Effective contraception will remain out of reach of the so-called “squeezed middle” if a new free birth control scheme is not rapidly extended to those aged over 25, GPs say.
Free contraception for those aged 17-25 is due to be introduced in the autumn as part of the Programme for Government. For the first time all young people will have access to the pill and other forms of contraception at no cost. Some who are older and accessing abortion services, however, will end up resuming the same contraception that failed them because they cannot afford more effective alternatives, doctors say.
The Department of Health has confirmed that for women and girls of eligible age, the scheme will be free with no consulting, dispensing or administration fees. The State will provide for the cost of prescription contraception; the cost of consultations with doctors to discuss and prescribe contraception to prevent pregnancy and treat other health issues; the cost of fitting and/or removal of various types of long-acting reversible contraception (LARCs) and related check-ups.
Included will be the cost of contraceptive options currently available to medical card holders including contraceptive injections, implants, various types of intrauterine systems (IUS) and devices (IUDs, or coils), the contraceptive patch and ring, and various oral contraceptive pills, including emergency contraception.
READ MORE
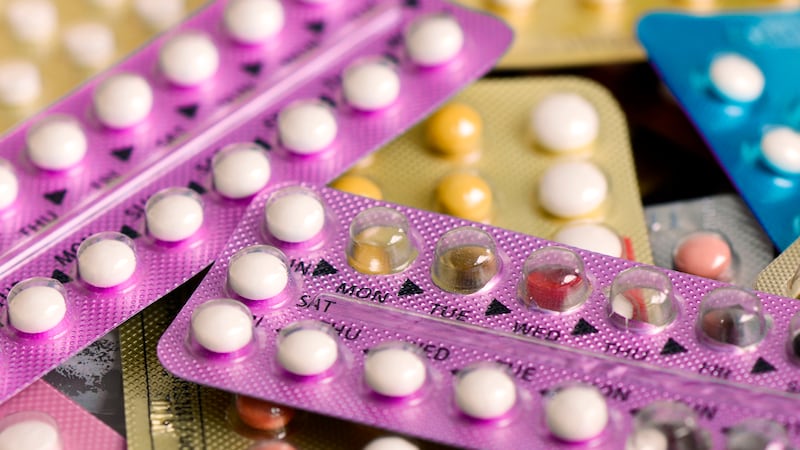
Condoms are already distributed free by the National Condom Distribution Service to HSE services and groups working with people described as at increased risk of “negative sexual health outcomes”, including young people, the department says.
Rollout of the new scheme, originally scheduled for last year, was delayed by the pandemic, the Government said. Subsequently promised for August this year, the Department of Health says it is now “currently scheduled for launch in Q3″. A wider rollout to women of all ages will be “gradually introduced”, Minister for Health Stephen Donnelly said last year. Free, or heavily subsidised, contraception for all ages has been the norm in the UK and other countries for decades.
The scheme has been welcomed by women’s groups and medics. However, they say reproductive health justice can only be fully delivered by removing the cost barrier across the whole reproductive age range. Cost is a greater barrier for younger women who are least likely to be financially independent, the Department of Health says. The cost of the most effective forms of contraception is, however, prohibitive for many women of all ages, experts say.
“We are seeing a group of women that have young kids already who can’t afford another child, but they also can’t afford a LARC, like the coil,” says Dr Áine Murphy who is a GP in Mayfield, Cork. “These are the people you would call the squeezed middle — they would have a mortgage and childcare costs and they can’t come up with the €400 or €500 for a LARC.”
Vasectomy, a surgical procedure providing permanent contraception, costs about €550. It is useful for couples who have completed their families, the HSE says. Though free to medical card holders, they may face waiting times and practice fees. Tubal ligation or female sterilisation permanently prevents pregnancy, says the HSE. It costs up to €1500 privately with waiting lists for the public system.
Meanwhile, Dr Murphy says she and medics in her network are now treating people who previously would have had to travel for abortion care or bought pills online, and they are seeing a clear link between unplanned pregnancies and the cost of contraception.
The Southern Taskforce on Abortion and Reproductive Topics (Start), a group comprising 250 medical professionals, did an audit of 475 people accessing its termination of pregnancy services in the first six months of 2019. Some 66 per cent of those accessing termination services were using no contraception; 20 per cent were using condoms and 10 per cent were using contraceptive pills. Only 1 per cent of women using long-acting, or what are sometimes called “fit and forget” contraception, had a contraceptive failure. Two-thirds of the women accessing the termination service were over 25.
“You never see LARCs being a failure — the coils and the implants — because they are 20 times more effective than everything else. You would be trying to encourage women to go for one of these afterwards.” The upfront cost, however, is prohibitive, Dr Murphy says.
“They’d be going back on the pill — ‘I’ll go back on the pill for now and I’ll get back to you later, I just need to get the money together’. They’ll make an appointment and then they will cancel the appointment. We are seeing quite a bit of that to be honest.”
Providing a free abortion service to women without free access to the most effective forms of contraception for all women is “putting the cart before the horse”, says Dr Murphy. Long-acting forms of contraception are more dependable than other popular forms of contraception such as the pill or condom, whose effectiveness depends on rigorously compliant use. Implants and coils are more than 99 per cent effective. With an extremely high rate of success, LARCs provide the best chance of reducing the incidence of unintended pregnancy.
“The reality is every week we send women away following an abortion with the same method of contraception that failed them in the first place because they cannot afford more effective contraception,” says Dr Murphy.

There is no question that people of all ages, those under 17 and over 25, need access to free contraception, says Dr Caitríona Henchion of the Irish Family Planning Association (IFPA). It is brilliant to see the scheme for younger people and the Government “has to start somewhere”, she says, but she is hopeful it will be quickly extended to all age groups.
Dr Henchion also says women with children whose contraception has failed are resuming the same form of contraception post-termination due to cost. “Because they can’t afford those upfront costs of getting the coil or an implant, they are just going back on the same pill they were on before to try and get the money together.
“We would love to just be able to give them whatever they want to be able to say, ‘Well that happened, but at least it’s not going to happen to me again’. It is just terrible not to be able to do that to someone who is actually saying, ‘I’m here, I never wanted to be here and I really don’t want to be back’ and you are not able to help them,” says Dr Henchion.
A six-month analysis by the IFPA of its early abortion service relating to 177 clients published in November 2020 showed many fell outside the age range of the new free contraception scheme. While 51 per cent of clients were in their 20s, 34 per cent were in their 30s and 7 per cent were over 40. Approximately half were mothers.
Some 68 per cent were not using a method of contraception when they became pregnant. Condoms at 20 per cent and short-acting methods such as the contraceptive pill at 8 per cent, were the most commonly used methods in the group.
Reform in contraception is lagging behind abortion care, the IFPA report noted, with cost still a barrier to some women’s access to the most effective methods of contraception. “Women experience unintended pregnancy for multiple and complex reasons. But lack of access to a choice of the most appropriate contraception should never be one of them,” said Dr Henchion.
Child spacing
Crisis pregnancies are not confined to women under 25, says the Irish College of General Practitioners (ICGP). The Government’s focus on tackling the issue among those aged under 25 must be widened, it says.
“It is really important for women who are in that age group where they may have had children already and are looking at child spacing,” says ICGP director of women’s health, Dr Noirín O’Herlihy.
“Child-spacing is just as important as other types of crisis pregnancies. Just because you are over 25 doesn’t mean it is not a crisis pregnancy for you.” Having the appropriate interval between births is recognised by the WHO as being important for maternal morbidity and mortality, she says. “I think the current Minister is very interested in women’s health. I think if free contraception care comes for everyone eventually, that will be huge,” says Dr O’Herlihy.
The health benefits of free reproductive care go beyond the young, says women’s health coordinator at the National Women’s’ Council (NWC), Alana Ryan. “There is good evidence that if you have pregnancies too close together, it increases the risk of maternal and infant complications, so having the control to be able to space your pregnancies, that does lower maternal health risks, not to mind all the socioeconomic benefits as well,” says Ryan.
The provision of contraception is widely recognised as a highly cost-effective public health intervention. This is because it reduces the number of unplanned pregnancies which bear high financial costs to individuals, the health service and to the state. This is according to research by Public Health England on the return on investment for publicly funded contraception there.
The Report of the Working Group on Access to Contraception, published in October 2019, identified barriers to accessing contraception for a significant amount of people in Ireland including accessibility, education, workforce capacity and cost. The group was established by former minister for health Simon Harris to consider the policy, regulatory and legislative issues relating to enhanced access to contraception, following the recommendation of the Joint Committee on the Eighth Amendment.
Some women are priced out of reproductive autonomy, says Ryan. “It comes back to a model of reproductive justice and enabling decision-making around our own bodies and ensuring that all services are accessible to all women.”
“The reality is that if you are a middle-class woman you have far more choices around contraception than if you are somebody who is struggling and living week to week. That is inherently unfair and not something in keeping with our values as a society,” says Ryan. It is also out of step with Sláintecare, which promises equal access to services for every citizen based on need and not their ability to pay, she says. “With the cost of living crisis at the moment, it is absolutely vital that we think about extending it.”
Extra staff
GPs say they have not received implementation details of the free contraception scheme for younger women, due to be rolled out in July. “We’ve heard nothing, absolutely nothing,” says Dr Áine Murphy. GP’s expectation is that all forms of contraception, including medical consultations and any related devices will be free, says Dr O’Herlihy of the ICGP. Many 17-25 year olds are holding off on fitting long-acting reversible contraceptives in the expectation that they will become free in later this year, she says.
Free contraception does not equate to it being accessible, however, says Dr Henchion. The scheme is likely to increase demand at a time when there is already a shortage of GPs, so there needs to be planning.
“There will have to be training and there will have to be extra staff to help with the extra workload. That’s the important thing, the planning of the implementation,” she says. The Department of Health says the cost of training and certifying additional medical professionals to fit and remove LARCs is included in funding.

Accessibility will be critical to the reform of contraception provision, says Ryan of the NWC. Pharmacist-prescribing for those 17 and older must be part of the conversation, she says. “It’s been done safely in other countries, and I think it would be quite transformative in terms of normalising access to contraception and also making it much easier for women in marginalised communities to access it,” she says.
Oral contraceptives could be delivered by appropriately trained pharmacists with risks mitigated by using medical screening tools, she says. “All this is part of the mix of ensuring we have a reproductive health model that works for women and girls.” In the US 17 states and the District of Columbia allow pharmacist-prescribed contraception, as do four provinces in Canada, she says. The regulatory framework in Ireland does not permit dispensing the pill without a prescription. It is not envisaged that this could be considered before the launch of the scheme, given the tight timelines, the department says.
More research would be useful in determining whether there is a reduced unintended pregnancy rate where the pill is available over the counter, says Dr Henchion. Going down this route may also mean women do not end up having the conversation about LARCs, though this can happen when women attend a GP for a last-minute pill prescription too, she says. Remote consultations with a GP or an appropriately trained practice nurse, normalised during the pandemic, could be a “game changer” for accessible contraceptive care, she says. “Not having to take time off or have to get your children minded every time you have to go and have a conversation would make it easier.”
Education
A public awareness campaign will also be critical to inform younger women about the free scheme, says Dr Henchion. “I would have loved to see a really, really good health promotion aspect to the rollout, not just about the methods, but the pros and cons such as, ‘this might make your painful periods go away’, or that there are long-acting reversible, no-hormone methods like the copper coil. That’s the kind of stuff people don’t know,” she says. Social media that tells girls that all hormones are bad needs to be countered. “People have this kind of, ‘I don’t want to take any hormones’, so they are relying on really unreliable methods and that’s definitely a health promotion issue.”
Discussions about the pros and cons of different contraceptive methods should be delivered in an age-appropriate way in schools, says Ryan of the NWC. All forms of free contraception will now be available to many in their final years of secondary school. “You shouldn’t just be relying on your peer network for this information, it should be part of the curriculum.”
Gender equality
The new scheme will free people up to have a healthy, happy sex life, without the dread of an unintended pregnancy hanging over them, says Dr Henchion.
It is also “a bit of rebalancing in terms of gender equality”, she says. While the cost of some forms of contraception like the pill is not that much, and some couples share the cost, contraception is nearly always paid for by women, she says. “It’s women and girls who have to find the money, or the girls’ mammies who have to find the money if they are worried about them. It’s not the boys’ mammies,” she says.
“Why should girls be bearing this cost, just because they will bear most of the brunt of the unplanned pregnancy if it happens? It’s a gender inequality issue,” says Dr Henchion. “You feel like in a lot of ways, if men had to pay for it, it would have been free absolutely ages ago.”













