Claire Cahill knows what it is like to see your child suffer with scoliosis while waiting for surgery and then witness what a difference the operation makes.
Her son Darragh (11) is so happy and active now, she says, four years after having “magic” growth rods inserted in his back, to address early onset scoliosis with which he was diagnosed at age two.
“It is such a positive outcome you couldn’t but want it for every child,” she says, but “why did we have to go through that horrible 15 months with him before his surgery, when he really, really suffered?” Also, Darragh will have to cope with reduced lung function all his life, partly, she says, due to the delay in care.
She helps run the Scoliosis Advocacy Network that campaigns for timely treatment for children with scoliosis. As they hear from families whose children have had scheduled surgery postponed, they fear the pandemic has set back efforts in recent years to tackle unacceptable wait times.
At the beginning of February, 225 patients were on the waiting list for scoliosis-related surgeries, across Temple Street, Crumlin and the National Orthopaedic Hospital Cappagh, according to Children’s Health Ireland (CHI). Some 128 of those were awaiting spinal fusion and 77 other spinal procedures.
“CHI has made great efforts to continue with scoliosis surgeries despite the restrictions imposed by Covid-19,” it says in a statement to The Irish Times. “By the end of 2020, we had performed 163 surgeries compared with 189 the previous year.”
With the challenges of Covid-19 reducing patient flow and access to diagnostics, “inpatient waiting times have increased and demand for surgery for urgent, semi-urgent and time-sensitive cases has steadily increased through the year”, it acknowledges.
CHI says it is working with the Health Service Executive on plans to set up extra clinics and sessions in the evenings and at weekends, and to secure investment in additional MRI and other scanning equipment. “For orthopaedics, we are expanding our activity in Cappagh hospital. And, subject to HSE funding in 2021, expect to make an impact on orthopaedic long-waiters and, within that, reductions in waiting times for children with scoliosis.”
Orthopaedic clinics
It is also running additional orthopaedic clinics in CityWest, which it says is reducing the number of children waiting the longest for appointments. “CHI sincerely regrets that children and their families are experiencing long waiting times for their appointments,” it adds.
Consultant paediatric orthopaedic surgeon Mr Connor Green carries out scoliosis surgery in both Cappagh and Temple Street hospitals, but in contrasting circumstances, involving very different groups of children.
The planned expansion of Cappagh’s capacity for paediatric surgery is one bit of good news in the ongoing plight of children waiting for scoliosis treatment. Those latest CHI figures show just 15 children waiting for spinal fusion at Cappagh and none there waiting for other spinal procedures, compared with 22 and 35 respectively at Temple Street, and then 91 and 42 at Crumlin.
However, Cappagh does not deal with children under the age of seven, nor does it handle more complex scoliosis cases that need the back-up of a dedicated paediatric hospital.
It is early onset scoliosis (under the age of five) and children with neuromuscular disorders where the most significant treatment delay exists, he says. And this is the sickest group, for whom surgery is urgent and often life-saving.
While a lot of attention has been paid to the situation for children with scoliosis, which is bad, he acknowledges, “it’s nothing compared to everything else” in paediatric orthopaedics. “Particularly in the care of children with neuromuscular and neurodisability problems.”
At Cappagh, Green has pioneered a rapid-access scoliosis service. They accept referrals from GPs all over the country and he screens the letters personally to pick out those who will be suitable for this service. “There is such a backlog in seeing children with scoliosis in clinics, we need to pick out the most urgent cases. The child with the bigger curve needs to be seen sooner.”
Idiopathic cases
The most important thing with scoliosis is what caused it, he says. About 80 per cent of cases are idiopathic, “otherwise-well children who just happen to have scoliosis”, he explains. “But a small number have causes such as brain tumours or spinal cord tumours or blockages in their spinal cord and we have to take those kids out really quickly.”
They have managed to reduce the waiting time for first appointments at Cappagh for idiopathic cases from 18 months to four weeks. By the time he meets children, they will already have been seen by a nurse specialist and X-rayed, and he is able to offer a date for surgery.
“The nice thing about Cappagh being an elective hospital is that the date generally doesn’t change.” While the waiting time for his patients there is about six months, those seeing his colleagues, he says, will be operated on within three or four months.
He acknowledges that, in 2017, the HSE set a target of a maximum four-month waiting time on scoliosis surgery lists. But “we never agreed to it in regard to idiopathic scoliosis because that is not the priority. With idiopathic scoliosis, the child needs to have the operation at a time that suits the child and their family, that is really what we work around.”
We don't have enough theatre capacity, we don't have enough ICU and we don't have enough bed capacity
It’s a very different story in Temple Street, which is dealing with more vulnerable children and where “we don’t have enough theatre capacity, we don’t have enough ICU and we don’t have enough bed capacity”, says Green. “That all existed before Covid.
“With Covid it got even worse because we had to reduce the number of beds to increase the distance between people. It has been really difficult to plan around ICU admissions because ICU is always full. So, it’s pot luck on the day of surgery whether you have a bed available and we routinely have to send children home on the day of surgery because there is no ICU bed available.”
Green has worked in several North American hospitals, as well as other Irish hospitals, “and there is nowhere more efficient in terms of management and nursing care than Temple Street,” he stresses. “It is purely an infrastructural issue. We are working in a Victorian hospital and we are trying to offer this high-level care. Those children, if with me or Prof McCormick, will not have their operation within the next 18 months to two years. That is absolutely unacceptable. Every single child on our waiting list requires surgery immediately.
‘Start deteriorating’
“These are the group for whom it should be happening within four months. The problem with these children is that when we list them for surgery, they immediately start deteriorating and some children we reach a point where they are so sick from their underlying condition and their scoliosis, that surgery is too risky.”
From the start of the pandemic, Green and his colleagues faced not only inadequate infrastructure, but inadequate staffing too, with significant numbers out due to Covid, before the vaccination of hospital staff began. It is an acute hospital where admissions must happen, regardless of patients’ Covid status, he points out.
For children on his waiting list with conditions such as spina bifida and cerebral palsy, they lose their ability to walk if you don’t intervene urgently, he says.
When he came to Temple Street initially, he couldn’t get to children in time before they went off their feet and were no longer walking. “I was trying to get them back walking again, which is a huge difficulty in a family. It takes nine months’ rehabilitation to get a child back up again once they have gone down.
“We have gone a step worse than that now. Unless you have an open pressure sore on your foot or your feet and legs are so bad that an orthotist can’t get the splints on to you and the parents who are trying their best to care for you can’t put anything on your feet because they have open sores on them . . . that is what it takes to get on my waiting list.
“If I operated every day from now until the end of this year, I still wouldn’t clear that part of my list. That is how bad we are.
“Nobody cares about these children because they are not going to contribute financially to society and everybody just wants to put them in a corner and ignore them. It is disgusting and unacceptable.”
Waiting children
While the CHI releases figures relating to scoliosis, it does not issue reports on other specific orthopaedic conditions. But data from the National Treatment Purchase Fund shows that the paediatric speciality with the longest waiting list for an appointment for treatment is orthopaedics. A waiting list of 906 children in January 2020 had grown to 1,138 by the end of the year.
Green says he has about 190 children on his waiting list at Temple Street, approximately 10 per cent of whom would be scoliosis patients, 20 per cent are otherwise-well children and 70 per cent would have neuromuscular conditions such as cerebral palsy, spina bifida, developmental disorders, metabolic disorders and bone dysplasia.
I can go into a clinic with 12 children and go from one room to another telling families . . . that I have no idea when I am going to be able to do their operation
“My access to theatre is half a day once a week, so I can do one child once a week. On average because I work on Mondays, with bank holidays etc, I can operate on 40 children a year.” Meanwhile, three to four patients a week are added to his waiting list.
“For every child I don’t operate on, it could be costing the State hundreds of thousands more in difficult care because their parents then can’t look after them anymore. I can go into a clinic with 12 children and go from one room to another telling families, who can no longer care for their children because they are so disabled and so deformed, that I have no idea when I am going to be able to do their operation.”
That takes a toll on medical professionals too.
“I used to wonder why some of my senior colleagues walked out of the public system and went to private only. The reason is because eventually you burn out in one way or the other. You burn out trying to change the system or you burn out because of the system.”
Referring to the recent Government apology over the mother and baby homes, Green says: “As a group of people who care for children with neuro-disability problems, we feel the next big apology in 20 years’ time is going to be from a government about how neglected these children are now. I am only in my post four years and I already have children on my waiting list for three years for neuro-developmental conditions, with no sign of getting surgery soon.”
However, “it is not because we are not being given the money to look after these children”, he says. “The issue is that Temple Street does not have the physical infrastructure to deal with these children and, as a group, we have absolutely no confidence that the [new] children’s hospital is going to be ready in the next 10 years.”
Scheduled care
The Dail Public Accounts Committee was told recently that it may not open until 2024, while CHI did not respond in time for this article to a query about the latest estimate for when the new hospital would be functioning fully.
At Cappagh, unlike Temple Street, there is space to expand, but it needs a commitment to funding, he says. “As Ireland’s only elective paediatric orthopaedic hospital we provide scheduled care to children and their families without the competition of acute services, which means operations are never cancelled because of a lack of beds and our infection rate is way lower.
“A forward-thinking board at Children’s Health Ireland have seen the importance of this service and insisted Cappagh Kids will be required even when the new hospital is built.”
However, the problem with Cappagh, as he sees it, “is our budget is linked to Ireland East Hospital Group, a busy hospital group with lots of unexpected and acute problems, which mean inevitable budget overruns and then scheduled care in Cappagh suffers”.
Whereas increasing care at Cappagh “will ease pressure on Temple Street and allow us to care for the sickest children there. Our kids can’t wait and unfortunately many have passed the point where surgery can help already.
“A mammoth effort was made for scoliosis but the real problem of neuromuscular and disability care is below that iceberg. We need this problem to be recognised and resources put to where they can make a difference.”
Green fears that when the pandemic is over, there will be an exodus of Ireland’s best medical and nursing staff, “who could be working in any hospital around the world, earning three times what they are earning here”. The system has been surviving for years on “misplaced loyalty to this country” and he believes Covid has finally wiped away the last of the goodwill.
“Successive administrations have failed to recruit and retain the required elite group in the medical and nursing fields and I am sure they will all leave now.”
With such an exodus, “the big white elephant being built in a hole in St James’s might be finished”, but there will be no elite work force to staff it.
“Right now, what we have in paediatric care in Ireland is a world-class staff in Third World facilities but by the time this hospital is built,” he says in exasperation, “we are going to have a world-class facility with staff you wouldn’t let operate on a dog”.
Mille Andersen: ‘I couldn’t believe that I had a straight spine’
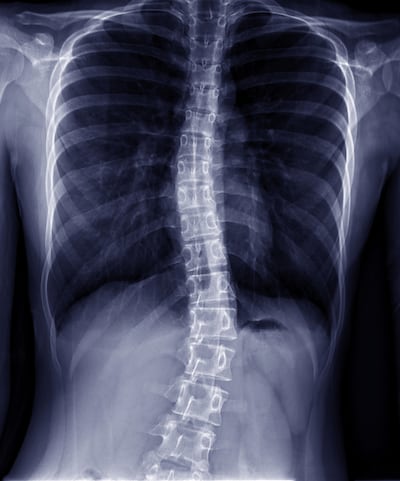
Mille Andersen (17) had surgery for her idiopathic scoliosis at the age of 15 and has since been raising awareness about the waiting list issues for other children and adolescents.
“I was first diagnosed when I was 13 and going into my first year of secondary school. My curve really didn’t bother me then.

“I met a consultant in Temple Street Children’s Hospital and he monitored me closely through the years. I think the main thing worrying me then was the possibility of surgery ahead.
I got tired very easily and I felt uncomfortable. It was hard to sleep.
“I remember when I was on holiday in Spain in 2017, I noticed how different my back’s appearance was from others and that its prominence was very visible in my reflection in shop windows. I started to became more self-conscious.
“I was lucky, in a sense, that I only waited around four to six months for a surgery date after I was put on the list. I was looking forward to growing taller, having a straight spine and just feeling better overall.
“Many of the things I worried about pre-op didn’t turn out as bad as I had thought and the Cappagh hospital team were great for easing my anxieties. I also had great support from family and friends, as well as my school, which had always been very accommodating. I had surgery in May 2018 and remained in the hospital for about six days. Recovery was definitely challenging but manageable.
‘A children’s rights issue’
“I remember taking my first steps, seeing my back for the first time and being taller. I couldn’t believe that I had a straight spine. It felt really weird.
“My mum is a nurse so that was a comfort while I recovered at home in Co Dublin. The first few months I took it very easy, increasing my walking over time. There were a few things I found challenging, like sitting and standing for long periods, but after a while I found my new normal again.
“I loved performing as a child, doing mainly musical theatre. It was more than a year after my surgery before I tried dancing again but it wasn’t the same, as I had new limitations. I have focused on my singing instead.
“Although I didn’t have a very long wait for a surgery date, I can empathise with others on what it’s like playing the waiting game. It can be such a painful and draining condition. Parents should not have to fight for their children to be seen and treated and I believe it’s a children’s rights issue.
“My hope is that waiting lists can be reduced and that children and adolescents don’t have to suffer. I also want to speak out because it can feel isolating if you don’t know anyone else with a similar condition.
“My back is doing okay now. I definitely have my ups and downs with it but I think it’s just about taking it day by day.”











