Dr Donal O’Shea
(Consultant endocrinologist at St Vincent's University Hospital Dublin)
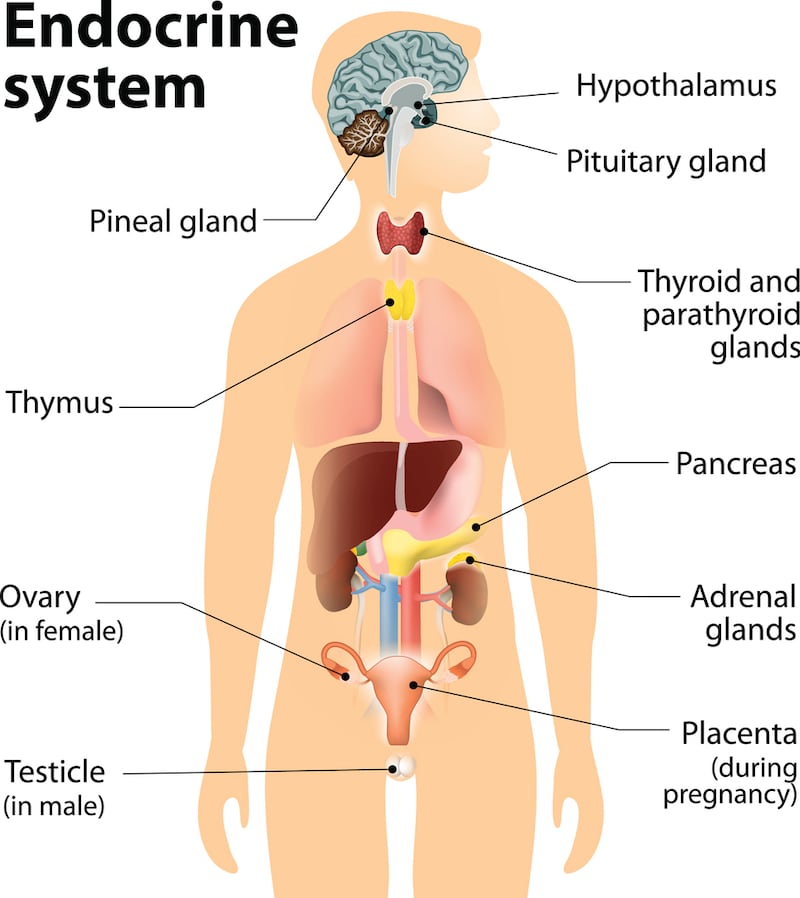
If I had a penny for every time I was asked what exactly an endocrinologist does, I could make a big donation to Diabetes Ireland. Endocrinology is the speciality that deals with hormones – they are chemicals made in one part of the body that travel via the bloodstream to affect another part of the body. For example, insulin is a hormone made by cells in the pancreas and it helps cells all over the body take in sugar.
I love growth hormone which is made by a gland in your brain and is responsible for your bones stretching and your organs growing during childhood and in adulthood. It is important for energy levels. Hormones do different jobs at different stages of life. My favourite hormone is Glucagon Like Peptide-1 – GLP-1 - (it has been nicknamed Good Little Peptide). It is released from your gut after you eat and it does several things. It stimulates insulin release from the pancreas, it makes you feel full (so you stop eating!) and it also regulates your immune system, keeping it calm. GLP-1 is now being used as a treatment for diabetes and obesity. With hormone problems you can either have too much or too little. When there is too much, you have to block the production – or remove the gland that produces it. When there is too little, we can usually replace the hormone with either a tablet or injection. By far the most important tip for a healthy endocrine system is a healthy diet – that allows the hormones to be made and also minimizes the stress that type 2 diabetes and obesity put on the endocrine system.
Dr Carla Moran
(Consultant Endocrinologist, Beacon Hospital, Dublin)
The thyroid gland is butterfly shaped and sits in our neck. Thyroid diseases are very common, especially in women. Thyroid gland overactivity ("hyperactivity") happens when the thyroid gland makes too much thyroid hormone. Typical symptoms include weight loss, shakes, poor sleep, irritation, an awareness of the heart beat, warmth. The most common cause is the autoimmune condition Graves' disease, where the body makes tiny proteins called antibodies that tell the thyroid gland to make too much thyroid hormone. Thankfully, thyroid gland overactivity almost always responds very well to medication to lower thyroid hormones. Some people require other treatments, such as radio-iodine (a once-off oral medicine with radiation activity) or surgery to remove part or all of the thyroid gland.
An underactive thyroid gland (“hypothyroidism”) happens when the gland makes too little thyroid hormone. People experience fatigue, weight gain, constipation, dry skin and hair, and can feel cold. It can sometimes take a while for people to recognize the symptoms or seek help from their GP. But the missing hormone is easily replaced with a tablet once a day, which has no side effects.
GPs are very familiar with thyroid diseases and can measure thyroid hormone levels. Thyroid diseases are usually straightforward to diagnose and treat. Most people completely recover from the condition and have no lasting effects. I advise people to avoid high-dose iodine supplements; these are often marketed as “thyroid supplements” but in fact can be harmful to the thyroid gland. A healthy balanced diet will provide all the iodine our thyroid gland requires.
Claire Naughton
(Regional Development Officer with Diabetes Ireland)
Diabetes is a lifelong condition characterized by high blood glucose (sugar) levels due to the body not making insulin or not having enough working insulin. There are many different types of diabetes but the most well-known are type 1 diabetes and type 2 diabetes. People with diabetes needs to self-manage their condition to keep the blood glucose levels within normal range so that they can live a healthy life and avoid any potential short- and long-term complications.
For someone with type 1 diabetes, daily diabetes management tasks include taking insulin injections or using an insulin pump. They also need to check their glucose levels continuously throughout the day to balance insulin with food intake and physical activity levels.
For someone with type 2 diabetes, having a healthy balanced diet and taking regular physical activity is key to successful management. Medication may also be prescribed to help manage the condition.
Anyone with diabetes should have twice yearly check-ups in a diabetes clinic or with their GP to ensure that they are managing the condition well and to screen for any potential complications of diabetes. These check-ups include a medication review, blood and urine tests and checks on blood glucose, blood pressure and cholesterol. An annual foot assessment to check circulation and sensation, and an annual eye test via the National Diabetes Screening Service is also important. Diabetes Irelandis the national charity in Ireland dedicated to helping people with diabetes. We provide support, education and motivation to everyone affected by diabetes.
Prof Declan Cody
(Consultant Endocrinologist at Children's Health Ireland at Crumlin)
Type 1 diabetes is the most common endocrine disorder in children in Ireland with approx 250 new diagnoses per year nationally in children and adolescents.
The other common disorders we see in children include growth hormone deficiency, short stature, over and under-active thyroid conditions, and early or delayed puberty.
Rarer conditions include those affecting the pituitary gland in the brain (which acts as the “control centre” for the other hormone-producing glands), the adrenal gland and problems with calcium metabolism. Children who don’t have enough adrenal gland hormones usually require lifelong steroid replacement. During times of stress such as illness, trauma or surgery; they will require extra doses of hydrocortisone.
Some endocrine conditions can also be identified in newborn babies. For example, infants who have very low blood sugars due to hyper-insulinism require urgent treatment. Treatment can at times be complex and the missing hormones may need to be replaced if they’re deficient. Occasionally we need to block the over-production of some hormones. In most cases, there is no need for children to do extra exercise or avoid foods. Treatment is mostly about taking the hormone therapies they are prescribed and regular follow-ups in-clinic along with frequent blood checks of hormone levels.
Dr Rachel Crowley
(Consultant endocrinologist at St Vincent's University Hospital, Dublin)
Most endocrine system tumours are rare and are only discovered during scans investigating other complaints. Thyroid cancer is the exception. It is diagnosed if biopsies of a lump in the neck are found to be malignant.
Neuroendocrine tumours (NETs) form in the neuroendocrine cells scattered throughout the body, so symptoms depend on where the tumour is. NETs in the gut can cause stomach upset. NETs that have spread to the liver can cause flushing and palpitations. NETs in the lung can cause asthma-type symptoms. The treatment for the NET depends on its location and the patient. It can include surgery, medications and a specialised type of radiotherapy. People living with these conditions often have to attend hospital regularly for multiple scans and blood tests.
Keeping track of medications and clinic letters is very useful when meeting different medical teams. Maintaining general health with a healthy diet, exercise and sleep means that patients are fit to receive any extra surgeries or treatments they may need over time. It can be really difficult for patients to live with a long-term diagnosis of a tumour over many years, so talking to the medical team about their concerns, seeing a counsellor or liaising with patient groups can support patients’ mental health.
Five experts, five tips
- GPs
- Heart health
- Musculoskeletal
- Digestion
- Respiratory health
- Urological health
- Reproductive health
- Brain health









