Were you surprised to read about the first ever pig-to-human heart transplant that took place in the US earlier this month? I have to say I was – for a multiplicity of reasons.
One of the first feature articles I wrote for The Irish Times, published in February 2000, looked at how xenotransplantation (animal-to-human organ transfer) would be "the next step forward in the ever-changing world of transplant surgery, and has come about because of a global shortage of human organs".
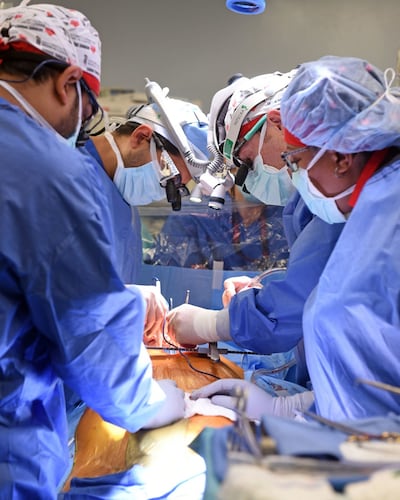
Almost 22 years later the first ever xenotransplant has finally taken place. On January 7th, David Bennett (57) was transplanted with a genetically modified heart from a pig at the University of Maryland Medical Centre. Suffering from end-stage heart failure, he was deemed unsuitable for a standard human-to-human transplant. Doctors had also decided he was a poor candidate for a ventricular assist device (an implantable artificial mechanical pump) because he had an irregular heart beat.
Some two weeks later Bennett is still alive, with his new heart beating soundly. So far, there are no reports of rejection of the pig’s heart by his immune system. Some of the 10 genetic changes made to the pig heart prior to transplantation seem to have subdued the usual sequence of rejection.
Why a pig and not a monkey or a baboon?
While it is true that pigs are less compatible with humans than monkeys, they can be genetically manipulated to produce organs less likely to be rejected on transplantation. Pigs quickly grow to full size, produce larger litters and can be more easily reared by biotechnology companies.
‘Better’ choice
You may also be surprised on ethical grounds. Animal rights activists may not be appeased by claims that pigs are already bred for human consumption and so represent a “better” choice than apes or monkeys. The significant genetic alterations necessary to prepare organs for transplant may be unacceptable to many. In Bennett’s case, the biotech company that made the pig heart used in the transplant cut out three pig genes that trigger attacks from the human immune system, and added six human genes that help the body to accept the organ. A final genetic modification aims to prevent the heart from growing post transplantation.
You may be taken aback to hear that Bennett’s surgery took place without a clinical trial of the procedure. The researchers had applied to the US Food and Drug Administration (FDA) to do a clinical trial of pig hearts in people, but were turned down. On the basis that he otherwise faced certain death, the researchers got a one-off permission from the FDA to give Bennett a pig heart.
Standard human-to-human heart transplantation is well established and highly successful: it has a one-year survival of about 90 per cent and a low one-year risk for rejection. Not knowing whether xenotransplantation has the potential to meet that standard in the absence of proper research puts a major question mark over the new procedure.
Around the corner
In favour of continuing to explore xenotransplants is the shortage of human donor organs. For example, about a third of donated hearts cannot be used in a transplant for a variety of reasons. And we must acknowledge the fact that heart valves from pigs have been used in humans for decades, and that insulins used prior to 1978 were derived from pigs and cattle.
But another issue that cannot be ignored when it comes to xenotransplants is that, for some of us, the thought of accepting an animal organ as a replacement for our own may even be repugnant. Would you have concerns for your personal identity if you received a pig’s heart?
So will xenotransplantation ever become routine? According to one veteran transplant surgeon I spoke to 22 years ago: “Xenotransplantation is just around the corner – and always will be.”
mhouston@irishtimes.com










