"It's a bit of an enigma being a school nurse," says Valerie Pedlow about a job she has worked in for almost 30 years, currently at Wesley College in south Dublin.
She reckons even some people within schools don’t know the scope of their work, never mind the public at large. But now with schools on the frontline of “living with Covid”, nurses’ expertise is arguably more important than ever within the education community.
Their presence, in case of emergency, in helping to oversee management of chronic conditions such as asthma, diabetes, epilepsy and anaphylaxis, and to deal with a wide range of physical and mental issues, undoubtedly provides reassurance to pupils, parents and teachers alike. They’re known to have picked up on things in teenagers that no one else has seen.
We’re not talking here about public health nurses who make periodic visits to both primary and secondary schools as part of the school immunisation teams to deliver childhood vaccinations but rather “in-house” nurses attached predominantly, but not exclusively, to fee-paying schools with boarders. They are also found in a few non-fee-paying day schools, such as St Leo’s College in Carlow and Newpark Comprehensive school in Dublin, as well as in private day schools.
They're a small, select bunch of health professionals with a distinct role, making up a sub-group of about 35 active members in the Irish Nurses and Midwives Organisation (INMO). However, union membership is optional for nurses while every school nurse is required to be registered with the Nursing and Midwifery Board of Ireland. Another IMNO sub-group caters for nurses working in special education schools, where there are pupils with complex medical needs and some posts are funded by the Health Service Executive (HSE).
They do treat us just like they do their own mothers – down to the simplest things like 'a button has come off my shirt'
In Finland, school nurses are the norm and regarded as an important part of children's and adolescents' health services, offering easy access for adolescents in their everyday environment. Britain also has a strong tradition of school nurses but the Royal College of Nursing last year blamed public health budget cuts for a 30 per cent fall in numbers since 2010, leaving an estimated 2,100 working among the 32,000-plus schools in the UK.
The director of the National Association of Principals and Deputy Principals at second level here, Clive Byrne, has visited a typical Finnish school in Espoo. It not only had a full-time nurse but also access to a psychologist, speech and language and occupational therapy on particular days, which made it easier for students to be referred. He says the dilemma here is that there are too many schools.
“The access to a nurse would be wonderful in a school setting but, given the shortage of nurses in frontline medical services at the moment, it’s probably unrealistic to expect it to happen in the short term but it is something we should aim for,” he adds.
A spokesman for the Department of Education says the provision of nursing support in schools is a matter for the HSE, but he also acknowledges the work of an inter-departmental group on the integration of educational and health supports for children with special educational and additional care needs.
Patching up a student who has cut their hand during a home economics class, dealing with a concussion on the rugby field, talking through a pupil’s panic attack and addressing a bout of homesickness can be all part of a mainstream school nurse’s day, which is as varied and unpredictable as the teenagers they care for.
Isolation room
Since September, they have to be on standby for any student showing symptoms of Covid-19, who needs to be brought to the mandatory isolation room and a parent contacted to take them home, before that room is sanitised in preparation for the next possible case. Some have been trained in swabbing for Covid tests, so they can attend to international boarders on site if the need were to arise.
"You never know what's going to come in the door next – we deal with whatever comes during the day, as it happens," says Beverley Callender, who has been a nurse at Villiers School, a co-educational, boarding and day secondary school in Limerick, for the past 14 years. "Every day can be very different because you never know what you can be faced with, from an emergency point of view, or the regular coughs and colds and sports injuries."
She and other nurses note that children are much less likely to be sent into school sick, as most parents are complying with the guidance to keep them at home if they’re showing any symptoms.
With 600 pupils, of whom about 150 are boarders, Callender or her nursing colleague is available in the surgery from 8.30am to 7.30pm, Monday to Friday, and one of them is on call every second weekend when the boarders are there. They continued to provide cover during the recent half-term break when international students were unable to fly home and some chose to stay in school, rather than live out with a guardian for the week.
You have to make sure your eyes are smiley and kind, particularly if they're coming in and upset about something
Homesickness can be a huge problem for some students, says Callender, and school nurses tend to become a mother figure, not just for boarders but the whole school community. “They do treat us just like they do their own mothers – down to the simplest things like ‘a button has come off my shirt’”. A small issue, such as losing an item they need for a lesson, can become a big thing in a young student’s mind.
She finds that being a mother herself, with now two adult children, is invaluable experience when working with teenagers, but so too is her background in psychiatric nursing. Mental health issues have become a much larger part of all school nurses’ work in recent years and they make referrals to outside professionals.
“There is definitely a heightened amount of anxiety among young people nowadays – apart from the usual anxiety coming up to exam time,” says Callender. She doesn’t believe the upcoming generation is “brittle” but rather that teenagers are expected to cope with far more nowadays before they have the maturity to do so.
“Obviously some of that is because they are exposed to a huge amount due to the internet. We didn’t have to deal with the overt sexuality that is out there for them now; we didn’t have to deal with the dark web.”
Even in school there is more pressure around exams, grades and CAO points. School nurses are also seeing the fall-out from relationship issues at home and challenges that may come with being in a blended family. The holistic wellbeing of students is always the priority.
“Sometimes they will come in with an ache or a pain but there might be something else on their mind and they’ll tell you. You can help then – even if it just somebody in the dorm is annoying them,” says Callender.
Teenagers need the guidance of adults but with everybody busier, including parents, such support may be less available than in the past, she suggests.
Anxiety and Covid-19
In addition, since the schools reopened in September, she has observed “anxiety about Covid, anxiety about whether they will be able to do their State exams, anxiety about where it is all going to end”. Some are even worrying that if a vaccine does become available, will they have to have it because they’re afraid of injections.
Life is different for all pupils because they’re socially distanced in the classroom and must remain in their pods during break times, so they can’t mingle in the yard. However, Callender has noticed that pupils seem to be getting to know those in their pod very well and developing close ties.
“They’re spending more time in each other’s company than they would have if they were moving regularly. It’s good from that point of view for them.”
This term has probably been hardest for first-year pupils in secondary schools throughout the country because they didn’t end primary school in the ordinary way and most missed out on introductory days at their new schools. But at least, as Callender points out, schools have provided some consistency for children this autumn as different restrictions have been lifted and then reimposed in the wider community.
In some ways, “living with Covid” has not made that much difference to the nurses’ work because they were always very conscious of sanitising and the importance of infection control. But she is conscious of the impact mask-wearing and the screen her desk has on communication.
“You have to make sure your eyes are smiley and kind, particularly if they’re coming in and upset about something. Obviously, you can’t hug kids any more anyway, but before you could put your hand on their hand; now you can’t even do that.
“You feel sometimes you’re not being as caring even though you are trying to be more caring,” Callender adds.
Nursing cover
At Wesley, a co-ed school with more than 900 children, including about 100 boarders and also day boarders, nursing cover is provided from 8am until 10pm, Monday to Friday, and also over weekends by Valerie Pedlow and colleagues.
What she enjoys is “never knowing what each day is going to bring. We have an open-door policy and they can come in with any need at all.”
They get to know the children well, particularly the boarders, as they progress through the school. She too acknowledges there is more pressure on today’s teenagers and that school nurses are seeing the results of that coming in their door.
“From a mental health perspective, certainly. I think social media has a lot to answer for in that respect.” Being on the spot, nurses are dealing with anxiety episodes and panic attacks and all the difficulties that go with them.
However, as regards the new Covid-19 protocols, she believes teenagers “are incredibly good at adapting to situations and then it becomes the norm”. Even those inclined to anxiety are coping really well, she reports.
A typical day for the Wesley nurse starts at 8am, with seeing boarders who, like day pupils, may have conditions that need medication, monitoring and minding. From 8.30am, day children can come in, if they have fallen off their bikes on the way to school, for example.
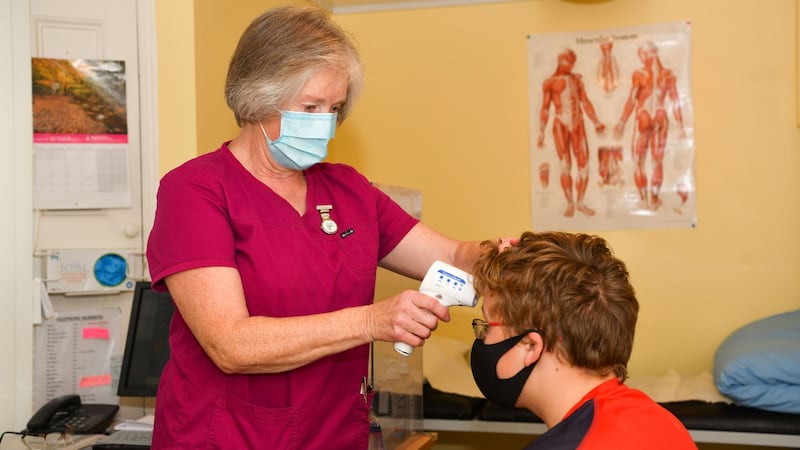
For routine issues they are supposed to go to the nurse during a break but they can come out of class if necessary. “If they become unwell or have an accident; if they need somewhere safe to be seen, to talk or to be cared for.”
PE is going on all day when “things happen”, says Pedlow and after 4pm there is sport until about 6pm. “We wait and see what walks in the door then.”
In normal times, “rugby does keep us busy” but not so much now when there’s no contact due to Covid-19. But generally, between it, hockey and basketball, there are “head injuries, knocks and bruises and dislocations – the usual sort of sporting injuries”, for the nurse on duty to attend to.
“We are lucky being in a Dublin school, we do have access to a variety of healthcare options; there are so many A&E’s they can go to,” she says.
The day pupils are gone by 6pm and after dinner both day and full-time boarders go to night study from 6.45pm. There is a nurse there until 10pm to make sure the boarders are okay for the night and that nurse will then be on call overnight. “Usually the call, if we get it, will be before midnight. We don’t get called often.”
While everybody is naturally highly alert to symptoms of Covid-19, it is important, Pedlow says, “to be aware of what else might be happening. If they come with a cough and feeling all hot, the GP will probably refer them for a test. But maybe something else is going on – just because it’s not Covid doesn’t mean there isn’t something important going on”.
It’s like when a child gets injured on the pitch, “if you think this is a definite head injury, you also have to be very mindful of how they hurt their neck and not to overlook anything else”.
While the pandemic has changed how schools operate, “at the end of the day,” she adds, “we are looking after children who don’t feel well. We just have to maintain our infection control and do what we do”.
Special schools
There are high-level needs among pupils in the country’s 125 special schools that can only be met by a nurse, according to a 2018 report of a cross-sectoral working group, which recommended ring-fenced HSE funding for such nursing support.
The nine health areas provide funds where possible, either directly or indirectly through voluntary bodies, while some boards of management directly employ their own.
The chairwoman of the special schools' sector with the INMO, Michelle Kennedy, says those nurses care for children with complex medical needs and physical disabilities, often as part of a multidisciplinary team. Although some work in isolation.
“The clinical challenges we are presented with would be vastly different to a school nurse in a mainstream setting,” Kennedy says.
As a union, they are looking for a standardisation of funding, processes and practices for nurses working in special schools, as currently it is very “ad hoc”. In this time of Covid-19, if staff are out sick it is very difficult to find relief staff at short notice, she says.
During the first lockdown, when parents had no respite, these nurses tried to support families as best they could even though services were closed. It was “a very difficult and traumatic time” for families.
Parents are stressed but, she adds, they really appreciate now the access to schools, which children with life-limiting conditions, for example, couldn’t attend without a nursing department.
The National Association of Boards of Management of Special Education reported in 2017 that a survey of 120 special schools showed 79 full-time and nine part-time nurses were employed in 40 of them.
A HSE survey that same year identified approximately 44.5 whole time equivalent posts it was funding in schools, along with an unspecified number of nurse educators and grant aid to fund additional nursing hours. The HSE was unable to provide any update in time for this article.












