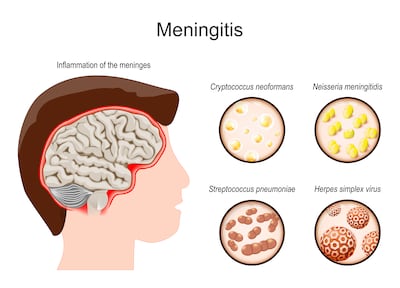
What is meningitis?
It’s an inflammation of the meninges, which are three layers of membranes cushioning the brain and spinal cord. The effects can be fatal or cause lifelong impairments.
What causes it?
“Any bug that can get into the central nervous system can cause it,” says Dr Sinéad O’Donnell, RSCI senior lecturer and consultant microbiologist at Beaumont Hospital in Dublin. “It is usually bacteria or viruses.”
[ Meningitis: I always say ‘my mum’s knowledge saved me’ ]
Bacterial meningitis is always life-threatening, not only in its impact on the brain, but also because it can progress to sepsis – an overwhelming body response to infection, which is what usually causes the fatalities. Meningococcal bacteria are the most common cause of bacterial meningitis and septicaemia (blood poisoning) in Ireland.
Viral meningitis is rarely life-threatening, but can still leave somebody with significant after-effects. Only hospital tests will determine which type somebody has.
Aren’t children vaccinated against it these days?
The vaccines offered under the national immunisation programme only protect against some of the range of bacteria that can cause meningitis. (In addition, the MMR vaccine protects against measles, mumps and rubella, which can cause some types of viral meningitis.)
Although the numbers of cases have dropped very significantly since the introduction here of specific vaccines, starting with one against MenC in 2000, not everybody is vaccinated and no vaccine is 100 per cent effective. It is still important that parents know when to suspect meningitis, and what to do. A rapid response can be the difference between life and death. A total of 27 meningococcal cases were notified to the Health Protection Surveillance Centre (HPSC) last year, of which four were fatalities.
[ HSE urges vigilance as third person dies from meningitisOpens in new window ]
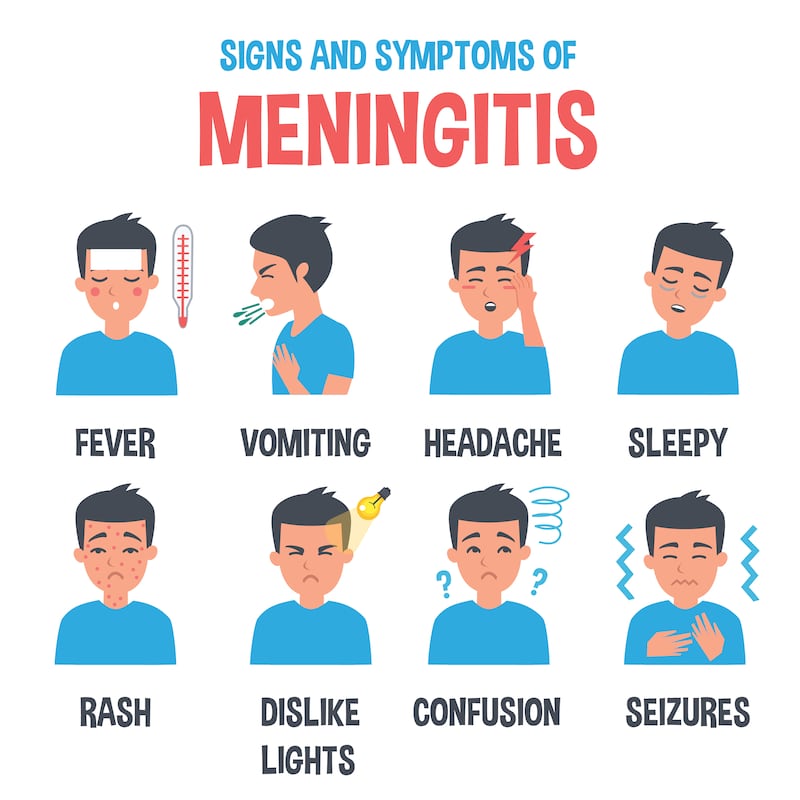
What are the symptoms?
A rash that does not fade when a glass is pressed against it is the most widely known symptom. However, not all forms of meningitis cause a rash – and where it does occur, it may come quite late on, so other signs should be heeded.
“If you see that rash, there is no delaying. You are putting that child, or person, into a car and getting them to an ED. It’s a sign that the organism is in the blood stream, so the probability of sepsis and organ failure is imminent.” Other typical symptoms depend on the age group.
“Babies and toddlers can’t tell you easily they have a headache,” points out Dr O’Donnell. Common indications are irritability, not eating and drinking, a high-pitched cry, being inconsolable and, as the condition worsens, cold hands and feet and rapid breathing.
For older children and young adults, the pattern is likely to be feeling generally unwell to start with, developing headache and muscle pain and then the headache progresses with photophobia, ie dislike of bright lights, and neck stiffness. As their condition deteriorates they are likely to become less rousable, and they can become confused and experience breathing difficulties.
“A lot of the symptoms are quite vague and can be put down to so many other things, but it is the rapid deterioration that is the key thing not to miss,” Dr O’Donnell stresses.
If someone isn’t improving despite taking Calpol or paracetamol tablets, and they are getting worse over a matter of hours, that is when you really have to start thinking that this ailment might not just be a cold or, perhaps in young adults, a hangover.
What should you do if you suspect meningitis?
If your child is becoming significantly more unwell quickly, go straight to a hospital emergency department (ED). GPs do have antibiotics to treat some types of meningitis, “but they don’t have the ability to deal with people who are deteriorating rapidly”, Dr O’Donnell says.
On arrival at the ED, say to staff, “this is progressing, could it be meningitis?”
It’s important to put the question out there straight away, Dr O’Donnell advises, as you know your child better than anyone – and you have also seen the timeline of deterioration in their condition.
How do they test for it?
A lumbar puncture will generally confirm or exclude a diagnosis of bacterial meningitis, and these tests are processed in all labs 24/7. There are blood tests that can be done, but the results would not be back as quickly.
How is it treated?
Caught in time, bacterial meningitis is very treatable with basic antibiotics – but it’s vital to get those antibiotics on board quickly.

For viral meningitis, some anti-viral drugs can be used, but very often just supportive therapy is required, such as painkillers, and keeping the patient comfortable and hydrated, and the illness “will just self-resolve”, says Dr O’Donnell.
Providing the patient survives, are there likely to be long-term consequences?
Possible neurological after-effects, particularly in children, include delayed learning, hearing issues and eye-sight problems. With meningococcal disease and ensuing septicaemia, there can be significant tissue death. This will lead to scarring or necessitate amputation.
People can also have prolonged headaches and infection, as well as psychological issues.
Who is at risk of contracting it?
Everybody is at risk; some people are just more at risk than others. It is more likely to occur within the age groups of one to four years, 15 to 19 years, and among the over-65s.
People with impaired immunity can be more vulnerable, but they are usually identified and have the risk managed through vaccines and prophylaxis, ie preventative medication. Those with a past head injury could have a greater risk too, as a defect in the brain barrier may allow a bug to cross over. We are approaching peak meningitis season now – winter and early spring.
Is there a higher risk during pregnancy?
There is a form of meningitis caused by listeria, for which pregnancy is the commonest risk factor. It is very specific, not vaccine-preventable, but an illness that can have devastating developmental consequences for the unborn child.

This is why you’re advised when pregnant not to eat foods that are more likely to harbour listeria, such as unpasteurised milk and cheese and pate, and to be particularly vigilant about avoiding undercooked chicken or sausages, and also cold meats and chilled seafood.
If one child has meningitis, is the whole household likely to get it?
Bugs causing meningitis can be passed on by coughing, sneezing or kissing. The viral type can be contagious, but not as contagious as the bacterial one. If it’s meningococcal, anybody who has had prolonged contact with the patient will be given antibiotics to prevent them from developing it too.
[ Young woman dies of meningococcal disease in LimerickOpens in new window ]
Thankfully we don’t see outbreaks of meningococcal meningitis in this country, says Dr O’Donnell, mainly because we have good vaccination records and we are very quick with prophylaxis. “Once a case is notified, the situation is managed incredibly well and the likelihood of onward spread would be very low.”
After all that, I want to make sure my children are up to date with the relevant immunisations, so remind me what they are – and what do I do if they have missed some?
The vaccines in the immunisation schedule which protect against some forms of meningitis are:
- 6 in 1 vaccine (Hib component) – offered at two, four and six months through GP practice
- MenB – offered at two, four and 12 months through GP practice
- PCV (protects against pneumococcal infections) – offered at two, six and 13 months through GP practice
- MenC – offered at six months through GP practice
- Hib/MenC – offered at 13 months through GP practice
- MenACWY – offered to students in first year at secondary school, and age equivalent in special schools, and to people who are home-schooled, through HSE school immunisation team
- PPV (to protect against pneumococcal disease) – available for people aged 65 years and older and people aged two years and older with certain long-term conditions eg chronic lung, heart, liver, or kidney disease, through GP practice
Anyone who is concerned that their child or teenager has missed any or all of these vaccines, for whatever reason, should contact their GP practice for advice, says the HSE. While the vaccination programmes did not stop during Covid-19, there has been a fall in the uptake of primary childhood immunisations here, as in many other European countries.
“Declines in immunisation coverage is a real concern, leaving young children vulnerable to vaccine-preventable diseases and leading to a risk of outbreaks,” the HSE tells The Irish Times.
The MenACWY vaccine will be offered to first-year secondary school students from next January, along with HPV and Tdap.










