At eight months pregnant with her third child, Siobhán Carroll was kept in hospital overnight for observation. On that April evening, she rang home to say goodnight to her other two children, Aoibhe (four) and two-year-old Eimhin, before their father, Noel Carroll, put them to bed.
“I told them I loved them and I would see them in the morning and Aoibhe told me what she learned about in the naíonra that day.”
Sometime later, Noel rang to say that Aoibhe had woken up and vomited, but that he had changed her and tucked her back into bed. Siobhán was sorry not to be there but wasn’t unduly worried.
However, Noel became concerned when Aoibhe got sick again later and he rang the out-of-hours doctor service. He was told there was a vomiting bug going around, but, as the little girl seemed to get worse, Noel was back in touch for more medical advice.
By 5am he was sitting on the couch in the sittingroom of their house in Oranmore, Co Galway, cradling Aoibhe in his arms while they watched cartoons.
When her eyes closed, he thought she was drifting off to sleep, but then he noticed her lips had started to turn blue.
He immediately rang for an ambulance and phoned Siobhán to tell her Aoibhe was very unwell and they were on the way to the same hospital where she was. Siobhán left her bed immediately and went down to the emergency department to wait for them.
“I remember standing at the front door of the hospital in the pitch dark, hearing an ambulance in the distance and thinking: ‘That ambulance is coming really fast, someone’s really sick.’ The ambulance pulled up and Noel jumped out of the front.”
She’ll never forget the look on his face. “By the time the ambulance was there, she had already gone,” she says. “They tried to revive her but it was too late.”
An aggressive strain of meningitis had snuffed out the life of a little girl who, recalls her mother, “loved singing, loved dancing, loved life. We lost her so quickly. In six hours she was gone.”
Meningococcal disease
It’s a stark reminder of how quickly meningococcal disease, inflammation of the protective lining around the brain and spinal cord, can bring tragedy to a family and change lives forever.
Meningitis can cause life-threatening blood poisoning (septicaemia), permanent damage to the brain or nerves, loss of limbs and, in about 10 per cent of cases, death. In the early stages of the disease it can be very difficult to tell meningitis and septicaemia apart from milder diseases as they often resemble common viral illnesses.
Last year, according to the Health Service Executive, there were 13 deaths in Ireland associated with meningococcal disease – eight of which were confirmed due to the disease; for two the precise cause of death was unknown and three are awaiting a coroner’s report. Eighty-nine cases were reported in total.
The latest figures show that this year, up to April 11th, six deaths have been reported as associated with meningitis (although only two of those are confirmed so far) and 40 cases reported.

Siobhán, a Montessori teacher at the time of Aoibhe’s death on April 2nd, 2008, believed she knew about meningitis. “I thought only babies got it and I thought there always had to be a rash.”
They are common misconceptions, as highlighted by a recent survey of Irish parents, the results of which have been released to mark World Meningitis Day on Wednesday, April 24th.
Four weeks after their daughter’s death, the Carrolls’ third child, Noah, was born and the following year they had another daughter, Sophie, now aged nine.
“The biggest thing for me after Aoibhe died was that I felt very alone,” says Siobhán. “I didn’t really know anybody else affected by meningitis and I just felt I had to try to stop someone else going through what we went through.”
This motivated her and Noel to found the Aoibhe Carroll Trust (ACT) for Meningitis in 2011, of which Siobhán is chief executive. The charity began with a Facebook page, aiming to raise awareness of the disease. "The one thing Aoibhe's dad said at the time was if he had known about meningitis – if he had had something in the house he could have looked at," she explains.
Patient support
The organisation evolved into offering direct patient support after they noticed a lot of people were ringing, seeking further information. “They wanted some advice and support because there was nothing out there when you walked out of the hospital.”
There is no aftercare plan for people affected by meningitis, she says. “Once you walk out the door you are left to your own devices.”
It’s the only charity in Ireland that provides a wide range of free support services to families affected by this disease, including counselling, home visits, play therapy and family days. Meanwhile, it is always pushing to make people aware of the signs and symptoms and highlighting the need to act quickly.
Parents may believe that once they have their children vaccinated, they can’t get meningitis. However, there are rarer strains that are not covered by vaccinations, which is why Siobhán stresses the importance of being meningitis aware.
Meningitis and septicaemia are caused by a number of different bacteria and viruses. The vaccines available in the baby and childhood immunisation programme which protect against bacteria that can cause meningitis and/or septicaemia are: Men B (for all babies born after October 1st, 2016), Men C, pneumococcal vaccine (PCV) and Hib vaccines.
In Ireland, babies up to the age of one year are most at risk from meningitis and so these children are now protected by both Men B and Men C vaccines, which cover the most common forms here.
Since the introduction here of the Men C vaccine in 2000, the annual incidence of meningococcal C disease has decreased substantially from 135 cases in 1999 (3.7 per 100,000 population) to 20 cases in 2018 (0.4 per 100,000 population), according to the Health Protection Surveillance Centre (HPSC). The annual incidence of meningococcal B has also reduced considerably from 292 cases in 1999 (8.1 per 100,000 population) to 46 cases in 2018 (1.0 per 100,000 population).
In February this year, the HSPC noted the emergence of the previously rare serogroups W and Y. In 2018, 12 meningitis cases of serogroup W and eight of serogroup Y were reported, along with 46 serogroup B, 20 serogroup C and three “unknown”.
The UK’s National Health Service has offered teenagers and first-year college students a MenACWY vaccine since 2015 and now the Minister for Health, Simon Harris, has approved its introduction here. On the recommendation of the National Immunisation Advisory Committee, the current booster dose of Men C vaccine that is given to teenagers in their first year of secondary school will be replaced with a quadrivalent ACWY vaccine, according to the Department of Health.
“The department is currently liaising with the HSE with a view to implementing administration of the new vaccine during the 2019-2020 academic year,” a spokeswoman adds.

Meanwhile, the HSE encourages all parents to make sure that their children receive all the vaccines that they are eligible for on time, so they can benefit from the protection they provide.
Uptake rates
According to the latest available figures (for the third quarter of 2018), uptake rates for meningitis vaccines are 89 per cent for one dose of Men C vaccine and 92 per cent for one of Men B for children at 12 months of age and 85 per cent for two doses of Men C vaccine at 24 months of age.
Provisional data for first-year secondary-school students show that during the 2017-2018 academic year, 86.6 per cent availed of the Men C vaccine.
ACT for Meningitis runs a "Mind Your Friends" campaign targeting college students who may be living away from their parents for the first time and are a high-risk group for meningitis. Young adults "just feel they are invincible", says Siobhán, who urges them to be vigilant if a friend feels really sick and has a bad headache. "Even if they have been out the night before, it may not be a hangover, it could be the signs of meningitis," she warns. "Go check on them; get them to ring a doctor if not feeling well."
This September, the charity will launch a transition-year campaign to make teenagers aware of meningitis before they go to college. It also connects with nurses and doctors who work on college campuses to keep up their awareness of the risks.
Siobhán understands that health staff everywhere have so many other illnesses to deal with. “That is why we try to empower the parents or the adults themselves to put it to the medical person: ‘Could it be meningitis?’ And let them rule it out then but put the word in their minds.”
The Carrolls are proud of how the charity has grown, undoubtedly saving lives through its awareness raising and trying to make sure that other families are not alone on their journey after meningitis.
Siobhán sees it as a fitting legacy for Aoibhe: “I just wanted her to be remembered in a positive way and not as being the girl who lost her life to meningitis.”
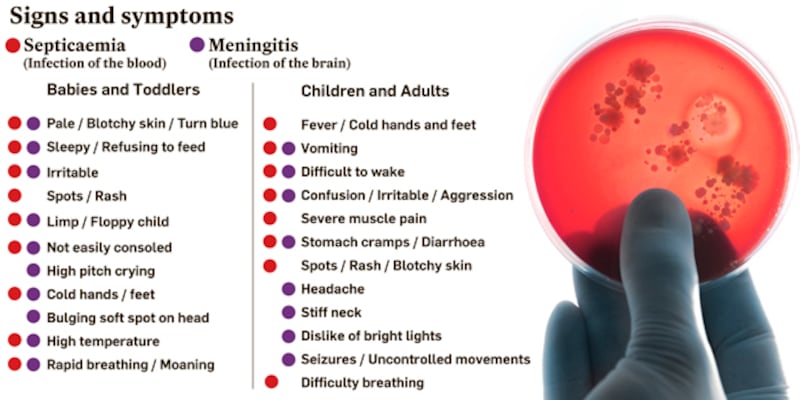
Meningitis symptoms
Vomiting, seizures and cold hands and feet are some of the least-known symptoms associated with meningitis, according to a new survey of Irish parents.
A rash is the sign most commonly cited, by 84 per cent of parents, even though it may appear at a late stage of the disease – or not at all. While that's testament to the success of public awareness campaigns about the rash and how it won't fade under a glass, there is more to it, says Dr Philip Cruz of GSK, which conducted the survey.
A paediatrician by training, he suggests parents of older children should ask themselves if the symptoms resemble flu. Those with babies should be alert to marked irritability, refusal to feed and floppiness.
“It’s all about having a high index of suspicion. Have always at the back of your mind that it could be meningitis,” he advises.
Cold hands and feet could be there at early onset, he explains. And while “irritability” is a broad term, look to move a baby’s limb or neck. As meningitis is an inflammation of the membrane of the brain and spinal cord, “minimal movement can really be very painful”.
Cruz also stresses the urgency of seeking treatment for a disease which can be “devastating” in the way that it can cause a patient to go from being well to in danger of death within hours. “Even though it’s rare, symptoms can really develop very quickly.”
He encourages parents to trust their instinct – if they feel something isn’t right, bring the child to a healthcare professional.
Only one in four of the 375 parents participating in the online survey was aware that, in addition to babies and children under five, young people aged 15-19 are also a high-risk group.
An estimated 10-20 per cent of adolescents carry the bacteria at the back of their throats and noses but they may be perfectly healthy. However, the bacteria can trigger harmful effects when something goes wrong in the immune system, says Cruz, who is GSK’s vaccines medical director for the UK and Ireland.
A high level of social mixing among students – through close living quarters, crowded venues, intimate contact and smoking – facilitates transmission of the disease.
Confusion about different strains of meningococcal disease was also evident among the parents surveyed. Just over a third (37 per cent) were not aware of any of the major types – A, B, C, W, X and Y.
Less than half (46 per cent) said they were aware of meningococcal B and just under a third (32 per cent) said they were aware of meningococcal C, although these two strains account for the majority of disease in Ireland. There were also extremely low levels of knowledge about other strains, with just 2 per cent knowing of Men W and 1 per cent familiar with Men X and Men Y.
This lack of knowledge was also highlighted by parents of 15-19-year-olds reporting that 62 per cent of those children had received the Men B vaccination as part of the HSE vaccination programme, even though it is not available through the programme for that age group.
To mark World Meningitis Day (April 24th), GSK has launched a Know Meningitis campaign through social media to generate awareness of the disease and offer advice on how to spot the signs and symptoms.











