There are similarities between Hurricane Ophelia and the likely imminent collapse of the Irish health system. Many of the trees that fell were already diseased or compromised in some way. Then came the unprecedented hurricane-strength winds, taking both these trees and some healthy ones with them.
Our public health service is already dangerously understaffed and doesn’t have enough beds in the system. Our population is ageing. And we are weeks away from the arrival of a healthcare Ophelia in the form of a severe influenza outbreak against which the current iteration of the flu vaccine is likely to be woefully ineffective.
Australia’s health system has just experienced a very challenging southern hemisphere winter. People were hit by two types of influenza: A (H3N2) and influenza B. More than 650 people in the state of Victoria have been admitted with the flu to hospitals – with almost one in 10 in such a severe condition they were placed in intensive care. Nationally, by the end of September, more than 137,500 cases of flu had been reported including a record-breaking 30,000 cases in August.That’s more than double the 53,159 cases confirmed by the same time last year.
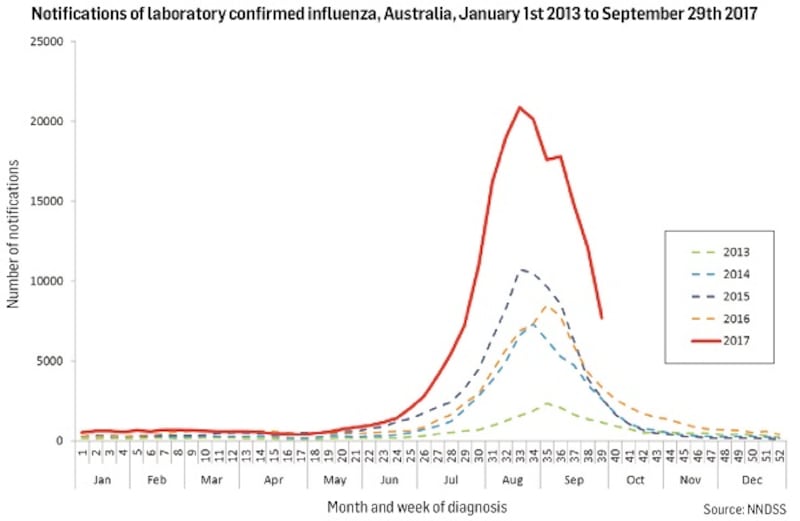
Ineffective vaccine
An ineffective vaccine seems to be the main reason for the severity of the flu epidemic “down under”. Infectious diseases expert Prof Peter Collignon of the Australian National University told ABC news that some 85 per cent of those who were vaccinated and then exposed to the influenza virus still got infected. This compares with an “average” year in which flu vaccine is about 40-50 per cent effective.
It appears the H3N2 component of this year’s southern hemisphere flu vaccine was relatively ineffective. The bad news for Ireland and Europe is that the vaccine being administered to people here contains exactly the same strain of H3N2 as the Australian population received. It’s too late to do anything about the mismatch; to allow for adequate production, our current flu vaccine – which contains three influenza strains – was chosen by the World Health Organization back in February. (Note: it is still worth getting a flu jab as it may reduce the severity of the illness for some.)
While not an absolute certainty, it is most likely a similar or slightly altered strain of H3N2 is already on its way, via air travellers from the antipodes, to Europe. It means we are in for a severe influenza season, with a huge consequent strain on the health service.
Ventilation
H3N2 is a particularly nasty infection in children under the age of 5 and in adults over 65. These age groups are the most likely to need hospitalisation. A significant percentage of these will require ventilation in intensive care units, as their hearts and lungs fail – some for a prolonged period. Which is where our struggling health service will finally run out of rope.
We have known we are short of intensive care unit (ICU) beds nationally for about 10 years. A 2015 report from the HSE estimates there were 237 critical care beds available nationally; some 67 were “not resourced”. Worryingly, there were less critical care beds in the system in 2015 compared with 2008.
A recommendation to expand ICU beds in the Department of Health/HSE prospectus report of 2009 must be implemented by increasing ICU bed numbers by at least 200 over the next five years, the president of the Irish Hospital Consultants Association, Dr Tom Ryan, told its annual meeting this month.
A slow collapse of the health system this winter will likely look like this: the influenza epidemic begins; attendances at emergency departments increase as the flu hits vulnerable groups; patients with flu complications who require admission will fill up trolleys; some people who develop respiratory and cardiac failure will be moved to intensive care; the already inadequate number of ICU beds will fill up quickly, forcing intensive care specialists to ventilate people in operating theatres and even in emergency departments. There will be no spare intensive care capacity in Northern Ireland or Britain to tap into.
Cancelled
As a result, even urgent cancer surgeries will be cancelled, as many patients who undergo major surgery cannot be safely operated on without an intensive care bed to transfer them to post-operatively. All elective surgery is likely to be cancelled for a period of eight to 10 weeks, adding to the already enormous backlog of people waiting to be treated in the public health system. Emergency departments will choke up and some will be forced to close. Already overstretched GPs will not have the capacity, and for seriously ill people, the facilities, to offer treatment.
There are many varieties of collapse. Some eventual collapses have a slow genesis. In the case of our health service, the writing has been on the wall for more than a decade, yet governments of different hues have failed to intervene appropriately. Instead, we continue with policies that actively disadvantage and alienate healthcare professionals from working in our health system. We have failed to expanded primary care services to compensate for the 1,400 acute hospital beds closed in the last 10 years.
It is too late to avoid a flu-induced failure of our health system this winter. As we saw with emergency personnel responding to Ophelia this week, doctors, nurses and others will rise to the occasion. But unlike our national emergency co-ordination group, who were clearly prepared, the health service is not. It will be a case of making it up as we go along. Unfortunately, that will mean avoidable deaths as the health system crosses a Rubicon of major failure.
Dr Muiris Houston is health analyst with The Irish Times.










