I'm in a house in west Dublin, and my interviewee is puzzling me. Theresa Kinsella (82) doesn't seem to be following my questions. She asks me to repeat them, and sometimes wanders off in another direction.
“My memory is going, I’m sorry,” she says every now and then, frowning into space. When I ask her about dates concerning the care of her daughter Fiona (52), who has intellectual disabilities and has lived at home all her life, Theresa apologises and says she can’t remember.
The Kinsellas first sought a residential placement for Fiona in 2004. I know this, because a letter dated May 6th, 2004, is shown to me by another daughter, Gina, who is also in the room, along with Gina’s father, Michael (79). It is from the then clinical director of the Daughters of Charity at St Vincent’s Centre, in the Navan Road area of Dublin. It concludes: “It was agreed that Fiona’s name would be placed on our long-term residential waiting list for a community residential placement.” That was 13 years ago; Fiona is still on the waiting list.
Gina hands me a second letter. It is from Theresa’s doctor, on HSE-headed paper, addressed to the current clinical director of services at St Vincent’s Centre. Fiona attends the centre daily, Monday to Friday. The letter is dated January 10th, 2017. It is cc’d to Gina, and three other people, including Fiona’s social worker at St Vincent’s.
This is what it says: “The above lady [Theresa] is a patient of mine . . . She has had a significant deterioration in the past six months and now has well-established dementia . . . I am aware that she is a carer for her daughter Fiona who has intellectual disability. Certainly, given her very significant dementia and this recent deterioration, I would have serious safety concerns for the two of them should this situation continue.”
It is only then that I realise I am interviewing a woman who has been diagnosed with dementia. It is now Gina to whom all correspondence goes about her mother’s hospital appointments, and it is Gina who has power of attorney over her mother.
In April, the HSE stated that “Ms Fiona Kinsella continues to remain on the priority waiting list for residential care placement with the Daughters of Charity. The HSE have spoken this week to Mr Denis Cronin, chief executive of the Daughters of Charity, and he has confirmed that there are currently no residential vacancies within their service. If such a vacancy were to arise, there is no guarantee that Fiona would be offered this placement, as there are other clients that have been clinically assessed as having a higher medical priority for placement.”
I'm worn out. I don't begrudge what I do, but I am really tired
So, despite the fact that all relevant officials are aware of Theresa’s progressive dementia, the State sees fit to allow her to remain as Fiona’s primary carer. Not only that, the HSE has clearly flagged that should a residential placement become available, there are others with a “higher medical priority” for that place than Fiona.
“I’m worn out. I don’t begrudge what I do, but I am really tired,” Theresa says. “To be really truthful, I would prefer if Fiona went before me, because then I wouldn’t be leaving her behind when I die.”
“It is so hard for all of us, and so worrying,” Gina says.
The letter Theresa’s doctor sent to the Daughters of Charity also listed some of her recent behaviour. She has left the house without remembering to turn the cooker off. She gets lost walking home from the local shops. She has had to have strangers on the street intervene to use her phone to call Gina to come get her, because she has forgotten who she is and where she is going.
“Mum and Dad are no longer really able for Fiona. They have cared for her for 52 years and they can’t do it any more.”
Michael, who is also sitting with us, doesn’t say much. To my inexpert eye, he looks very physically frail. Last year, he was in a car crash in Limerick. “Dad has not been the same since,” Gina says. “His speech and mobility are not what they were. He is much more frail than he was.”
“Fiona is a good girl,” Michael says. For much of the time I spend with the Kinsellas, Michael looks as if he is in a kind of daze. I’m not sure how much of the conversation he’s following, as he is mostly unresponsive: it’s Gina who answers my questions for him.
At one point, he gets up with great difficulty from the couch, to show me a tile mosaic of a yellow flower Fiona made at the day centre she attends. “Fiona did that. She’s a good girl,” he says.

At 3.30pm, Fiona arrives home from the day centre. She bursts into the room, and immediately sits down beside Theresa; so close to her, she’s almost sitting in her lap. “Hello!” she says to me. Fiona can speak, and eat, and is mobile. When prompted, she is able to dress herself and shower, but if not reminded, won’t do either.
She can’t read or write, cook, drive, ride a bike, make a phonecall, cross the road safely, use public transport by herself, or safely go outside without supervision. She cannot remember her full address, although she has lived in this house for 52 years. Fiona will never be able to live an independent life.
When the family last had a meeting with the Daughters of Charity about Fiona’s care, Gina and her sister Ann asked straight out what would happen Fiona should either of their parents die.
“We were told she would be placed in a nursing home until a residential placement was found for her. But why can’t they find it now?”
* * * * *
In November last year, I went to rural Wexford to talk to Johanne and Alan Powell. They wanted to talk about the challenges they were facing as primary carers for their profoundly disabled daughter, Siobhan (32). They had been seeking residential care for her since 2013.
Siobhan cannot walk or speak, cannot eat solid food, and is doubly incontinent. She is the physical size of an eight-year-child. Johanne in particular spoke very frankly of her exhaustion for caring for Siobhan, and her infuriation at the general perception by the public that family carers are somehow saintly because of the work they do.
“What annoys me the most is when people come up to you and say, ‘God only gives these special children to people who can cope with them.’ Well, he can take her back then,” Johanne told me. “I’m doing this job because I have to, becasue there is no alternative. I don’t want to do it any more.” she said, “I want to be able to have a life while I have a life. I want residential care for my daughter. There is no such thing as retiring for carers unless you die.”

At that point, Siobhan was one of 61 people in Co Wexford awaiting a residential care placement. , I contacted the Powells again to see if anything had since changed for them. It has not.
The State is divided into nine Community Healthcare Organisations (CHOs). Wexford is in Area 5, which also includes South Tipperary, Carlow, Kilkenny and Waterford. Their area office is in Kilkenny. On March 28th, a HSE representative wrote to Brendan Howlin, who is the local TD for the Powells. They had asked him to advocate for a placement for Siobhan on their behalf. In the letter to Brendan Howlin, Johanne’s name is misspelled as “Johanna”. It stated:
“The provision of residential services in Wexford has come under further pressure in recent years . . . In November 2015, Siobhan had been assessed as Priority 1 (people who have been assessed as requiring this service [residential placement] in the short-term). Unfortunately, it is not possible at this time to specify when a residential placement can be provided.”
We are being completely ignored in the hope that our children will die before us
“So nothing has changed for us since last November,” says Johanne. “There are thousands of us carers: parents, sisters, brothers, uncles, aunts. We are being completely ignored in the hope that our children will die before us. Well, I for one do not want to see our daughter dead before us, I want to see her settled and happy and living a fulfilled life before we are gone.

"I don't blame the local HSE representatives, but I do most certainly blame the Department of Health, the Minister for Health and the Minister for Disability. They need to start consulting with us and help us look for solutions instead.
“I am so sick of being patted on the head and being told how wonderful I am for caring for Siobhan. It is patronising twaddle, and so is the lip service trotted out about looking after the most vulnerable in society. What is desperately needed is a proper plan for the future of services for disabled people and the proper funding to improve life for us.”
* * * * *
The November 2016 interview with the Powells provoked an enormous response from readers who wanted to share their own stories about caring for family members.
One couple who got in contact were Rem and Niki Collier, who live in Dublin. They were seeking additional respite nights for their daughter Coral, then nine. Coral was born with Trisomy 13, which means she has severe intellectual disabilities. In addition, she has epilepsy, and uses a wheelchair when she leaves the house.
Coral was waking every night between 3am and 4am, requiring one parent to then get up and stay up to supervise her. The Colliers took turns, and were both suffering sleep deprivation, and were fearful of neglecting their other child, Tanya (7), who is in good health.
The Colliers had been offered one night’s respite a month for Coral, starting in January. They had asked for three nights a week. So what has happened for them since?
“We have three nights respite a month now for Coral,” Rem says. “Two consecutive nights, and one other night. It has made a huge difference. We can plan to do some things now.
“Coral is sleeping now until 5am or 5.30am, and it has made a dramatic difference to our rest,” Niki says. She describes the LauraLynn centre, where Coral goes for respite, as “our sanity blanket. I cannot say enough about what they mean to our small family”.

Rem lectures in computer science in UCD. The Colliers wanted me to know that after the article appeared, his students took up a collection “for us to go towards getting some help or break”. They raised €2,350. “We used it to take Tanya to visit London for the first time, and for Rem’s birthday, to go to his family in the UK so that Tanya could meet her cousins for the first time.”
They are able to spend more time with Tanya, and do more activities with her on the days and nights Coral is in respite, although they are still hoping for additional respite nights a month in the future.
* * * * *
Mary McDonnell, who has since turned 80, remains the primary carer for her daughter Sinéad (53). She also wanted to tell her story. The McDonnells live in Douglas, Co Cork. Sinéad has severe cerebral palsy, is doubly incontinent, has curvature of the spine, and is fed via a feeding tube.
In the past, Mary had received 10 weeks a year residential respite for Sinéad, in blocks of five fortnights. but due to cutbacks, it had been reduced to less than three weeks. Mary and her husband Denis (79) were seeking a residential placement for Sinéad, as they felt they would be soon physically and mentally unable to continue to care for their daughter.
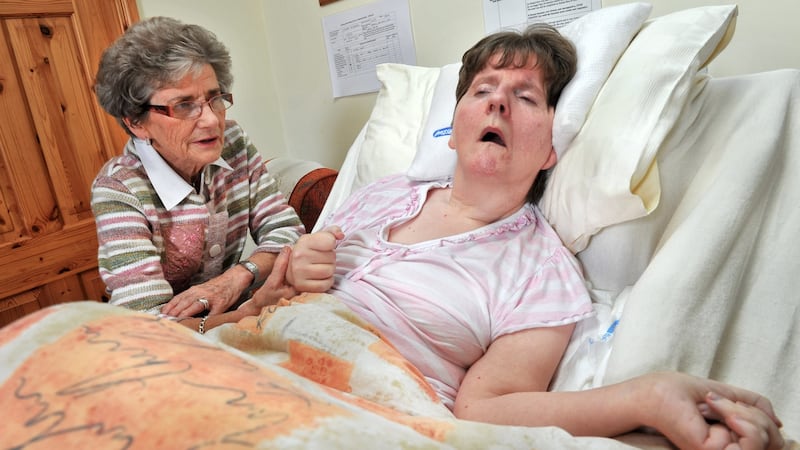
Mary is often unwell with respiratory problems due to asthma. When I called Her to see what the last few months had brought, she told me Sinéad had received three weeks of emergency respite earlier in the year, but only because Mary had herself been hospitalised. “I have breathing problems,” she said. She was in hospital for six nights, and when discharged, was very weak. Even talking to me on the phone, I can hear her struggle to catch her breath.
Sinéad is still awaiting a residential care placement. “The bottom line is that nothing has changed for us, or for the thousands of others like us,” Mary says.
* * * * *
Recently, I contacted the HSE with a Freedom of Information request. I was seeking information on the number of people with intellectual disabilities who were awaiting residential care placements, and the number of existing residential care placements in each county.
Although I had been given these figures in November by the HSE for Co Wexford, it now appeared getting similar country-wide information was going to be more difficult.
The reply to my request read: “The information you are seeking is not held centrally and falls under the remit of each CHO [the country is divided into nine Community Healthcare Organisations] area . . . You will need to make a separate FOI request to each of them for their local records.”
I did this. The responses from the nine CHO areas were not standardised. Some detailed the figures for each of the counties they represented; some only gave overall figures and did not break down the figures by county. In total, 1,375 people were waiting for a residential placement. The county with the highest number of people waiting was Galway, at 402.
The report found that 2,164 new full-time residential placements were going to be required
Some of the nine CHO areas informed me they do not currently operate a waiting list. One of these is Area 4, which covers Kerry, North Cork, North Lee, South Lee and West Cork. “The HSE in Cork and Kerry CHO provides residential services for people with intellectual disabilities in two centres; Cluain Fhionnáin, Killarney and St Raphael’s Services, Youghal. Both services are closed to admissions and there are no waiting lists for placements in these services.”
On June 21st, the Health Research Board published its Annual Report of the National Intellectual Disability Database Committee 2016 Main Findings. These findings refer to the 28,272 people countrywide registered with the National Intellectual Disability Database. Almost two-thirds of them are male, at 59 per cent, with 41 per cent female.
The report found that, based in these figures, there is a significant unmet need for services. To meet this need, the report found that 2,164 new full-time residential placements were going to be required: residential placements for people with intellectual disabilities such as Fiona Kinsella, Siobhan Powell and Sinéad McDonnell are all in such dire need of.
Earlier this month, the Central Statistics Office (CSO) released more summary results, taking the data from Census 2016. These summary results included information on carers. The CSO's full report on the module covering Health, Disability and Carers will be released in November of this year. However, it's already clear from the summary results that just over 4 per cent of the population, at 195,263 people, were providing unpaid care at the time data for Census 2016 was collected. That's an increase of 8,151 from Census 2011.
The data also showed that in addition to the growth in the number of carers in Ireland, the number of people spending more hours a day caring had also increased. For example, 41,185 people were providing care for more than six hours a day.
Those figures of 195,263 people include Theresa Kinsella in Dublin, Johanne and Alan Powell in Wexford, Remi and Niki Collier in Dublin, and Mary McDonnell in Cork. Theirs are just four stories of carers in crisis. How many of the remaining 195,259 people in this country who are carers are also in crisis?











