No parent has really earned their stripes until they have been through the ordeal of arriving at a hospital emergency department with a sick or injured child.
If they’re lucky, there will be lots of waiting around. Yes, lucky. A real emergency will be seen to very quickly.
But we parents don’t always see it that way. For us, being there with our child is, by definition, an emergency.
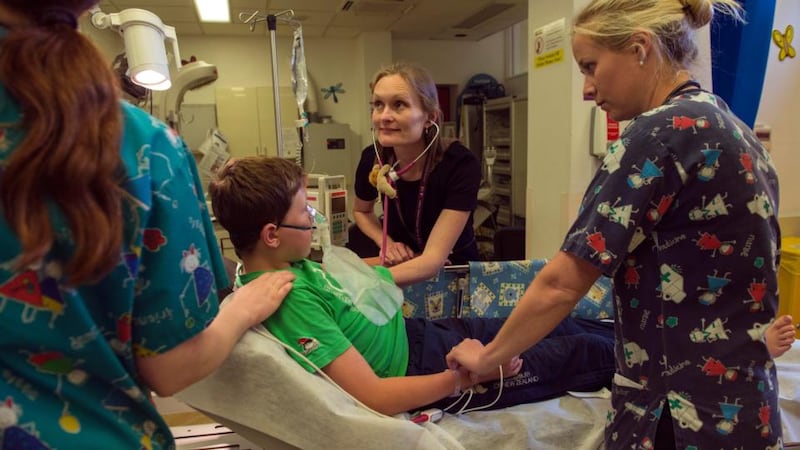
“Where am I in the queue?” is a question parents often ask and, while not unreasonable, it’s one the staff can’t really answer. It all depends on the severity of cases coming through the doors behind you, and there’s no way of predicting that.
There are more than 23 hospitals in the Republic in which acutely ill or injured children are seen, according to the HSE. Nearly all will admit cases if necessary, although some, such as Naas General Hospital in Co Kildare, will only see children and not admit them.
In Dublin, children are taken to one of the three specialist paediatric hospitals, while outside the capital, where hospital emergency departments (EDs) see both adults and children, about 20-25 per cent of attendances are children. Yet, “with few exceptions”, the 2012 “National Emergency Medicine Programme” noted, those hospitals “lack the necessary infrastructure, ie they lack adequate, child-friendly and appropriate audio-visually separated areas within EDs”.
Calm atmosphere
Passing through the ED of Our Lady’s Children’s Hospital, Crumlin, on a recent Friday afternoon, all seems calm. The resuscitation room with three beds, one designed for small babies, is empty and fewer than a dozen people are sitting in the waiting room.
Out in a treatment bay, one cheerful little boy with a blue bump on his forehead, who is being kept in for four hours of observation, is chatting while a nurse does one of the periodical checks to make sure there are no signs of deterioration.
There’s a seasonal nature to both the pace and the nature of work in the ED. While the number of children coming in reduces during the summer, it’s also the time when trauma injuries, both major and minor, are most common.
“As soon as the sun starts to shine, boys and girls fall out of trees,” says Dr Carol Blackburn, one of three ED consultants at Crumlin. “It is when kids get up on buildings and jump off roofs and things.”
Water-related incidents also spike, with drownings and near-drownings, coming in. Across the city, the ED of the Children’s University Hospital, Temple Street, has had two such headline incidents to deal with within 10 days.
It’s a reminder of the old cliche that emergency doctors never know what’s going to come through the door next, and illustrates why waiting times for less ill patients can be an issue.
“A big emergency coming into the department will slow everything down,” says Dr Róisín McNamara, ED consultant at Temple Street.
A drowning or a child in cardiac arrest will take up quite a few of the senior doctors, she points out, and, on occasions, she has had to go into the waiting room and explain that for the past hour and a half they have been working on a very sick child and that others will be seen as quickly as possible but, in the meantime, she requests parents to bear with them.
In her experience, there is never an issue with parents in those situations – or even generally, as their prime focus is the welfare of their child.
“It’s not like an adult hospital where you need a fairly serious security presence,” she says.
Keeping parents informed
Both she and Blackburn did their specialist paediatric emergency medicine training in the Royal Children’s Hospital in Melbourne, Australia, where the consultants emphasised the importance of keeping parents informed.
“I think that makes a difference,” says McNamara, who believes that, for the most part, what parents experience in Irish paediatric EDs is reasonable.
Knowing what to expect if you are making your first visit to an ED also helps. Sitting in Blackburn’s office in Crumlin, both she and McNamara outline how the system works – or, at least, is supposed to work.
Triage nurse
Within 15 minutes of registering at ED reception, some 95 per cent of children should be seen by a triage nurse.
Using the Irish Children’s Triage System, a nurse assigns the child a category ranging from one to five – one being the most acute – which will prioritise the order in which he or she is seen by a doctor (see panel).
A category one patient (less than 1 per cent of cases coming into the ED) will need a full medical team and will certainly be admitted. The majority of the category twos (about 15 per cent of cases) will also end up staying in.
Both agree that as ED consultants, category three children are the biggest challenge. “They tend to be the ones who have the potential to get very sick,” says Blackburn.
“We’re trying to decide what the problem is,” says McNamara. “It’s very easy when your arm is bent like this,” she says, miming a dangling limb. “But it’s the febrile child who has a bit of this, a bit of that . . .”
Although all three paediatric EDs in the capital – Crumlin, Temple Street and the National Children’s Hospital in Tallaght – strive to meet the 15-minute triage target, there is no formal assessment of whether or not they achieve it, says McNamara.
“In the future I am sure it will be tracked, but at the moment, it’s not.”
However, a “key performance indicator” is the six-hour target: in at least 95 per cent of cases, it should take no longer than six hours from the time a child arrives at the ED until that child is leaving the department, whether that is to go home, to a ward or the operating theatre.
“That is a target we monitor all the time,” says Blackburn. “In summer we exceed that target a good per cent of the time; in winter we do less well. But what we would say is that we consistently do better than any of the adult [emergency] departments.”
However, parents who find the process taking a lot longer than the six hours needn’t think they are entitled to their money back from the hospital, as some do.
The €100 charged to those who have no medical card and have not been referred by a GP is a State levy, which the hospital collects on behalf of the Government, Blackburn stresses.
Are staffing levels an issue? “Staffing levels everywhere are an issue,” says McNamara. And, for EDs in particular, it is extremely difficult to roster staff.
“One day, from 12 to 2pm, five patients can walk in the door and the next day, from 12pm to 2pm, 25 patients can walk in the door,” she says. It is consistently quieter between midnight and 8am, “but then if you come in between 12 and 8am, you are sick and if you are sick you need a complete team.”
Doctor shortage
Like all hospital departments, they are trying to work around a shortage of non-consultant doctors which, they say, is worse than in recent years.
“Doctors are leaving. We’re in flux now that we are trying to prepare for July,” says McNamara about the next six-month rotation of junior doctors that is due next Monday, July 14th.
Although being referred by a GP is a cheaper option for non-medical-card holders, only about one in five children coming into Crumlin and Temple Street EDs have gone this route, while the figure is more than one in three in Tallaght. For families in some areas, access to a GP can be a problem.
“We probably do see some children because parents can’t get into their GP through no fault of anybody’s – it is the way things are,” says Blackburn. And McNamara agrees that she has been told by parents that they were there because they couldn’t get a GP’s appointment soon enough and were really worried.
Do they think parents come into the ED unnecessarily? “We would take the view that if somebody is worried enough to come, they need something from us,” says Blackburn.
“We would never say to people: ‘You shouldn’t have come.’ ”
However, ringing an ED to outline your child’s symptoms isn’t helpful. It is very hard to give advice over the phone and it isn’t safe, she stresses.
“If your child is acutely unwell, you need to call an ambulance,” Blackburn adds.
“If your child is not acutely unwell but you are worried, it is probably best to call the GP first.”
swayman@irishtimes.com
What are the treatment options for minor injuries?
Minor injuries from outdoor activities are a summer hazard for children but sometimes bringing them into a hospital emergency department seems a little excessive.
However, if they need an X-ray or have a bad cut that needs stitching, there is little alternative within the public health system for the under-14s, although the age limit for treatment at minor injury units outside Dublin varies.
For example, in Monaghan Hospital it's age two and up; at the University Hospital, Ennis, Co Clare and Bantry General Hospital, Co Cork, it's age five and up; while in Louth County Hospital, Dundalk, it's age 14 and up.
In Dublin, when the new national children’s hospital eventually opens – currently scheduled for 2018 – on the St James’s Hospital campus, the capital’s three paediatric EDs will merge into one. But two satellite centres are planned for Tallaght and Blanchardstown, to treat minor paediatric illnesses and injuries.
Currently, for those willing and able to pay, the VHI operates SwiftCare clinics in Swords and Dundrum in Dublin and a third in Cork, that are open to all aged over 12 months and the family does not have to be VHI members to use them.
These clinics are very clear on what they do and don’t treat: for instance, fractures, cuts, burns and insect/animal bites are some of those on the “do” list, while the “don’ts” include loss of consciousness, severe burns, serious head/neck injuries and severe stomach pain.
“In the first six months of 2014, just under 30,000 children under the age of 16 presented for treatment at VHI SwiftCare Clinics,” says a VHI Healthcare spokesman.
“These children required attention for a complete mix of acute minor injuries and illnesses.”
He adds: "Patients are generally seen by a doctor within 10 minutes of the time they are first seen by the nurse."
That is what makes parents of children with minor injuries prepared to pay the heftier fees, although VHI members, depending on the nature of their insurance cover, may not have to pay any, or only part, of the doctor's €125 consultation fee.
The reduced consultation fee of €65 if referred by a GP is waived for VHI members. Fees for additional treatments include €95 per X-ray; €60 for stitching (free to members); and €60 for a full cast.
What to bring to the emergency department
Any medications that the child is currently taking
Child's correct personal details, such as forename and surname, date of birth, home address and telephone number, and also next-of-kin telephone number if different
Your medical card if you have one. Unless you have this, or a GP letter, or you are a member of the National Forces, there is a mandatory Government charge of €100
Your GP’s name
Bottled water is a good idea for child and waiting adults alike; a few snacks too
Some form of entertainment to pass the time with a child
Mobile phones should be switched off as they can affect some of the ED machinery (this request seems to be routinely ignored)









