Being diagnosed with breast cancer is undoubtedly a very difficult experience, but coupled with a gruelling treatment plan, in addition to physical and emotional side effects, the whole journey can really take a toll. Of course, recovery or keeping the disease at bay is the end goal, but some people, while grateful to have survived the ordeal, are left with lasting side effects.
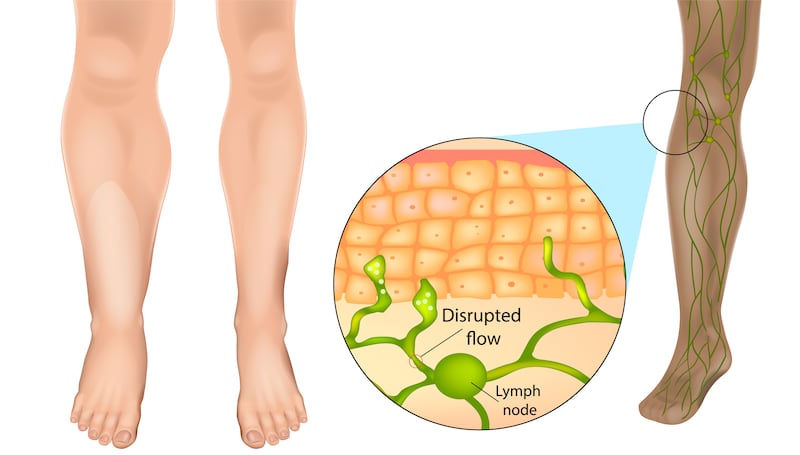
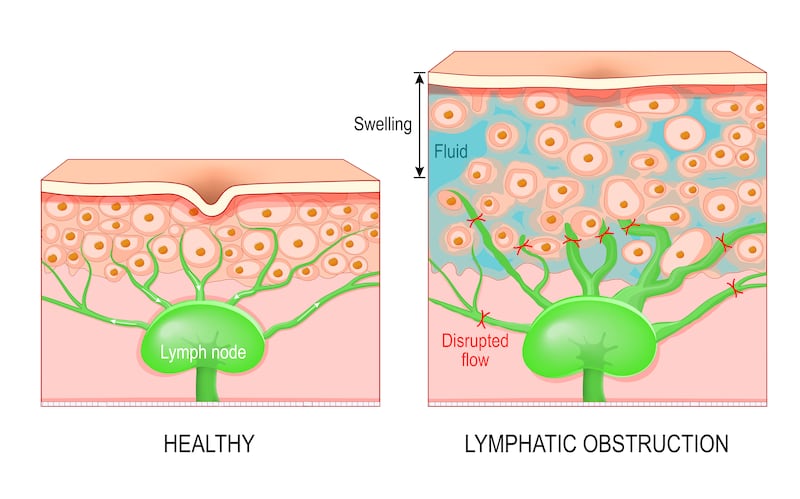
One of these is a condition called lymphoedema which causes swelling in the body’s tissues and can be uncomfortable and painful.
Orla Brennan knows exactly what this feels like as, having been diagnosed with breast cancer in November, 2021, she underwent treatment which involved a mastectomy and an ancillary clearance of lymph nodes. “After being diagnosed with cancer in my left breast, I underwent treatment, during which I met Sinéad Cobbe (a physiotherapist, who has specialised for many years in the area of cancer rehabilitation), a week after my surgery to take my measurements in case of swelling.
She showed me some simple breathing techniques, exercises and manual techniques such as massage to get the lymph moving in the right direction
— Orla Brennan
“Following this, a few weeks later, I noticed swelling in my left arm and hand. I also felt a heaviness in my left arm so I contacted my breast cancer nurse (BCN) and was referred to the Lymphoedema Early Detection Team.”
Q&A: How the new gambling regulator will affect Irish punters
‘My son is getting married in the summer, and the likelihood is that I’m going to be able to see that’
‘There is an undercurrent of racism from some people – you can feel it’
Ireland v France: What time is kick-off and what TV channel is it on?
Lymphoedema is a swelling which can occur in the arm, hand or trunk after cancer treatments including surgery, radiotherapy, chemotherapy and endocrine therapies.
Once Brennan had been diagnosed, the 50-year-old began treatment to try and reduce the swelling and give her some relief. “This all started fairly quickly after my surgery, but Sinéad explained what was happening and loaded me up with leaflets and links to educate myself on the diagnosis,” she says. “She showed me some simple breathing techniques, exercises and manual techniques such as massage to get the lymph moving in the right direction. I was also provided with a compression garment to keep the swelling at bay.
“Before my cancer diagnosis I knew nothing about lymphoedema — or what I call, ‘the nasty cousin of breast cancer treatments’ — and when I was initially diagnosed, my world fell apart and I went straight into survival mode. At the time, the possibility of lymphoedema was shared with me by my BCN, Mags, who knew where my head was. I was focused on getting the cancer out of me, so she said that lymphoedema may or may not happen and we would deal with it, if it did. That was all I could take on board at the time.”
The Clare woman, who is a swimming coach and teacher, is used to being active, so as part of her recovery and treatment, she made sure to incorporate as much exercise as possible into her daily routine. “Mobility is essential to me for work and my daily life.
“I had very serious injuries following a road traffic accident some years ago and spent time in a wheelchair learning to walk again, so I have an existing disability and my daily mantra, is ‘If you can move, do move’ — also, any form of movement and exercise helps to keep my lymphatic system moving.
“So, I swim as regularly as I can, and even started supervised weight training, after getting the go-ahead from my physio. I never thought this would be possible and I’m so grateful, as I believe it has made a huge difference, and I need to do it to strengthen myself and keep my much-fought-for mobility.
It’s human nature for your nearest and dearest to move on (or become less concerned), if and when you’re fortunate enough to have successful cancer treatment
— Orla Brennan
“I also try and minimise symptoms by doing regular manual massage — it’s great to guide the lymph to new pathways, particularly after a node clearance, as it doesn’t know where to go for a while. I also moisturise much more regularly as it’s an essential way to protect my skin — a natural barrier to infection, which can trigger reoccurrence of lymphoedema. I also carry a little tube of antiseptic cream everywhere I go to protect me from bites or burns and use Factor 50 every day.”
Brennan has just undergone a second (elective) mastectomy and says she is determined to keep an optimistic outlook. “I’m a positive person and always on the go. But a cancer diagnosis changes you — and the addition of a lymphoedema diagnosis can be deflating — it’s another bloody thing to be managed.
“It’s human nature for your nearest and dearest to move on (or become less concerned), if and when you’re fortunate enough to have successful cancer treatment. So because lymphoedema isn’t cancer, they come out of survival mode and move on. But you don’t. So it can be very easy to feel like you’re treading this path alone — however, the lymphoedema team are always there, to educate, and provide you with the tools to manage.
“I think that education and awareness of the condition gives you power, and, so far, it doesn’t affect my daily life. I try to make sure to remember all the advice, go back to my links and leaflets regularly, and know what to do if I notice anything different.
“I’ve just had a second mastectomy and I’m in a positive place during recovery. Fair Play to all the ‘Uni Boobers’ out there — but ‘Going Flat’ was my way to be happier and have symmetry on my chest. I had my visit to Sinéad last week and was delighted to hear that my lymphoedema is under control on my left side and no sign of it on my right.”
The cancer survivor says that while having lymphoedema can be tough, she would advise others to take all the support offered and try to be positive. “I was very lucky that there is an Early Detection Lymphoedema Team in place at UHL,” she says. “But I was shocked to find out that it is the only one outside of Dublin. Their support, information and knowledge has been invaluable and early detection clinics should be accessible to everyone all over the country.
“I would advise anyone who is going through lymphoedema to know that they are not alone — they should keep in touch with their breast care team, regardless of where they are. They should also educate themselves on the condition and reach out to lymphoedema professionals and clinics.
This is a crappy diagnosis after or during cancer treatments but it is manageable. You have been through, or are dealing with, cancer
— Orla Brennan
“Much of the management of the condition is about what you do for yourself, so I would encourage them to make a list of the tips they are given and keep them up every day. Also, we have lymph all over our bodies doing wonderful work, but if you don’t move it won’t either — so make sure to hydrate, moisturise and protect the skin and most importantly, breathe.
“This is a crappy diagnosis after or during cancer treatments but it is manageable. You have been through, or are currently dealing with, cancer. Lymphoedema is just an unwelcome nasty cousin who can be managed when it first arrives at your doorstep. Putting into action your education and tools can close the door to that unwanted visitor.”
Currently, almost halfway through the Irish Cancer Society’s three-year pilot project at University Hospital Limerick (UHL) focusing on the early detection of cancer-related lymphoedema, progress of the scheme seems promising. Sinéad Cobbe says the project helps to empower people as well as giving them coping mechanisms to deal with the physical and mental issues associated with the condition. “The primary objective of this service is to educate and empower breast and gynaecology cancer patients in the midwest region, enabling them to attain expertise in assessing their own susceptibility to lymphoedema,” she says.
“This is achieved by educating patients about the structure and functions of the lymphatic system. Patients are encouraged to engage in self-monitoring and manage their personal risk factors for lymphoedema. Strategies encompass physical exercise, weight management, skincare, and recognising the signs and symptoms of lymphoedema.”
Initially, all breast and gynaecological cancer patients receiving treatment in UHL who are deemed high risk for lymphoedema will be referred to the service. Each patient will then have their Lymphoedema Index score measured by a lymphoedema therapist in the physiotherapy department of the hospital pre- and post-treatment. If required, patients will then be treated with compression garments, skin care and tailored exercise programmes and monitored for up to two years.
In general, there is very poor education for health care providers about lymphatics and lymphoedema
— Specialist nurse Kathy Nugent
The programme also offers education and information sessions, online resources and support to patients throughout their involvement with the project. “In general, there is very poor education for health care providers about lymphatics and lymphoedema,” says fellow specialist nurse Kathy Nugent. “Most doctors, nurses and physios get perhaps one lecture on the lymphatic system.
“It is hugely ignored by conventional medicine and a lot of patients have to seek their own answers. Also, there are a lot of scare tactics and misinformation about lymphoedema on the internet and people often get very fearful about it.
“So, the HSE working group has devised information leaflets, to give the best and most up-to-date information, empowering people to become their own experts in lymphoedema prevention and care and reducing the stress and fear associated with it.”
Besides offering this service to patients in the midwest region, Nugent and Cobbe are involved in national initiatives, playing a role in creating lymphoedema prevention booklets and are presently working on an app for the early detection of lymphoedema. “We strongly believe that this information should be available to all individuals undergoing treatments that put them at risk of lymphoedema — this is why the phone app and information leaflets are so important.”













