Bed sore scanner that can detect sores before they can be seen
Bed sores are one of the most common and most painful conditions affecting patients confined to bed in hospital. Generally associated with older people, they can also be a problem for people with spinal injuries, advanced-stage multiple sclerosis, and children and adults on surgical wards for extended periods.
"The problem is that we can't see any pressure points until they reach the skin," says Prof Zena Moore, head of the school of nursing at the Royal College of Surgeons of Ireland (RCSI). The current treatment for bed sores, otherwise known as pressure ulcers, is to turn the patient in bed every two to three hours. Specialised mattresses and cushions which better distribute the body mass are also used for some patients.

However, a new tool is currently being piloted in Naas General Hospital which offers hope for early detection and prevention of bed sores. This hand-held scanner can detect the sub-epidermal moisture in the skin which is an early sign of inflammation.
“Raised levels of sub-epidermal moisture (SEM) alerts us to bed sores that are developing inside the body at the muscle/bone interface,” says Gillian O’Brien, a nurse at Naas General Hospital, who has researched the SEM scanner as part of her Masters in advanced nursing practice.
In her study, O’Brien discovered that bed sores can be detected four days earlier using the device compared to patient-monitoring using skin inspection and other risk assessments. “We’d need one scanner for about 30 patients so that each patient could be scanned once a day,” says O’Brien. Naas General Hospital purchased a SEM scanner, following O’Brien’s study.
The RCSI is keen to highlight O’Brien’s study so that hospitals throughout Ireland can seek funding to buy these new scanners for use in wards. Based on NASA Mars lander technology, the scanners have been developed by the California medical device company, Bruin Biometrics. They are sold through Fannin Healthcare in Ireland.
“They are extremely expensive but prevention is cheaper than treatment in the long term – and this isn’t even including the reduction of pain and discomfort to the patient with early detection,” says Moore.
A new blood-glucose monitoring system could replace finger-prick testing among people with diabetes Type 1
A new blood-glucose monitoring system using skin sensors has been described as a “potential game-changer in diabetes management” by Prof Donal O’Shea, consultant endocrinologist at St Vincent’s University Hospital, Dublin.
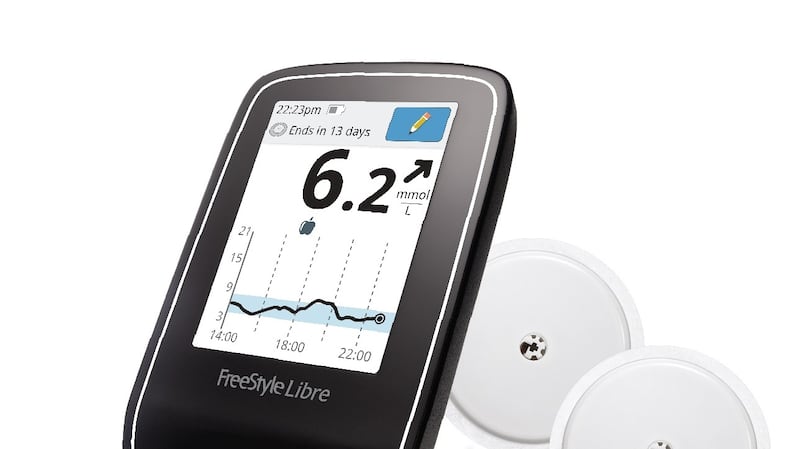
The system, which has just become available in Ireland, picks up blood-glucose levels via a sensor whose data is then transmitted via wireless technology to a hand-held reader. The sensor is embedded into a circular tab placed on the upper arm, allowing the person with diabetes to take readings as often as they like.
"A lot of parents of young adults with diabetes [Type 1] have already been purchasing the sensors through the UK so it's good to see it on the Irish market now," says Dr Anna Clarke, health promotion and research manager at Diabetes Ireland.
It is expected that people with diabetes who need to regularly monitor their blood-glucose levels will prefer the sensors to the current method of checking levels via a finger prick of blood and a blood-glucose meter. The sensor continues to monitor glucose levels throughout the night and this information is downloadable from the reader for use by the individual and their healthcare professional.
“Reaching a state of hypoglycaemia [low blood sugar] is the biggest concern for people with diabetes Type 1 and this system allows frequent readings of blood glucose so that the person can avoid this state by taking something to eat or drink,” explains Dr Clarke.
It is hoped that the longer term risks of hyperglycaemia (high blood sugar) can also avoided with more careful monitoring of blood glucose by those with diabetes Type 1.
Dublin footballer and PE/science teacher, Kevin Nolan spoke about his experience trying out the sensor when international healthcare company, Abbott, launched the product in Dublin in October. "I was diagnosed with diabetes in 2011 after I had lost two stone and was constantly thirsty," he explains.
Nolan says that he doesn’t hide his diabetes and often tests his blood-glucose levels in front of students in class.
“There are no real restrictions to having diabetes if you manage it well,” says Nolan, who checks his blood-glucose levels about five times a day and before, during and after football training sessions.
Professor O’Shea has also tested out the sensor technology in his diabetes clinic. “Ninty per cent of people prefer it and find it painless. There are lots of requests for it for children because parents can check levels with the reader at night time through a duvet. The diabetes teams will have more data than we’ve ever had so it will be important to use this data well,” says Prof O’Shea.
Called Freestyle Libre Flash Glucose Monitoring Systems, these new sensors are available only from the Abbott website. A starter pack with two sensors and a reader costs €169. Each sensor (which lasts for 14 days) costs €59.90. See freestylelibre.ie
O’Shea is keen to highlight the need for reimbursement for these sensors for people with diabetes Type 1 who can’t afford them. Currently, the HSE reimburses patients with diabetes Type I for their monthly supply of finger-prick tests.
Wearable tech
We know wearable technology is no longer science fiction as devices to monitor everything from blood pressure to sleep to daily steps have become commonplace.
However, research into how clothing can protect us from injury or indeed alert us to injury is still at the laboratory stage.
For instance, researchers at the University of Limerick are part of an international team of scientists and bioengineers developing a biometric exoskeleton. The aim of these soft "intelligent" trousers is to improve the mobility of older people or people with disabilities. The health robotics researchers are hoping that the soft lower limb exoskeleton would work as a movement prompt for the legs.
Dr Leonard O’Sullivan, head of UL’s School of Design says, “the current assistive devices for independent movement are fairly bulky and inflexible. They don’t encourage or support the activation of the legs, which is essential to prevent further atrophy.”
The so-called XoSoft project will use advanced textiles and smart materials with built-in sensors to communicate the user’s motion and intention so that the right level of support can be given.
Meanwhile, you can see a model of a prototype for wearable technology at the current exhibition, Design and Violence at the Science Gallery, Dublin (until January 22nd, 2017).
The exhibit, entitled Bruise, is an artistic representation of a pair of leggings fitted with pressure-sensitive film which can alert its wearer to injury. Intended for people who can't feel or communicate pain, the pressure-sensitive film changes colour when the body experiences a fracture, or soft tissue or joint damage. It was developed by researchers at the Royal College of Art and Imperial College London innovation graduates who were inspired by para-Olympian, Talan Skeels-Piggins.









