When I found out on September 1st, 2014 that I was going to become a mother, I was overcome with joy and excitement. My husband and I were delighted and began discussing maternity options, car seats, baby carriers and cots. Like all expectant parents, we started preparing for our new arrival, adapting our lives in anticipation, imagining who our baby would be and what our lives would be like with them.
I could not wait to become a mother and yet it was through a barrage of tears that I packed my maternity bag; asking questions I never thought I would need to ask.
I packed all the usual items such as teddy bears, baby blankets, an outfit for our daughter. I also packed night dresses, maternity pads and a tens machine for labour.

However, among all these were items you wouldn’t typically expect to find in a maternity bag, such as our medical files, passports, accommodation information, hospital correspondence, directions and a memory book.
The day I had waited for with such excitement and anticipation had finally arrived, I was going to become a mother. But all I felt was grief, trauma, isolation and fear.
My daughter was dying inside me. She would never be born alive
My daughter was dying inside me. She would never be born alive. I could not save her and it was killing me. The one act of mothering that I could do as her parent was to ensure that she did not suffer, and this is how we ended up in the care of the foetal medicine team at Liverpool Women’s Hospital.
While my early pregnancy was like any normal pregnancy, at a 12-week scan a midwife raised concerns as to the wellbeing of our daughter. She arranged to carry out further blood tests and follow-up scans. At our next hospital appointment, we were given the heart-breaking news that our baby would not live.
Chromosomal condition
Our baby had stopped growing. They told my husband, Yousef, and me that she had a very rare chromosomal condition called triploidy. This meant she had a complete extra set of chromosomes; 69 compared with the usual 46. Not only was she extremely underdeveloped for her gestational age, but her lungs, chest and heart were comparatively smaller than the rest of her body.
This meant that her heart would never survive labour, she would never be able to breathe and she would never be born alive. It was predicted that I would likely have an imminent miscarriage.
Over the proceeding weeks, further diagnostic tests confirmed our daughter’s condition – backed up by foetal medicine experts across Ireland, the UK and Australia.
Our daughter had complete triploidy. The severity of the variant was fatal; no intervention could save her. Our daughter had what is medically classified as a fatal foetal abnormality (FFA).
The team of medical experts assigned to our care explained that if we wished to stay in the Irish hospital system and under its care, the only maternity option available to us was for me to remain pregnant and to wait for our daughter to pass away naturally. If we wanted to choose a different care path, we would have to leave our home, our families, our support network and our country.
I was overcome with grief and I could not accept that I was going to lose my baby. I wanted my daughter to be born at home under the team of foetal medicine experts at the maternity hospital that we were attending. I could not contemplate any other scenario, and I could not actively participate in her loss by seeking medical intervention to end my pregnancy.
I secretly hoped that they were all wrong, that even though she would not live, that she would survive labour, survive long enough for me to hold her, to kiss her and tell her that I loved her.
My mind was wishing for my pregnancy to end, as I grieved for the baby dying inside me
So, we waited. We waited 14 torturous weeks, 14 weeks where I could not participate in any aspect of normal life and finding myself in a most unnatural state of being. I was physically pregnant, and my body was telling me that I was having a baby. However, my mind was wishing for my pregnancy to end, as I grieved for the baby dying inside me.
Signs of demise
As the weeks progressed she began to collect fluid on her brain, her lungs and her colon. All of these were signs of her demise and the team charged with our care would no longer guarantee that she was not in distress in utero.
I learned that if her heart was still beating when I went into labour, that it would be the trauma of labour that would cause her to pass away. If she somehow survived labour, she would have a fit and pass away gasping for breath. Both of these experiences would be extremely distressing for her.
My physical and mental health was also suffering. My blood pressure had started to rise, and I had begun to show signs of early pre-eclampsia; a condition associated with triploid pregnancies that continue into the third trimester. The condition could develop very rapidly and, depending on its severity, could even be life threatening.
I was, however, told that unless my life was in imminent danger that they could not induce my labour.
I came to see abortion as a form of care for both my daughter and me
It was during this time that I came to see abortion as a form of care for both my daughter and me. As a mother, I felt that I had to take responsibility for my daughter’s wellbeing and ensure that she did not suffer. I also felt that in this instance I had to protect my health and my ability to have a family in the future. This is how we made the decision to travel to Liverpool Women’s Hospital.
To ensure that our daughter felt no pain during labour or birth, the medical team put her to sleep with a foeticidal injection into my umbilical cord before they induced my labour.
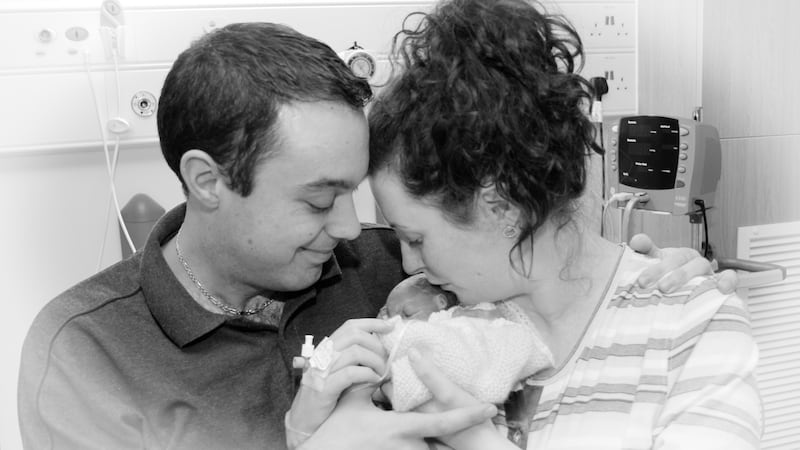
So, it came to be that in consenting to this procedure, I got to perform an act of mothering and, after a compassionate induction of labour in February 2015, our daughter, Rose Sophia Hazimee, was stillborn.
When we were travelling to Liverpool, I was hopeful that no other family facing a situation like us would have to travel abroad to receive the maternity care that they needed. Clare Daly had put forward a Bill to amend the Protection of Life During Pregnancy Act to allow for terminations of pregnancy in cases of FFA.
The day Rose was stillborn at Liverpool Women’s Hospital was the day that Clare Daly’s Bill was defeated by 104 to 20 votes. Our Government had been given the opportunity to care for families like mine and yet they would continue to turn their back on us in our time of greatest need.
Home alone
We had travelled by ferry to Liverpool as we had wanted to bring our daughter home with us. However, when she was born, she was very tiny and fragile, and the medical team advised us that she may not survive the journey home intact. It was put to us that it would be more respectful to her to leave her in the care of the midwife who had delivered her, and to have her cremated in Liverpool.
I was forced to leave Ireland pregnant and found myself returning without my baby
So, I found myself returning home without my baby to a country that no longer felt like my home.
Like so many women before me, I was forced to leave Ireland pregnant and found myself returning without my baby.
In the months that followed I attended support meetings run by a group of bereaved parents called Leanbh Mo Chroí. It supports women and couples who receive a diagnosis of a fatal foetal abnormality in pregnancy and are denied access to abortion services in Ireland.

By participating in these meetings and hearing the stories of others, I began to see the many ways in which Ireland’s abortion ban affects women, couples and families like mine. Heartbreaking situations are made more difficult, traumatic and dangerous because women are denied access to abortion healthcare in Ireland.
I decided to share my story publicly and join Termination for Medical Reasons Ireland, which is campaigning for a change to Ireland’s ban on abortion.
Citizens’ Assembly
I was eager to participate in the Citizens’ Assembly because I saw it as an opportunity to contribute valuable first-hand experience to Ireland’s abortion debate.
I submitted a personal account of my pregnancy with my daughter Rose through the online process on the Citizens’ Assembly website. I was then contacted by the secretary of the assembly and asked if I would give a personal testimony to the citizens.
The secretary stipulated that my testimony would have to be given anonymously and that it would take the form of a pre-recorded interview which would then be played on one of the assembly weekends.
I raised concerns regarding the anonymous aspect of the testimony as I felt it dehumanised the women and perpetuated the stigma of abortion, and I asked if I could present my testimony in person. I was, however, informed that my request would not be facilitated. Despite my reservations I decided to give my testimony and contribute to the discussion.
The Citizens’ Assembly was an opportunity for the discussion to be informed by fact, human experience and expertise. Presentations were made by medical, legal and human rights experts, both nationally and internationally. This was in conjunction with presentations from advocacy groups and women who have been directly affected by Ireland’s abortion ban.
The open submission process gave all citizens, regardless of their views, an opportunity to contribute to the discussion. The recommendations made by the Citizens’ Assembly indicate that the public understand that women need greater access to abortion in Ireland. I hope that the Irish Government will listen to its recommendations.
I welcome the report by Justice Mary Laffoy published this week, and I urge the joint Oireachtas Committee to use it as a framework for abortion reform. I specifically welcome the auxiliary recommendations outlined in the report for universal access to anomaly scans and prenatal testing for all pregnant women.
I have learned that when parents like myself are presented with all the medical evidence they may choose to have an abortion, as they see it as being the most humane care option for their baby in their specific set of medical circumstances.
From my experience, I don’t think any legislation can cover the full complexities of medical need that can arise in pregnancy. I believe abortion should be treated as a healthcare issue, so that women and families can make medical decisions based on their specific healthcare needs.
While I never imagined that I would need an abortion, I did. I was trapped in a pregnancy with no happy ending and we felt, in our circumstances, an abortion was the best care option for us.
I since have had a daughter called Alice Rose Hazimee (Rose, after her sister), who is 16 months old.








