The President of the High Court has warned it may be open to the Medical Council to take legal action to end the HSE's "scandalous", "dangerous" and continuing practice of permitting non-specialist doctors to be appointed as consultants in hospitals and mental health services.
"The HSE appears to be a law unto itself in this regard," Mr Justice Peter Kelly said.
It “cannot be right” that a difficulty in recruiting doctors at consultant level is addressed even temporarily, by appointing persons inadequately qualified for such posts, he said.
That such an approach has been adopted by the HSE, in breach of its own requirements for the last 10 years, “is scandalous”.
The council, Health Information Quality Authority and Irish Hospital Consultants Association had all expressed serious concerns about this practice but the council considered legislation was necessary to address a lacuna in the Medical Practitioners Act, failure to define “consultant”, the judge said.
While not criticising the council, the judge believed, even without legislative change, it was not “entirely powerless” and it may be open to it to bring legal proceedings aimed at ending “this dangerous practice”.
He hoped such proceedings would not be necessary and the authorities would act to bring “a speedy end to this lamentable situation”.
The judge has directed that his judgment should be sent to the Attorney General; the Minister for Health and secretary-general of his department; the HSE chief executive; Hiqa and the State Claims Agency.
Judgment
After it was delivered on Tuesday, Patrick Leonard SC, for the council, said he hoped the judgment would help bring an end to the situation “relatively quickly”.
The judge had raised several issues with the council concerning the HSE's practice when he last month confirmed its recommendation to cancel the registration of Arjan Kumar Bhatia, a radiologist with an the address at Drumcliffe, Sligo, and at Northamptonshire, England, recruited by an agency to work as locum consultant radiologist at Cavan General Hospital.
Dr Bhatia worked at the Cavan hospital between June and September 2014. After the hospital raised concerns, the council’s fitness-to-practise committee found some 80 allegations involving 43 patients amounted cumulatively to poor professional performance, including failures concerning CT scanning, to see liver abscess, to recognise acute stroke, understating of cancer scans, and missed fractures.
Dr Bhatia previously worked over a number of years in other hospitals in Ireland despite failing the examinations for the position of consultant radiologist, the judge noted.
He reserved judgment on what directions he might issue to the council after receiving detailed material from it concerning the disputed HSE practice.
Giving that judgment on Tuesday, the judge said the evidence was “very disquieting” and showed the lives, health and welfare of patients were being “jeopardised” by the HSE’s approach of permitting doctors such as Dr Bhatia be appointed as temporary and permanent consultants in a wide variety of specialities despite not meeting the HSE’s requirement, set in 2008, to be registered on the council’s specialist register.
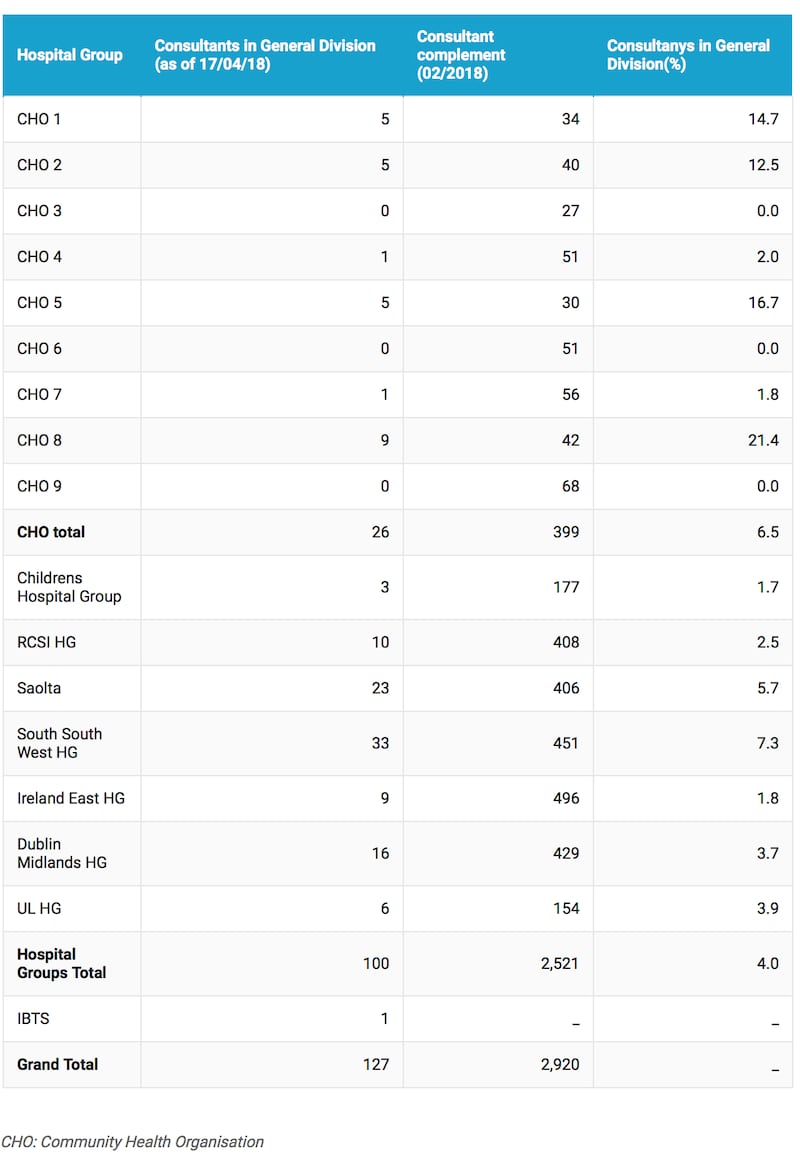
A total of 127 out of 2,920 consultants currently employed by the HSE are not registered on the council’s specialist register and this practice was affecting positions in 20 acute hospitals in a wide range of specialities including obstetrics, paediatrics, emergency medicine and radiology, he said.
He was also concerned at the disparity in distribution of “sub-standard” consultants which was as high as 21.4 per cent in one community health organisation and considerably higher in regional than in other hospitals.
Does not define term
The fact the Medical Practitioners Act does not define the term “consultant” had been used numerous times by the HSE to appoint persons as consultants who were not specialists, he said. That distinction was unlikely to be known by the average patient who quite reasonably would equate one with the other “but with potentially disastrous consequences”.
The position had “actually worsened” since July 2017 when Sinn Féin TD Louise O’Reilly asked a parliamentary question about this practice, he said.
While the HSE has stressed 127 amounts to 4.3 per cent of the consultants’ workforce, that was “no comfort” to patients who may be dealt with by non-specialists.
The council considered the lacuna in the Act meant the only legal requirement for an employer in hiring a consultant was that they be on the general register of the council and was seeking the Act be amended to correct that position, he noted. Passing legislation is a slow business and his judgment was aimed at helping resolve the situation more speedily.
The judge also criticised a “lack of clarity” in the HSE’s response of April 20th to the council’s concerns arising from the appointment of Dr Bhatia and other non-specialists. There was no information whether patients adversely affected by his performance were notified or whether any review was carried out of patients whom Dr Bhatia had dealt with in other hospitals, he said.











