Psoriasis is a very common, non-contagious, long-term inflammatory skin disorder in which there is an increase in the rate at which skin cells are produced and shed from the skin. It affects at least 73,000 people in Ireland.
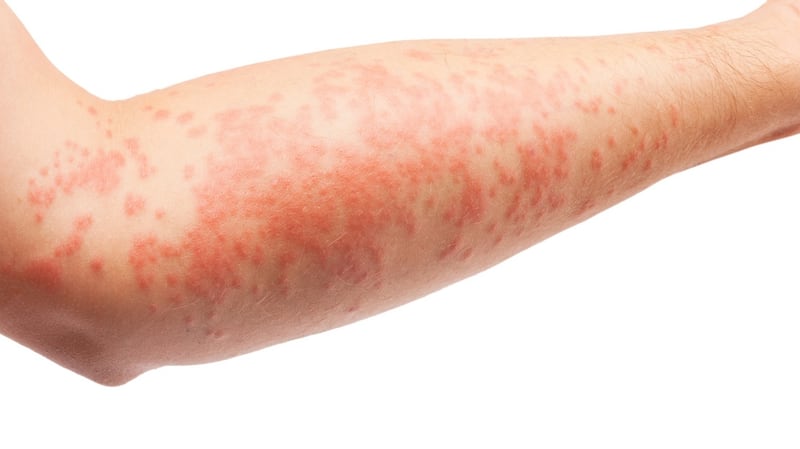
The red, raised scaly patches of psoriasis can affect any part of the skin surface, but most commonly involve the elbows, knees, lower back and scalp.
Psoriasis is a condition that tends to run in families – both the immune system and genetics are important in its development. Environmental factors can also play a role. In some cases, emotional stress, infection (such as a streptococcal throat infection), injury to the skin or certain medications can trigger the first episode of psoriasis, while certain lifestyle factors (such as heavy drinking and smoking) may worsen it.
Psoriasis is not contagious, infectious or the result of poor hygiene.
Some people with psoriasis notice seasonal changes in the severity of their condition, sometimes experiencing a worsening of symptoms in winter. Over the winter months, things like dry air from central heating and reduced exposure to sunlight can contribute to this deterioration. More generally, psoriasis tends to improve in warmer climates and worsen in colder ones.
Although there is no cure as yet, there are a range of effective treatment options available. Treating psoriasis is important for good disease management, as well as general health.
1) Emollient therapy: an important part of daily skin care
While the treatment of psoriasis depends on its severity and location, the use of emollients (commonly known as moisturisers), and emollient wash products (used instead of soap and shower gel), play an important, but often undervalued, role in management. Used every day, emollients help to soften the scale, soothe dry, itchy skin and increase the effectiveness of prescribed treatments.
2) Remember: avoid ordinary soap, shower gel and bubble bath
Winter conditions can be very drying on the skin, and soap-based products can further dry out the skin. Instead, choose soap substitutes/emollient wash products when bathing or showering.

3) Choosing an emollient
Emollients come as lotions, creams and ointments. Finding the right emollient is often a matter of trial and error – the best emollients are those that you prefer to use and will continue to use every day. Your healthcare professional will be able to give advice about the different emollient products available.
4) Applying emollients to the skin
Do not stick your fingers into a tub of emollient. Always use a clean spoon or spatula to prevent contamination. Emollients should be applied in a smooth, downward motion, in the direction of hair growth, after a bath/shower and before going to bed.
5) Treatment options for psoriasis
Talk with your doctor to find a treatment that is suitable for you. Try not to become disillusioned if one treatment does not work – there are many effective treatment options available: topical treatments (preparations applied directly to the skin), phototherapy (a form of artificial ultraviolet light therapy, delivered in hospital dermatology departments), and medicine taken in tablet form or by injection. Be sure to talk to your doctor about your symptoms and progress, and if necessary alternative treatment options or onward referral to a dermatologist.
6) Psoriasis affects people in different ways
Living with psoriasis can affect you emotionally and socially, as well as physically. Its unpredictable nature (psoriasis can vary in severity in the same person at different times) and visibility can negatively impact on a person’s quality of life and personal relationships. Everyday activities like trying on clothes when shopping, going to the swimming pool or even going to a hairdresser can be a challenge, sometimes leading to feelings of self-consciousness and embarrassment because of worries about what others will think or say.
7) Acknowledge your feelings and emotions about your condition
If you are feeling anxious or down, it is important to share your feelings with your doctor.
8) Associated conditions (co-morbidities)
Although psoriasis affects the skin, it is an inflammatory disorder, which means it is related to irregularities in the body’s own immune system, and has been associated with a number of other conditions, including cardiovascular disease and psoriatic arthritis. Ask your doctor about your risk for heart disease, diabetes, high cholesterol and high blood pressure. Your GP is an expert in screening and treating these if necessary. If you have symptoms of arthritis, ask for a referral to a rheumatologist.
9) If possible, identify and avoid psoriasis triggers
Things such as infections, injuries to your skin, stress, environmental conditions, smoking, alcohol and sunburn may make it worse.
10) Learn more about psoriasis
This will make it easier to have a conversation with your doctor about treatment options and treatment progress.
- Dr Anne-Marie Tobin is a consultant dermatologist at Tallaght Hospital, Dublin.
- The Irish Skin Foundation – a national charity which supports people with skin conditions – has relaunched its SaySomething campaign, which aims to empower people with psoriasis, and dispel the myths and stigma that can surround the condition. For more information or support, contact the Irish Skin Foundation at irishskin.ie or call 01 486 6280.










