explained that there was no evidence to suggest that continuing with chemo would be of any benefit. I had successfully navigated my way through six cycles of VIDE, which many people cannot tolerate. I was still considered to be in their good prognosis group. The team had told me repeatedly that I was doing very well. But due to the surgical delay, I would have been without chemo for 11 weeks and restarting it for three more cycles was going to have a negligible effect, Prof Whelan said.
To reduce the lung inflammation, he prescribed heavy-duty steroids for the next four weeks. It was a “massive dose”, according to my hospital discharge letter. The steroids made me anxious, lowered my immunity, gave me muscular cramps and interrupted my sleep, but I took them consistently, knowing they were a means to an end. No pain, no gain.
The week before my rescheduled surgery, I travelled to see my parents in Achill, Co Mayo, to enjoy some home-cooked meals and relax. It was only my second time back in Ireland since my diagnosis because the risk of infection had been too high and my general condition too poor to travel during the previous eight months. Although I lived in a flat in central London, I really was tethered to the facilities at UCLH Macmillan, so even being allowed to fly to Ireland was a relief.
Four weeks passed and March 1st finally arrived. With a cancelled operation under my belt, checking into hospital felt smoother the second time around. Scans showed that my lung was still inflamed but had improved.
Around 6.30am, I was awakened to have lines drawn on my back again, to shower and to get ready. The anaesthetist came in and explained exactly how I would be put under, adding that she’d be monitoring me for the whole surgery. It was reassuring.
This time they were going ahead.
the pain in the area where they had operated was immense
Within seconds of the anaesthetic being administered, I was out like a light. I woke up about five hours later in the recovery room, with several people surrounding me, looking to see that I was all right. I had tubes and wires in my chest and neck. Instinct was telling me not to move at all because suddenly, I was semi-disabled and the pain in the area where they had operated was immense.
Tumour removed
Mr Jordan and his team removed the cancerous tumour, a section of my fourth rib and sections of my fifth, sixth and seventh ribs on my right side. Parts of four ribs, in total. As they said all along, they wanted clear margins and they did not compromise. Mr Stuart James, clinical lead for plastic surgery at the Royal Marsden Hospital, next door to the Brompton, moved my Latissimus Dorsi flap (the LD flap is used in reconstructive surgery) from my back, up under my shoulder and over my pectoral to cover a mesh prosthesis inserted into my chest to replace the gap in my ribs.
The LD flap was used because it would help to create a new eco-system in my chest. It has its own blood supply and would assist my body in accommodating the mesh, which is a light, life-lasting material held in place by a layer of cement.
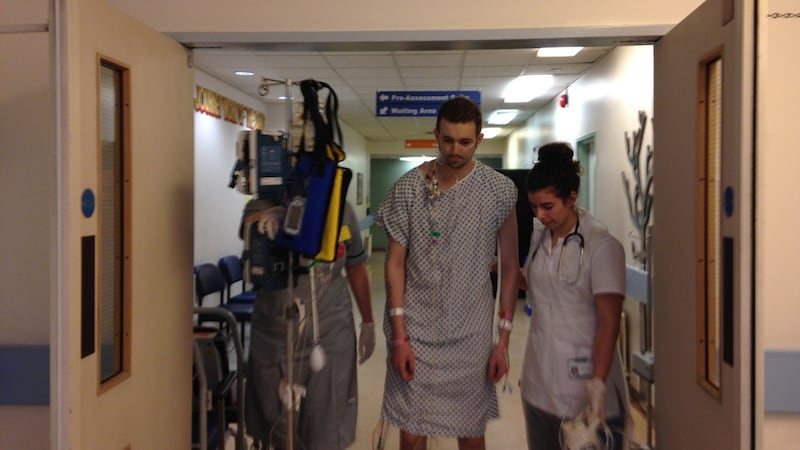
Surgery was the hardest and most painful experience of my life, far worse even than aggressive chemo. During the following week, it was important that I cough forcefully, to clear my lungs. It felt like a punishment. The pain from having to move my chest was intolerable and I winced whenever they asked me to do it. That week consisted of rarely leaving bed, except to sit up in a chair for 30 minutes a day. I had to inject myself with 1mg of morphine every five minutes on top of other medications and had fevers at night, which concerned me.
I had gone, in a matter of hours, from capable runner and swimmer to learning how to walk and move again. When the different nurses helped me to get up, they were always shocked to see how tall I was (6 feet 5in) because they had only seen me lying in bed. I could barely move my right arm or shoulder. For four days, I had several large tubes coming out of my back and side, draining into plastic buckets, so when I walked, nurses had to carry the buckets behind me. I had never felt more fatigued.
High dependency unit
A few hours after my surgery, Mr Jordan and Mr James visited me in the high dependency unit, where I had been taken from the recovery room. Mr Jordan was extremely pleased with the results. He said my right lung had been “very angry” and they had to remove a very small wedge of it that had become attached to the tumour. Mr James, who had put 32 staples in my chest, was happy with the way my long, horizontal scar looked. It was neat and thin. Ten years ago, another doctor on the team told us, “It would have looked like a shark bite.”
The surgery had been an unequivocal success from the surgeons’ point of view, but we were still waiting for reports from the lab on the bone, tissue and tumour that had been removed, which meant I couldn’t feel celebratory just yet.
I was told it could be two weeks before the reports came back but about a week later, on my penultimate day in hospital, a Macmillan specialist nurse came into my room with news.

The reports had come back, showing that the response to chemo was completely successful, showing “clear margins and complete necrosis of the tumour”. In other words, the tumour was dead and the margins were safe. The chemo and radiotherapy had killed it. It wasn’t just good news, it was the best possible result. It was incredible news.
“Put your feet up,” Mr Jordan said, and so my recovery began. But that, as they say, is another story.
People from all over the world have contributed £8,900 to my online fundraiser for Macmillan Cancer Support in the UK, which gave me fantastic help during my 11 months of treatment. Our goal is to reach £10,000 (E 11,332).
Macmillan offers services in cancer care ranging from walk-in counselling and financial advice to alternative therapies for patients and their families. Please give what you can as they helped me. See https://www.justgiving.com/100daysofcalories











