The new National Cancer Strategy will cost €100 million a year over the next 10 years, Minister for Health Simon Harris has said.
Speaking at Wednesday’s launch of the strategy, which covers 2017 to 2026, Mr Harris said he would seek the funding on an incremental basis as part of the budget estimates process.
He also said he was fully committed to all 52 recommendations in the strategy. His department will publish an annual report on the implementation of the recommendations, he said, and the degree to which the key performance indicators are met.
“We need to show year-on-year, the progress we are making in turning this strategy into a reality,” he said.
He described the launch as a “good day for the Irish health service” and said he was very determined to implement it.
The number of cancer cases in Ireland is expected to double by 2040, mainly due to an ageing population. Non-melanoma skin cancer is the most commonly diagnosed, followed by breast cancer in women, prostate cancer in men and colorectal and lung cancer in both.
Cancer prevention is described as the “cornerstone” of the strategy, which is the third iteration of a national cancer plan.
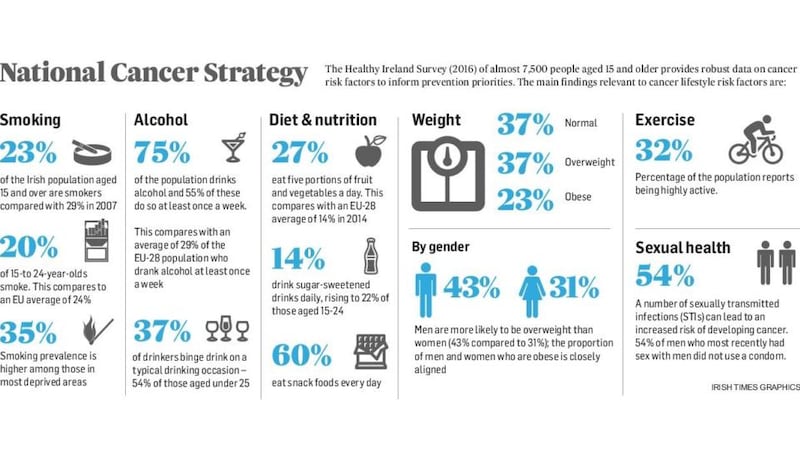
It aims to work toward a tobacco-free Ireland by 2025 and promote healthy lifestyles to address the 30 to 40 per cent of cancers that are preventable.
Speaking at the launch, chairman of the cancer strategy steering group Prof John Kennedy, said there had been enormous improvements in cancer treatment in Ireland in the past 20 years, but there were very substantial challenges to be faced.
Staffing problems
“For obvious reasons there has been limited investment in capital and human infrastructure over the past decade,” he said.
Allied health professionals, including radiographers, specialist nurses and specialists in genetic oncology are all “desperately needed”, he said.
He said Ireland must develop world class centres of excellence, and this will require significant investment and focus.
He also said the State is not producing enough staff in our institutions, and “desperately needed” foreign trained graduates or faced “inordinate and counter-productive delays in registration in Ireland”.
Prof Kennedy also said Ireland is “in danger of being left behind by the scientific revolution sweeping the world in cancer molecular diagnostics and treatment”.
This needed to be urgently addressed, he said, and significant investment was also required in cancer genetics.
Key recommendations
Key recommendations in the report include the extension of the screening programme for bowel cancer, from people aged 60 to 69 years, to those aged 55 to 74 by the end of 2021. Extension of the breast cancer screening programme will also continue, to take in all women aged 55 to 69 years by the end of 2021.
The strategy recommends centralisation of cancer surgery should continue, and 95 per cent of cancer surgery should be carried out at designated cancer centres by 2020.
Public sector radiation oncology facilities should be expanded in Dublin, Cork and Galway to meet patient demand and a national programme to refresh and replace equipment should be implemented.
Third level college places should be increased for the training of radiographers and sonographers. The report said the small numbers graduating in the field, 35–40 a year, was of “real concern”.
It recommends existing cancer genetic services be amalgamated into one national service and an appropriate site be identified. It also recommends the establishment of a steering group for cancer molecular diagnostics, tests which evaluate the status of tumour cells. The group will be chaired by a national lead, to be appointed.
The strategy also recommends “cancer survivorship programmes” be developed for patients with cancer and each cancer centre should establish a dedicated service “to address the psycho-social needs of patients with cancer and their families”.










