Parents who trot their children in and out of their local dentist’s surgery once or twice a year and pay for the privilege, might be forgiven for forgetting that there’s free dental care for all under 16s – in theory at least.
In reality, the current public dental service is so chronically underfunded and limited in what it can offer children, that informed parents, with the financial means, make their own arrangements with private dentists. That’s not to say they don’t welcome the opportunities for free examinations and follow-up care that comes their children’s way, probably twice during their time at primary school.
At the severe end of the spectrum, it is estimated there are thousands of children on waiting lists for teeth extractions under general anaesthetic, who may be on multiple courses of antibiotics in the meantime. Approximately 7,000 children a year, according to the Health Service Executive, are referred for this treatment in 20 acute hospitals.
The HSE reports a very high uptake of its routine dental services available through the universal school programme. “Often in excess of 95 per cent of children are screened and offered follow-up treatment where indicated”, according to a spokeswoman, who adds it is planned to see 162,336 children as part of the school programme this year.
But with dental decay affecting at least one in three children by the age of five and the HSE routine services not kicking in until targeted screening at second class in school (age seven/eight) and, typically, not then repeated until sixth class, it’s clearly too late and too little. (In some parts of the country fourth-class children are also invited to attend their local HSE dental clinic.)
Before and after these ages, children only have access to emergency care for the relief of pain (eg toothache) and infection in the public service. Approximately 70,000 children attend for emergency treatment annually, with figures up 4.5 per cent this year. In most of those cases, what’s essentially a preventable disease has become a crisis at a very young age.
Action plan
In this scenario, and with a quarter of a century having passed since the last dental "action plan", there's universal agreement that the National Oral Health Policy, Smile agus Slainte, was long overdue when it was jointly launched by the Ministers for Health and for Employment and Social Protection in April. Its focus on prevention is also widely welcomed.
After that, the views of the policymakers behind the document and the association representing the majority of the professionals whose job it will be to implement it, diverge sharply. Currently, more than four-fifths of all dental care is paid for privately and only 14 per cent is funded by the State.
On paper, what is proposed in the new policy is likely to appeal to parents. Eight preventive oral healthcare packages, each over two years, are promised for everybody between the ages of 0 and 16. These will focus on prevention and primary care such as examinations, preventive advice, fissure sealants and fillings.
Instead of going to the local HSE dental clinic, parents or guardians will be able to choose a dentist for the delivery of these packages to their child. The concept promoted is that of establishing a “dental home” early on in a child’s life.
The pre-schoolers are being prioritised in the first phase, with the Department of Health saying it aims to have the 0-6 care programme available by 2020.
"The policy won't be judged on what it promises, it will be judged on what it delivers," says Dr Kieran O'Connor, chair of the general practitioners committee of the Irish Dental Association, who served as the association's president last year. The association argues that the €80 million-plus funding proposal for implementation of the policy's services is "totally unrealistic" and will make it unworkable.
‘Privatising’ the system
O’Connor, based in Youghal, Co Cork, questions what the thought process could be for “dismantling” a public system that, despite its constraints of under-staffing and lack of resources, has a team of dentists in 220 locations around the country, very committed to, and good at, treating children. “It’s almost privatising the system – although they won’t like that language,” he remarks.
The chief dental officer in the Department of Health, Dr Dympna Kavanagh, who has led the team developing the new policy, rejects the word "dismantling". If the salaried service wasn't so good, "we would not be in a position to move forward", she tells The Irish Times.
The plan to divert routine children’s treatment to primary care and to assign a greater number of more vulnerable adults and some special needs children to public service dentists is not a reflection of what they are doing, she says, “but rather that we feel they should be given a wider remit and an opportunity to use their skills”.
All international research indicates that “you don’t use a salaried service for primary care services, for very pragmatic reasons – they can provide much more time and energy in providing for vulnerable people”, she adds.
This perspective does not seem to have been conveyed to, or at least accepted, within the ranks of the public dental service. “If you talk to the HSE dentists, they say we will be the dumping ground for all the stuff you can’t get somebody else to do – be it the children that can’t find dentists to take them, or the residents of nursing homes who need to be assessed,” says one senior HSE dentist.
Whether or not there will be enough private dentists in the right places willing and able to take over the routine care of children from their public service colleagues is unknown. Nobody has asked the nation’s dentists if they would be prepared to take on children, says Gillian Smith, a general dentist working in Bray, Co Wicklow.
Behaviour management
“Lots of dentists don’t treat children and if they don’t want to treat children, they probably shouldn’t,” she says. “The dentistry of children isn’t complicated but the behaviour management is.”
Smith’s practice has naturally evolved as a centre for children, nervous adults, special needs children and adults, so she would have more in that line than most general practice. She believes the extra time needed for treating children has been overlooked in the plan to transfer the HSE’s child cohort to private surgeries.
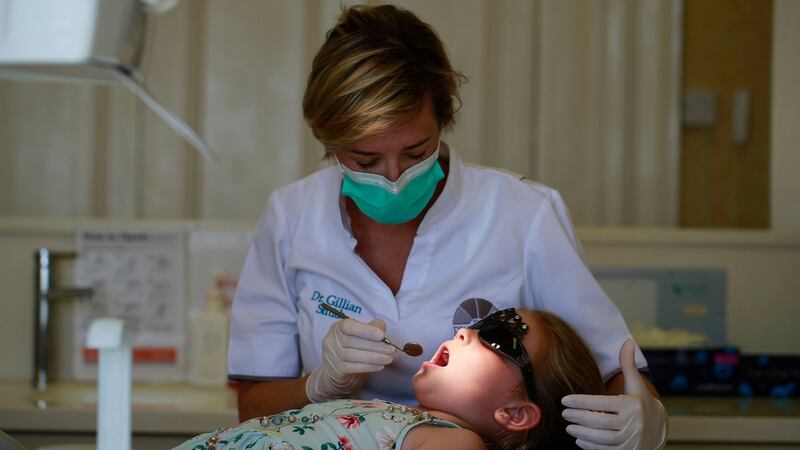
“They vary immensely. You could have a six year old who hops up in the dental chair. Typically, the parents have no dental anxiety; there is great expectations about going to the dentist – no cavity, no pain. They open their mouth, you have a look, there is no treatment needed, you give them a sticker and everybody is happy.
“On the flip side, you have a child who has pain in their mouths, who won’t even open their mouths, never mind sit in the chair. You might be talking an hour before you get a look in their mouth, after playing with them. It might take three visits to do an X-ray.”
Smith says she has tried to see the positives in the new oral health policy and, to this end, singles out the focus on prevention and the move to more involvement with general, community-based practices.
“But the implementation of it is a disaster from start to finish and I think, unfortunately, it is doomed to failure because of that. Even if there are good ideas within it and good aspirations, I can’t see it being successful.”
If this group of patients with huge dental care needs is transferred to private dental practice but then there aren’t enough dentists willing to take it on, it is just going to lead to chaos, she says, “yet the Government will be able to say it is the private dentists’ fault for not treating the patients”.
Deepening divide
Both the Department of Health and the Irish Dental Association recognise the inequities in the current parallel system of public and private dental care for children. However, the former argues that the new policy will address that, while dentists maintain it will deepen the divide.
The association highlights the dangers of what dentists perceive to be a “demand-led” service, which would be “catastrophic” for patients in lower-socio-economic areas with high treatment needs, an assertion that Kavanagh rejects.
O’Connor says that one of the biggest issues the IDA has is that children will fall through the gaps because the new policy depends on parents to be proactive in taking up care packages. Currently, all children are targeted through the school rolls, he points out.
“And if they don’t turn up, we find them,” says one HSE dentist. “The great concern among HSE staff is that we know the ones who need it, the ones whose parents are chaotic or the ones whose parents don’t cook and feed them loads of sugar – that can come from very well-heeled parts of town – they will be the children who will be left behind.”
O’Connor says the targeting and following-up of missed appointments, and the fact that children in pain-seeking emergency care at HSE clinics are generally seen right away, is “a very good safety net”.
Kavanagh denies that what is described in Smile agus Sláinte is a demand-led service but rather that it enables the public “to access services and to forge a relationship with their chosen dental practice – their dental home. To support this universal primary care approach, a safety net system will identify those who do not or cannot attend their local dentist,” she told an Oireachtas Health Committee hearing on the new policy.
A “nudge” letter will go out to every child at age five to say they are entitled to state screening and follow-up treatment, Kavanagh explains to The Irish Times. “We don’t want it worse than before, we want to get in at five, as opposed to getting in at seven or eight.”
Safety net
The child can have that assessment with their existing dentist, if they have one, or pick a dentist operating the scheme. “If all else fails and for whatever reason they don’t want to go there, we would maintain a safety net service within the HSE.”
Establishing a clinical public health surveillance programme is a key priority, she stresses so there is a “helicopter view” of everybody. “We need to ensure we know people are being looked after because if they are missing dental appointments, that’s giving a signal they are missing something else.”

The Oireachtas committee also heard from the Irish Dental Association's chief executive Fintan Hourihan about "disbelief and anger" at how few practising dentists were consulted in the preparation of the policy, "even though they are the ones it is hoped will deliver 95 per cent of dental care in future". He noted that the association had only seen the policy contents for the first time the day they were published.
While a draft of the policy did go out to the HSE for consultation, “we didn’t send it to the IDA because they are a union”, says Kavanagh. They will be involved in negotiating the State contracts for their members.
The IDA, which represents 2,000 dentists across all branches of the profession, argues that there was no "meaningful" consultation during the four years the 158-page policy was being formulated and that it is "naïve" and unworkable. It says it was only given "five headings", which it used to produce its own 16-page document last November, Towards a Vision for Oral Health in Ireland.
"On the face of it they look very similar," says Eamon Croke, a Dublin-based member of the Irish Dental Association, but the fundamental difference is that the Government's consists of "concepts", while the association's is grounded in the reality of the "massive amounts of dental disease out there", and what will drive improvements. "We share common aims – it is how we get there," he adds.
Expert group
Kavanagh counters that an expert group was appointed under the usual conditions Government policy is developed and that the association was briefed on several occasions and invited to give feedback.
“My perception is they thought they should be writing the document or involved in the steering group and that’s understandable. I think people used to do that in the past. Times have changed.”
In addition to the steering group, there was an independent, external panel to oversee research and recommendations, she explains. The process also involved structured interviews with 50 practising dentists and 18 students, about how various aspects would “fly on the ground”, she says, and “they didn’t hold back on their views, which is good”.
“This is a policy for young professionals and the next generation of the public,” she adds. “It is up to the profession to grab hold of it. If it is going to be implemented, it is up to them.”
But the profession’s distrust of the State’s dealings in dentistry runs deep, after years of neglect and cuts. For example, the IDA says the State’s sudden chopping of dental benefits through the medical card and PRSI in 2009 took away €100 million in supports per year.
It would appear significant bridge-building needs to be done if parents have any hope of being able to take pre-schoolers for their first free visit to a local dentist by the end of next year.
Counting teeth: by numbers
- 25 years since the State last produced a dental policy
- 19 per cent only of children, it is estimated, attend a dentist before the age of five
- One in three children are affected by dental decay before the age of five
- 0-six years is being prioritised in the first phase of the new oral health policy
- 162,336 children are expected to be seen in 2019 as part of the HSE's school programme, which it is planned will be replaced by care packages in private dental surgeries.











