The extraordinary case of a clearly under-experienced doctor highlighted by Mr Justice Peter Kelly is far from an unusual occurrence in Irish hospitals.
Indeed, the judge pointed out that the case was not isolated and he has come across others where registered doctors “with little knowledge of the basics of medicine” were recruited to work for the HSE.
The Medical Council has also expressed concerns about the appointment of junior doctors with inadequate experience and qualifications to the HSE and medical recruitment companies.
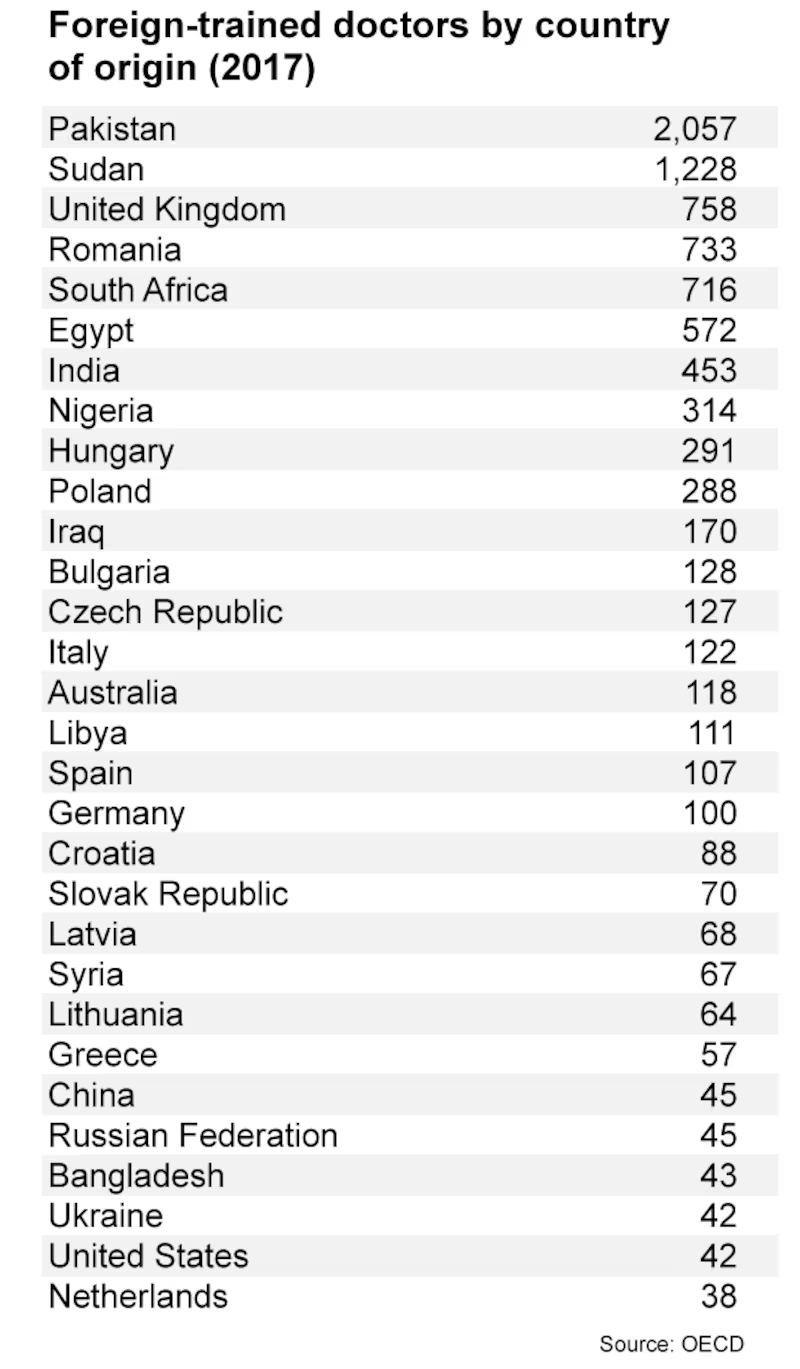

Privately, senior doctors are quick to express concern about the Irish health system’s ever increasing reliance on overseas doctors and the challenges of adjustment and integration this poses. The system’s equally heavy reliance on temporary, agency staff exacerbates the situation.
In recent years, there has been a steady stream of fitness to practise cases from the Medical Council featuring overseas doctors alleged to have made errors while working in Irish hospitals. Doctors from non-EU countries are over-represented in complaints made to the Medical Council.
In one case, it emerged the doctor before the inquiry had been hired following a single video-link interview between Ireland and an eastern European country. In other cases, questions were raised about the adequacy of checks on the qualifications of overseas applicants.
Language barrier
One area of difficulty that has arisen relates to some doctors who trained in an EU country, often in eastern Europe, but are themselves from a non-EU state. They may have trained in one non-mother tongue and are now practising in Ireland, using a second language, raising challenges.
In the most high-profile inquiry, a Sudanese doctor was found guilty on 28 counts of poor professional performance and six counts of professional misconduct after a Medical Council fitness to practise inquiry in 2016. The doctor, who mistook an ankle for an elbow in an X-ray, was taken off on-call duties because of concerns about his performance, but went on to be employed by three other public hospitals.
A subsequent report commissioned by the Government identified serious flaws with medical recruitment procedures, including a failure by one hospital to seek references. The report pointed to a lack of centralised recruitment processes for doctors in service posts and the absence of a single human resources system across HSE hospitals.
The HSE responded by saying it would establish a standardised policy to deal with references and Garda and medical registration checks prior to the appointment of junior doctors. An electronic personnel file for medical interns would also be rolled out, it was promised.
‘Blind eye’
One private sector recruiter told The Irish Times that hospitals seemed to prefer hiring short-term agency staff, despite the extra cost, to filling posts permanently. Some “turn a blind eye to English-language tests” and are stricter in vetting headhunted staff than direct hires, the source claimed.
The HSE uses a mix of central and localised recruitment, the latter organised through HR units in hospitals. Hospitals also recruit their own junior doctors.
Candidates are shortlisted if they meet standard eligibility criteria and are interviewed by a three-person board. Successful candidates are verified by screening their details, references and Garda vetting, the HSE says.
A doctor cannot practise in Ireland unless he or she is on the register, but the Medical Council says this does not mean the person is “suitable for every role”.
“It rests with employers to determine the suitability of a doctor to fulfil the requirements of a post, and to ensure that they are supported and appropriately supervised in their role,” according to a spokesman.
Minister for Health Simon Harris was also quick to point out that recruitment is the responsibility of the HSE. Mr Harris says he wants the HSE to "progress expeditiously" the review of its recruitment processes already under way.
Given the review has been under way since 2016, this seems like stating the obvious.









