Dread, commitment to the work, team spirit, fatigue, professionalism, frustration that we are here again, delight that a vaccine is beginning to be administered; dread. These are just some of the emotions observed during a day speaking to staff at St Vincent’s Hospital in Ballsbridge, Dublin, as they deal with the Covid-19 surge that is now under way.
"I had a few sleepless nights last year worrying about being faced with that scenario," says Dr Andrew Westbrook, intensive care consultant, referring to what happened in Bergamo, Italy, last year, when the hospital system there was overwhelmed by the number of coronavirus patients in need of care.
And now? “I’ve had one or two sleepless nights more recently.”
The hospital has 18 commissioned beds in its intensive care unit (ICU), a further seven in the post-anaesthesia unit beside the ICU, and has organised an ICU overflow ward, with up to 24 additional beds.
Does Westbrook expect the overflow ward to be used? “Of course we do. Based on the numbers.”

During the first coronavirus wave in March/April 2020, the hospital had 16 ICU beds, all but one of which was taken up with Covid-19 patients at one stage.
In that first wave, there were 36 individual ICU admissions of patients with Covid. One out of every five Covid-19 patients in the hospital, or 20 per cent, ended up in ICU.
As of Thursday, there were 66 patients in St Vincent’s with Covid, of whom four were in ICU. And hospital admissions are expected to grow sharply.
“We can probably get to mid-to-high 40s in this hospital” in terms of number of Covid-19 patients in ICU, “but beyond that, we would be running out of bodies and equipment.”
The ability to accommodate those in need of intensive care matters because it has a direct impact on mortality rates.
Mortality in the first wave was “in and around” 25 per cent of all ICU patients suffering from Covid. “Across the water [the UK] it could be double that.”
The key determinant in the differing mortality rates is the ability of ICU to cope with demand.
Learning from first wave
The hospital has the benefit of the experience gained during the first wave. But this time round the dynamics of the surge are different, says infectious diseases consultant Prof Paddy Mallon.
Speaking on Wednesday, he says he expects the number of Covid-19 patients in the hospital by this weekend to reach the peak seen when the first wave of the disease hit last year.
The March 2020 lockdown was introduced before we started seeing the hospitalisation of people suffering from Covid-19. This time around, the lockdown is only really coming into effect, and the hospitals are already dealing with a surge in cases.

“It is going to take a while for [this] lockdown to have an effect. So the whole dynamic is completely different... The numbers are likely to be much larger. The impact on the health service is likely to be much larger. And that is the big concern.”
He is by a window on the ground floor, to one side of the open reception lobby where people are sitting on chairs waiting to be seen at various clinics. It looks like a clean, bright hospital that is cruising along, below capacity, at ease. But that’s not the case at all.
“We are only at the start of wave three, unfortunately. We are nowhere near our peak, and I think we are some weeks away from where this is going to peak.”
Are we halfway to peak? “No. This is only started. The numbers have really only started to rise dramatically in the last four or five days, so this escalation is likely to go on for at least another 10 to 14 days if not longer. That’s how serious this is.”

As well as having to deal with the rising number of Covid-19 patients, the hospital is also having to deal with staff getting sick, or having to stay away from work because they need to self-isolate. This affects the hospital’s ability to deliver non-Covid services, in-patient and out-patient. In this way, the coming surge directly affects the health of a significant proportion of the population.
“People are exhausted. There is an element of frustration that we are here again. But staff are highly trained and know what they need to do. They are not going to stop working because this is happening, so we will all pull together and we will get through it.
“But you are looking at a different dynamic in terms of staff energy, staff enthusiasm, as compared with the first wave. I think that is an important point for the community to remember. Community actions, continued contacts, have an impact on the whole health system and on society, including the morale of the health services.”
Increased chance of survival
More is known now about the disease than was the case during the first wave, and there are treatments now that increase a patient’s chance of survival, he says. If you are over 60 years old and in hospital with Covid, progression to severe illness and death can be reduced by 10 per cent by these new treatments. “It is an important reduction but not a huge reduction.”
During Wednesday’s visit, The Irish Times speaks with consultants, nurses, scientists in the hospital’s laboratory, technicians, a porter, the head of security, people from the pharmacy division, a healthcare assistant and a medical laboratory assistant.

Everyone is dealing with risk. Patients who arrive at the emergency department (ED) with advanced Covid-19 illness "are very risky patients to deal with, as they have high viral loads, and may be coughing, and you are in and around their airways, treating their breathing difficulties," says Prof John Ryan, consultant in emergency medicine and the head of ED.
Prof Mallon, as an infectious diseases specialist, has always had to deal with threats to his personal welfare, because of the nature of his work, but makes the point that this is not generally true for hospital workers.
“I trained for this. I know what it is like to work with infectious diseases. The majority of people who entered healthcare did not do so to put themselves at risk of getting seriously sick, or dying, from an infection they would pick up in the course of their duties.”
A member of the hospital staff died over the Christmas period from Covid. “That had a significant impact across the hospital base.”
Safety is a constant in people’s minds, says Dr Michael O’Dwyer, consultant in anaesthesia and intensive care and head of the ICU, where to date not one member of staff has caught the disease arising from their work.
“By and large the staff have been fantastic. Everybody understands that this is a transmissible disease, that it has the potential to cause severe illness in all age groups, and [that] those at most risk of contracting it are those in close contact with infectious patients, and that is the staff on the front line within the hospital.
“Our appeal to society would be to assist us, because there is only so much that we can do. And if the numbers don’t drop, then we will exceed our ability to manage people safely.”
In the hospital laboratory, Dr Sinead McDermott, consultant clinical microbiologist and laboratory director, explained how the pressure on the unit was all the greater because, this time round, the hospital is hoping to keep as many non-Covid services operating as it can.
Covid-19 testing by the laboratory for staff and patients is crucial to the whole issue of the efficient deployment of the hospital’s finite resources, especially its isolation beds.
The laboratory has carried out 42,000 tests since March 2020. (It conducts tests for other hospitals also.) During the summer there were days on end when there were no positive results. Over the period since March, an average of 3.6 per cent of all tests have proved to be positive. These days, 10 to 13 per cent of tests are proving positive.
Young Covid patients
Grace Kenny is a young infectious diseases doctor who works in the hospital's post-Covid clinic, which has been seeing patients since May.
The majority are young, and had no underlying health issues prior to contracting Covid. Many suffered a mild dose of the disease during the first surge, but have yet to fully recover.
They have symptoms such as shortness of breath, chest pains, fatigue and “brain fog”, yet no structural problems with their hearts or lungs are evident. There is no particular treatment on offer, other than symptom management.
“The average age is about 40, but we have patients as young as 16. All the patients have some improvement over time, but it is really slow for some people.”
Ten per cent of Covid-19 sufferers can be suffering symptoms four weeks later, and 2 per cent 12 weeks later, according to one study.
“That is not a massive proportion, but if you think of our numbers now, it is a lot of people.”
The clinic’s patients are not only young people, but people who were fit and strong prior to getting sick. Some were even elite athletes.
“It is the thing about Covid that worries me most were I to get it, not landing up in hospital, but that I would end up with these sort of symptoms, because I see a lot of people like me, who were healthy [but] who still aren’t right, weeks and months later.”
Vaccinating the staff
If anxiety was general among those staff members of St Vincent’s Hospital who spoke to The Irish Times on Wednesday, then so too was delight that vaccinating the staff had begun the day before our visit.
Typical of the responses was that of Helfra Griffin, a healthcare assistant working in ED. "The vaccine, hopefully it will give us a better future, so we can hug each other again, and even shake hands. So it is a positive for the hospital."

Westbrook, up in ICU, temporarily lost possession of his analytical manner when talking about getting his jab. “I found it was bizarre. I felt different, as I was waiting. It was almost like the human race was united under one banner. I found it sort of like we were all in this together.”
“Everyone feels so much safer coming to work,” says Gill Carty, assistant director of nursing in ED. “It’s a huge boost.”
Rebecca O’Connor, one of the nurses busy administering the vaccine to her fellow workers, has received it herself. “I was happy to get it. There was a sense of relief, and I sense that’s what everyone is feeling. A sense that something is changing.”
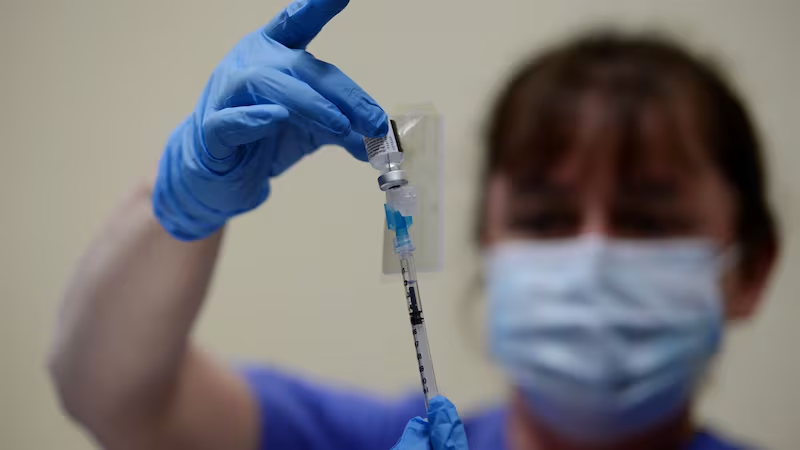
The Pfizer/BioNTech vaccine comes in small vials that have to be stored at minus-70 degrees Celsius. On Tuesday, St Vincent’s was allocated 195 of the precious vials, which were removed from a central storage point that morning and delivered to the hospital.
Once removed from ultra-cold storage, the vaccine has to be used within 120 hours. Back in the hospital, the vials are brought from normal fridge storage to the vaccination centre as they are required for use. Once taken from the fridge, the vaccine must be diluted within two hours and, once diluted, it must be used within six hours. One vial can make six doses.
In one room, overseen by head of pharmacy Paul Tighe, pharmaceutical technicians diluted the vaccine concentrate, with the expiry time for every dose being carefully noted. As needed, the doses were brought to another room, for inoculation by vaccinators such as O'Connor.
In a third room, those who had received the vaccine waited for a while to ensure they had no immediate negative responses.
Vaccination began at 1.30pm on Tuesday, and 246 staff got the jab that day. It resumed at 8 am on Wednesday and, by 2.45 pm, when The Irish Times visits, almost 300 more staff have been given the vaccine. There has been no instance of a negative reaction.
The hospital has 3,035 staff. The vials received on Tuesday mean 1,170 can receive the vaccine. There is no date as yet for the allocation of the vials needed for the rest of the staff.
A second dose will be administered at the end of this month to those who received their first jab this week. The first jab provides immediate protection, but the greatest boost comes from the second shot.
This time round the Irish health service, and St Vincent’s Hospital, is trying to keep as many services operating as possible as it faces into what looks likely to be the worst Covid-19 surge yet. But as the situation worsens, more services will close.

“This is an illness that thrives on people socialising, on people being out together,” says O’Dwyer. “You have to make a decision as to whether you think that sort of socialising is worth the consequences in terms of the burden of illness you are going to see in the weeks afterwards. And it is difficult to make those decisions until you can see the consequences.
“We’ll look back on this in a couple of weeks, and people can make their own minds up as to whether it was worth having the sort of Christmas interactions we had, and the prices people will inevitably pay over the next couple of weeks.”
















