There is no way of definitively checking you have it, no way of definitively checking if you have rid yourself of it, huge disagreement over how many people have it, and no known treatment once it gets to a certain stage.
Lyme disease – the various grisly strains of the Borrelia bacterium that live in the guts of some ticks – is just the gift that keeps on giving.
I picked it up in a field in July.
At some point, I’m hoping to put it back down again.
There were warnings in the compost toilets, to be fair. No morning’s trudge across the campsite to the elegant wooden boxes for the dawn ablutions was complete without a glance at the warnings about miniature arachnids carrying the northern hemisphere’s very own climate change-induced tropical disease.
Like a lot of people, I just assumed I’d be grand. After a laptop-heavy June, I turned up for some voluntary physical work in England’s west country thinking only of losing a bit of early-30s padding and enjoying spending time with friends.
The first week I was riddled with bites.
That’s nothing new. Various flying invertebrates seem to regard my arrival as a school of sharks might greet the floating carcass of a sperm whale. In the folk tales of some mosquito cultures, I am fondly associated with times of plenty. And by and large, I’m happy to offer up a blood sacrifice now and then to assuage the insect masses, itching and scratching as I go.
This time was no different, with a creative menagerie of bites nestling between the scratches, bruises and cuts sustained in shifting firewood, pallets and intermediate bulk containers.
After breakfast one morning – aha! – I spotted two ticks, about the size of a sesame seed, and had them removed expertly by a first-aider, using a tweezers and a twisting technique.
Job done, you’d think.
The next morning, I sought some cream for my other bites, including one which had begun to annex the greater part of my thigh.
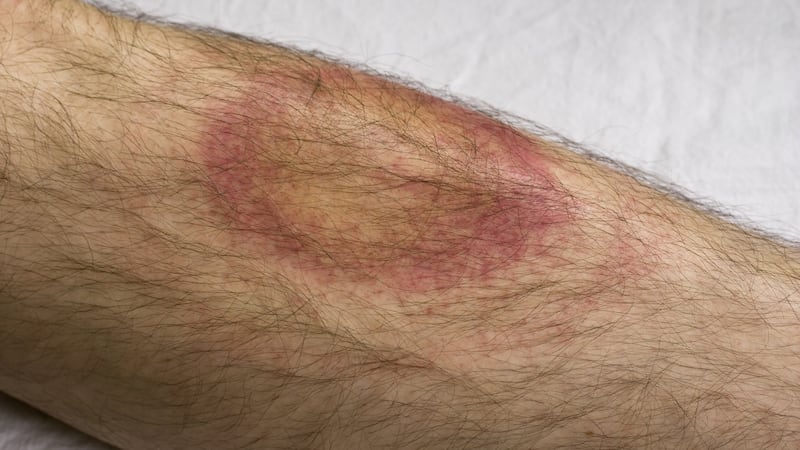
Kirsty, a paramedic on site, took one look at that bite – and two others on my ankles – and identified the telltale signs of Lyme disease: a red bite-mark, surrounded by a pale circle, surrounded in turn by another red circle. It’s like a second World War RAF roundel in miniature.
It explained, she said, why my muscles had ached in an unearthly manner for two days. I just thought it was the result of some uncharacteristic manual labour. “You need to see a doctor now,” she added.
The only problem is that it’s Saturday. A call to 111 and two hours later, and I’ve cadged a lift into town from a generous friend. Her sister apparently got Lyme disease but was only given 10 days’ worth of antibiotics, and it developed into a persistent condition – chronic Lyme disease.
Scary
Chronic Lyme disease is scary. There are documented stories of neurological damage, cognitive problems, seizures, muscle weakness – even heart failure – due to protracted infection from the beauties that are Borrelia burgdorferi bacteria.
Because it seldom follows a clear symptomatic path, some doctors dismiss or downplay it. It often fails to show up in testing. Chronic Lyme is a multi-systemic disease that imitates the symptoms of other ailments: stroke, Alzheimer's, vasculitis, motor neuropathy. Other doctors believe, with some justification, that we are missing 80 per cent of all cases. In Ireland, one consultant in infectious disease has put the estimated number of new Irish cases at 2,500 a year, 10 times his previous estimate, and multiples of the 50-100 listed on the HSE website.
It has been painted as some sort of planetary payback to the emission-producers of the northern hemisphere, and it seems to go after its quarry without fear or favour, robbing Shania Twain of her voice, Kris Kristofferson of his memory, Alec Baldwin of five summers. It left England rugby player Matt Dawson needing heart surgery.
Once it goes from acute to chronic, there is often no cure. Basically, it sounds like you don’t want to allow it to get to that stage.
Hence, then, Kirsty’s urgency to get me to a GP. And hence the GP’s slight alarm when she sees not one but three bites, all showing the telltale bullseye motif of the Lyme-ridden tick, and her acquiescence when I politely asked for a month’s supply of doxycycline.
Hence, also, my willingness to drop my trousers in front of friends at dinnertime, asking if they think the rash is less noticeable than it was before.
Hey, we’re all adults here.
The doxycycline has now run out, but one rash remains. After speaking to a doctor back home, I’m given a three-week course of Amoxicillin: 12 tablets a day. He says blood tests, which just show up antibodies to infections, are useless before six weeks, and inconclusive thereafter. The NHS recently updated its guidance over Lyme disease – the HSE’s date back to 2011.
Many people’s answer to Lyme, and much else besides, appears to involve going out to shoot some non-human animals in the form of deer. Given that Lyme-bearing ticks are most partial to sheep, and also hitch rides on dogs, cats, migratory birds, squirrels and mice, you’d need a lot of bullets.
After being wiped from the doxycycline, I’m taking on the penicillin with two probiotic strains proven to reach the gut alive during antibiotics, and buying enough kefir and kombucha to bathe in.
Who knows what will happen. Either way, I caught it early.
A lot of people don’t get the rash at all, or see the tick. Those are the patients who can end up with chronic, long-term Lyme: doubted by doctors, bewildered by symptoms, and often bereft. And maybe needlessly.
A working Lyme vaccine – approved by the FDA in the US – was withdrawn by its makers in 2002 due to unproven links to arthritis floated by anti-vaccine activists.
Anti-vaxxers and climate change – Lyme disease is very 2019 .







