Facing into the winter flu season during a pandemic is a frightening prospect. The severity of the influenza viruses in circulation each year is already difficult to predict, but with lower levels of winter flu in the southern hemisphere earlier this year, there is less data on both the flu viruses themselves and the effectiveness of the vaccine which is developed towards the end of the previous flu season.
And that’s before you even factor in confusing Covid-19 and flu symptoms and the risks of getting both at the same time – not to mention the risks of spreading Covid to vulnerable people by those who think they just have the flu and not coronavirus.
"There hasn't been much flu virus in the southern hemisphere this year because the flu season came at the same time at the Covid-19 lockdowns, and interventions that block Covid also block flu virus," explains Dr Kim Roberts, assistant professor of virology at Trinity College Dublin.
And while, on one level, that might lead to optimism that countries across Europe will have less flu this winter, Dr Roberts cautions that we are not at the same point in restrictions here as places such as Australia and New Zealand were during their winter flu season. "The flu season puts a huge strain on the health services in a normal year and the potential for Sars-Cov-2 [the scientific name for the novel coronavirus which causes Covid-19] to transmit will also see transmission of flu as well," explains Dr Roberts.
Approximately 4,300 people were hospitalised for flu in Ireland in the 2019-2020 flu season, according to figures presented at the Oireachtas Special Committee on Covid-19. And between 200 and 500 people die every winter from complications arising from the flu. With fewer beds in the hospital system due to social distancing restrictions – and fears of a second wave of Covid-19 – the potential impact on hospital services doesn't bear thinking about.
Symptoms
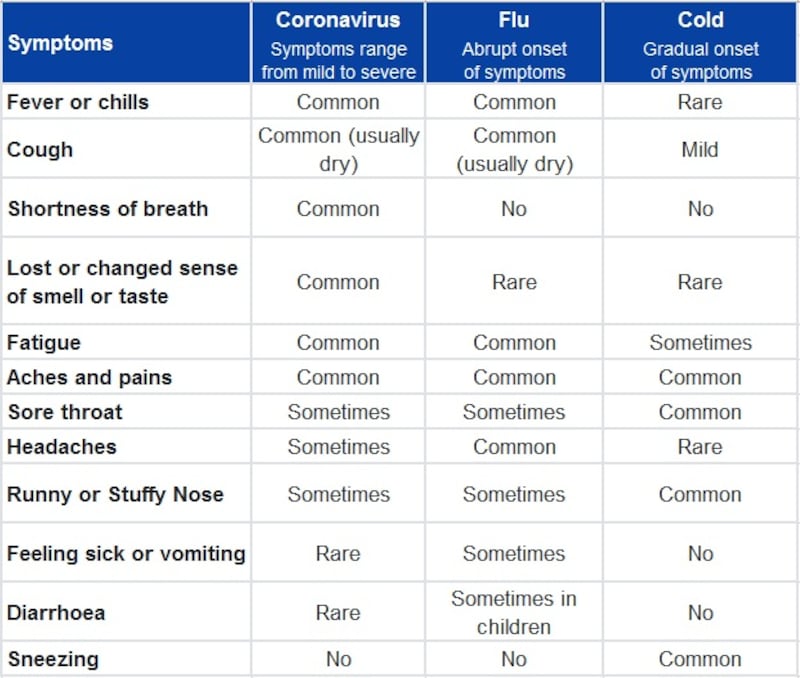
There are also widespread concerns that it will be difficult to tell the difference between flu and Covid-19 symptoms, leading some people to assume they have the flu rather than Covid or vice-versa. Fever or chill, a dry cough, aches and pains and fatigue are common symptoms of both the flu and Covid-19. However, shortness of breath and loss or changed sense of taste and smell are more specific to the novel coronavirus which causes Covid-19. Headaches are more commonly associated with the flu while sore throat is sometimes associated with Covid-19.
“It will be tricky for GPs to distinguish flu from Covid-19 so the best way to protect ourselves and reduce the extra pressure on hospitals this year more than ever is to get the flu vaccine,” says Dr Roberts, who is promoting flu vaccination on behalf of a leading chain of pharmacies. She advises people to get the flu vaccine early as it usually takes about two weeks to take effect. Pharmacies are currently taking online booking from those keen to get the vaccine in pharmacies rather than at GP clinics. The flu vaccine is free for those over 65, people with long-term health issues and children.
Dr Cillian de Gascun, director of the National Virus Reference Laboratory at University College Dublin and chair of the expert advisory group of the National Public Health Emergency Team (Nphet) says that people who have had flu in the past should recognise it. "The influenza virus results in a sudden onset of debilitating symptoms including muscle aches and pains, lethargy, fatigue and night sweats, while the onset of Covid-19 seems to be less dramatic with fever, cough and shortness of breath; [the latter] is not a usual influenza symptom," he explains.
What happens if people catch Covid and flu at the same time? Dr Lucy Jessop, director of public health at the National Immunisation Office, says that early studies from China during the end of the 2019/2020 flu season found that there are more likely to be complications and poorer outcomes in people who have Covid-19 and the flu virus at the same time.
Dr de Gascun says that in some situations, people will need to be tested both for influenza and Covid-19 but that there won’t be a need to do population testing for influenza. “Those with underlying conditions who can be treated with anti-viral medication for influenza should be tested for both and if there is an outbreak of a respiratory illness, people may need to be tested for Covid-19 and influenza,” he says. However, the amount of testing for influenza virus in a normal winter is between 15,000-20,000 tests which compares to 60,000 tests for Covid-19 in one week at the end of August.
Young children and older adults as well as those in other vulnerable groups are most at risk of suffering from complications of the flu, according to Dr Jessop.
October 1st is the designated beginning of the winter flu season. The Health Service Executive has ordered about 1.4 million doses of injectable flu vaccines which are due to arrive in Ireland by the end of September. These will be distributed to pharmacies and GP practices over the course of the flu season.
Who should get it?
Flu vaccination is recommended for everyone over 65, those with long-term medical conditions such as diabetes, heart, kidney, liver, lung or neurological diseases and those whose immune system is impaired either due to treatment or disease. Pregnant women, nursing home residents, healthcare workers, carers and those with a body mass index over 40 are also advised to have flu vaccination.
Another 600,000 nasal spray vaccines, to be administered to children aged two-12, have also been ordered by the HSE for the first time this year. These sprays contain a weakened live flu vaccine which gives a better immune response in children. The injectable vaccine administered to adults has a viral protein rather than a live virus which the adult immune system responds to in order to protect the person catching one of the flu viruses currently circulating. Vulnerable children aged six months to two years and vulnerable teenagers will be given the injectable rather than the nasal spray flu vaccine.
Measures to reduce the spread of Covid-19 – coughing etiquette, hand hygiene, wearing of face coverings and social distancing – might also reduce the incidence of flu here this winter. “Hand hygiene is critical for the prevention of the flu and the “catch it [sneeze or cough into a tissue], bin it, kill it” slogan together with wash your hands have always been promoted for flu prevention,” explains Dr Jessop.
Dr de Gascun adds, “The public health measures introduced for Covid-19 will have an impact on all respiratory viruses. So, if people continue with these public health measures and if there is an increased uptake of the flu vaccine this year, I would be slightly optimistic about the winter season.”
The fact that children are known to be vectors of the flu – but not Covid-19 – is one of the reasons why the HSE has introduced the flu vaccine for children aged between two and 12 for the first time this season. Childhood immunisation for the flu was already under review by the National Immunisation Advisory Committee but the pandemic arguably brought forward its introduction here.
“Children are very good at spreading the flu virus and the World Health Organisation has been recommending flu vaccine for children for years. The winter flu vaccination programme for children started in the UK in 2013,” explains Dr Jessop.
She says that vaccinating children against the flu virus not only protects children themselves but also protects families and vulnerable people such as grandparents. “Vaccinating children against the flu is good for preventing the spread of the influenza virus in the population,” says Dr Jessop.
[ Dr Muiris Houston: Have I got the flu or Covid-19?Opens in new window ]









