Mike is propped up on pillows in his bed in Our Lady's Hospice in Harold's Cross in Dublin, listening to news coverage of the UK election on his phone. "It looks like Boris Johnson will get in. It will be interesting to see what happens after he gets in," he says, and then his voice trails off.
Mike does not seem to be thinking about what might happen with Brexit. He’s not even thinking as far ahead as Christmas, he says.
“I don’t know if this is the way you want to go,” he says, after a moment. He is referring to the interview. He seems unsure if I want him to be honest about this part of life that few people are comfortable discussing: the subject of his own death. I do.
He starts at the beginning. He was diagnosed with cancer two years ago. “I just started losing weight without trying to. I went for a check-up, and they found cancer. Initially they thought they could cure it. Going into the operation, they said I had stage two cancer. And when I came out, they said it was stage four. It’s terminal. There’s absolutely nothing more they can do. They gave me six months to live. And that was a year and a half ago.”
Lately, the pain has been getting worse. “It’s been a long time. It’s been a while. It’s wearying.”
When somebody mentioned palliative care to him at first, “there was a panic. I thought now, this is the end, and this is just going to be a matter of weeks. But actually there’s actually a lot more to it than that.”
This is his second admission to the hospice, and despite his initial fears, the experience has been very positive. When his pain intensifies or a new symptom develops, he can get relief immediately. Other aspects of his wellbeing are looked after too, “from the psychology to religion”.
“Like, I believe in God, but they cater for everything. Some of the alternative therapies they have here have made it bearable. It’s trying to find the point . . . Well, there is a point in the afterlife.”
There’s no point in the suffering though, I say. “No. That’s why I’d like to go. I’m quite happy to go now to be honest.”
Does he feel frightened? “No. Sometimes you get a touch of panic. But I’m not frightened to go now.”
“Everything is done,” he says. “The plot is bought.”
After the terminal diagnosis, he went on holidays to Lake Como with his wife. He bought a present for each of his four children “and I said when it’s nearer the time, I’ll give them. I know now in the last few weeks, it’s got a lot worse. And so I gave them all presents. It was a way to say goodbye.”
Mike is 62. Though his body is very frail, he has bright, keen blue eyes, which look like they belong to a much younger man. His own mother lived to 85. “My brother asked me, do I not feel angry or bitter? No, I don’t. I feel that’s the way life is. I had a reasonably good life and I have no reason to be angry or to be bitter. I’ve been very fortunate with four kids, all working, all living in Dublin,” and four grandchildren.
He has said everything he needs to say to them. “I’m ready for it. If you’re going to go, you want to go nicely, you know.”
****

Dr Stephen Higgins is the palliative care consultant at Our Lady's Hospice, which is celebrating its 140th anniversary this year. The organisation relies on fundraising of over €5.5. million every year. Over a cup of tea in the airy coffee dock in the new palliative care unit, I ask if most of the patients he sees are as reconciled as Mike.
“I think sometimes people are just weary. Their physical illness has made them so tired that actually it’s time to go. And they’re ready to go. They’re not happy about it, they’re not welcoming it, but it’s time to go,” he says.
Tiredness is the most common symptom he sees in patients nearing the end of their lives and is among the most difficult to manage. “It’s a very different tiredness” to the kind I might feel, he explains. “It isn’t proportionate to exertion.”
He has been working in palliative medicine for 15 years, work he finds enormously rewarding.
“People come to us dying. We can’t change that. We can acknowledge that, that we acknowledge that it’s hard.” The joy is in the “simple things you can do for them”, to make their final weeks or days easier. “What we do is we take very simple, obvious things, and do them really well.”

His own father died here, he says. “He was my first connection to here.” When he came to Harold’s Cross, “they brought him in a great big teapot. He was a tea junkie, and suddenly there was as much tea as he wanted in that teapot instead of the little metal one that only filled a half cup. So it’s those simple things.”
During the day, I sit in one of the multi-disciplinary meetings led by Higgins, at which every aspect of the wellbeing of each patient is discussed. This includes their physical and mental health; whether or not they have family support; if the family and patient are all fully aware of the situation; if there are any family strains or concerns. A lot of time on the day I visit is spent discussing logistics to get patients home for Christmas.
As the population ages, Higgins tells me later, he is seeing more patients of very advanced years. But those extra years of life are not necessarily healthy ones.
“By and large, although our life expectancy is rising very steeply these days, that extra life is not healthy. We’re living unwell for longer. So the need for palliative care or supportive care of symptoms is going to go up. Quantity of life is very important. But quality of life sometimes trumps that.”
Are we reaching a time where we need to give people more autonomy over decisions about the end of life? “You mean euthanasia,” he says, with the directness that, I learn, is essential to the job. “It sounds like something that should be a daily issue, but it comes up very infrequently.”

He estimates that only around two per cent of patients ever ask about it. “Is it something that I’m personally thinking would maybe help people? I don’t think it is. But it’s complicated, because I think there are small number of people for whom euthanasia would be a good thing.”
But he adds: “I don’t know how you can legalise it to be right for that small number, without endangering the bigger numbers. Because we see lots and lots of people who feel they’re a burden. They’ll say, ‘it’s not fair on my son or my daughter, I’m a burden. They would feel better if I was gone’.” Those patients could feel pressured, he fears.
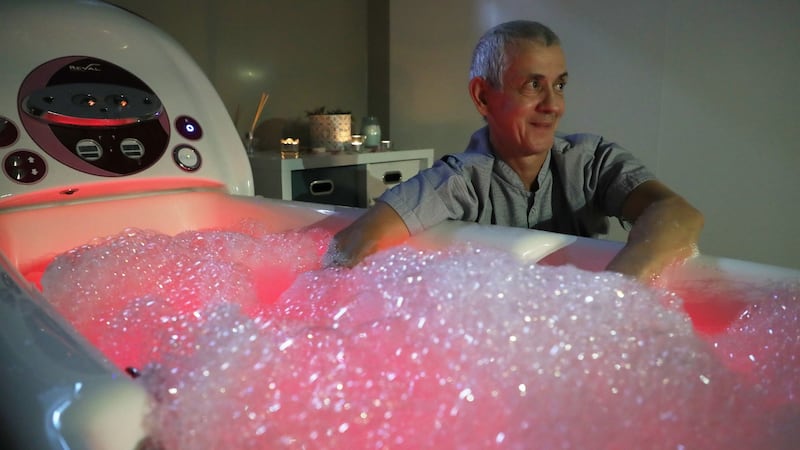
Here, the emphasis is on caring for the whole patient, not just treating the illness. There is a hair salon on site, a jacuzzi bath, beautiful landscaped courtyards, and classes in mindfulness; Tai Chi; relaxation; and other forms of exercise. As well as end-of-life care, there’s a day hospice, rehabilitative and respite care and a rheumatic and musculoskeletal disease unit, and Anna Gaynor house – the residential home for older people.
Over the course of the day, I meet a number of the 330 volunteers who work here. There are also more than 600 staff. One of the volunteers, Gay Davern, has never been stressed for a single day since he retired from the bank and started volunteering here as a driver. “I have never gotten up in the morning and said, ‘oh God, I’ve to go in there today’. And there’s many a day I had that in the bank. Once you come in the drive, and you see the ‘Slowly’ sign, the world just calms down. There’s a peace and serenity here, if you could only bottle it.”
*****
Caoilte Christie is a respite patient. He has been here for the past two weeks for pain management and “to be built up again”, after a host of health problems that started with a liver transplant he had in March 2013.
Until his admission here, he was in and out of other hospitals for about a year, before he collapsed at home in August and ended up in a coma. He is feeling much better now. His only complaint was that he wasn't well enough to get out of bed when singer Andrea Corr was here to switch on the Christmas lights.

He is very happy in his big, bright room, but anxious to get home to his Dad, who is in his 80s, and his older brother, Oran, who is in a wheelchair after a brain stem injury.
Christie, one of eight children, is full of stories. Oran “would buy and sell you and I,” he says. One time, after he got a new motorised wheelchair, which he was told could do 25km an hour, “My mother rang me at work going up the walls. She said, ‘it’s Oran, guess where he is? He’s on the M50’.”

*****
Anne D’arcy has what must be one of the most challenging jobs in the hospice. As senior medical social worker and bereavement co-ordinator, she runs the bereavement support service.
We meet in the room where support is provided to children aged between five and 18. For the very youngest children, the challenge is to make death concrete for them, she explains. “We would explain that when somebody dies, they’re no longer feeling anything, their body no longer feels hot or cold, they’re not hungry, they’re not thirsty, they’re not sad.”
Often, it has “to be done again and again and again, because the child can’t understand abstract concepts”, a process that can be heartbreaking for a bereaved parent, she says. “People are reluctant to use the words ‘death’ and ‘dead’, but for children it’s so important to do that.”

The experience of grief is often very physical for a child, and they can seem to bounce abruptly and without warning between devastation and normality. “They’ll have the tummy pains and the headaches, so it’s helping them to make those connections.”
Every year, the hospice holds a weekend for recently bereaved children. There is a worry box, and the biggest worry for children who have lost a parent is often that their other parent will die. When institutional abuse has been in the headlines, many worry that they will end up in an orphanage.
“We can tell them it’s very unlikely [that their surviving parent would die], and that they were very unlucky, but we can’t guarantee that it won’t happen,” says D’arcy, so the counselling will focus on getting them to think about the other people in their family and in their network who love them.
It’s important for parents to remember, she says, that “children adapt. They learn to live with it. They can still have a really good, positive life. But the thing with childhood loss is that at one level, it never goes away, because a child will re-grieve at different times” throughout their lives as the enormity of the loss becomes more real.

Higgins says that some of the hardest cases he sees, and the ones least likely to be at peace with the prospect of death, are the parents of young children. “I think it’s harder when you’re young, and it’s harder when you have dependent children, who might be eight or 10. That’s an age where they can understand. I think it depends on what you’re leaving behind. I think people are very brave. I’m consistently very impressed by people’s courage.”
*****
In his room at the end of the corridor, a bright space overlooking a courtyard, 35-year-old Aleksander Savostikovas – he goes by Alex – is watching YouTube videos about cars. "I just love this place. It's like a second home. And I really appreciate being here, having the chance to be in a place like this."
It’s not hospital, he says, and it’s not home, “but somewhere in the middle, which is great”.
He seems very grateful for everything. “It’s nice to have our garden, a bit of your own space and fresh air always. When you’re in the hospital, you have those locked windows and it’s only air con.”
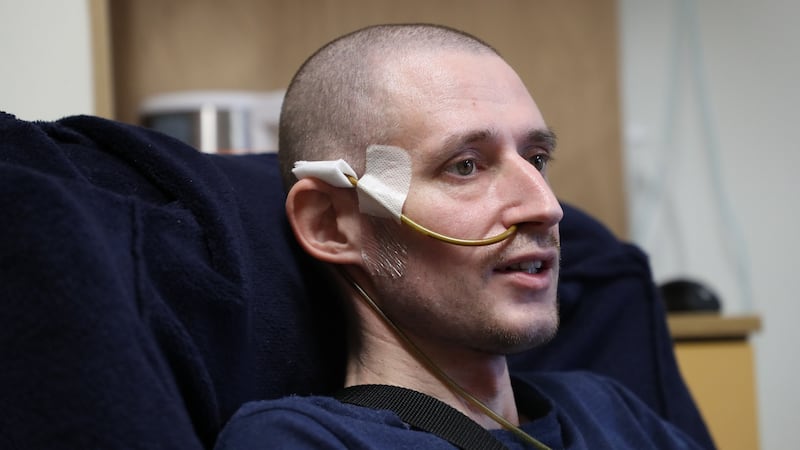
Why is he here? “Since the end of 2017, I’m fighting my cancer number four, which won’t let me go. It just won’t go. It is staying with me,” he says, in a low voice.
He had his first diagnosis shortly after he moved to Ireland from Lithuania at 20. "I was a mobile security supervisor. I was driving a van and pretending to be important. I loved that job. Oh, I really enjoyed that life. I had my wife, I was young, full of happiness, full of good energy . . . I could rule the world. I'm going to achieve things. This country is open for opportunities. But then when the sickness got me, everything just fall apart."
Between bouts of cancer, he had “five good years”, when he and his wife decided to try for a second baby. The baby, a son they called Denny, came “just in time”. Denny is six now, and his older boy, Dimitri, is 15.
“They understand that I’m sick. The bigger fella, he understands more. That it’s like a life issue. With the little fella, he’s always waiting for me, ‘Dad when are you coming?’”
In here, he says, “I just keep on thinking about my family. Family for me is very important, I want to be even a little part of their lives. I still want to be that little part. I want to see them grow and achieve something.”
How does he feel in himself now? “I’m hoping that I’m stable, and I’m okay. But the reality is a bit different. My cancer keeps growing and giving me more issues, little by little.
“That’s my life, which I did not choose, but it just happened to be.”
He wishes other people, who are well, appreciate their health. He spreads his arms wide as he says this. “If you have a lot of money you don’t have the health, what’s the point of the money? It can’t make you be a healthier person than you are.”
Later, he says, without self-pity: “I know my future is not long. Every moment now is a happy moment. I appreciate it.”
Some names have been changed at the request of patients. Find out about volunteering and fundraising for Our Lady's Hospice and Care Services in Harold's Cross and Blackrock at olh.ie











