The number of Irish people who are living after cancer has grown by more than half over the past decade as survival rates continue to improve.
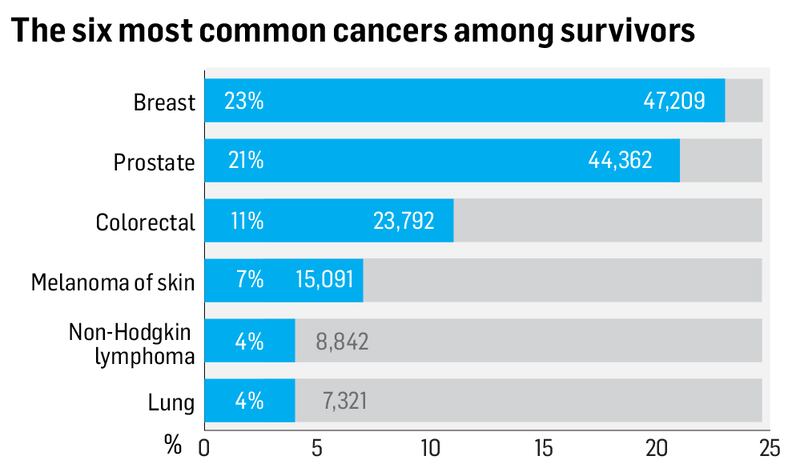
One in every 24 people in the population has survived cancer as the number of survivors passed the 200,000 mark for the first time, according to the latest annual statistical report from the National Cancer Registry. Almost half of the 207,000 survivors have experienced breast or prostate cancer.
However, 10 per cent fewer cancer diagnoses were made in 2020, due to the impact on services of the Covid-19 pandemic. This is equivalent to about 2,000 fewer people diagnosed with the disease than might have been expected.
There was an 11 per cent drop in the number of microscopically verified cancers in 2020, compared with what was expected, according to NCR Ireland. These figures are lower than the 10-14 per cent drop suggested last year by preliminary data.
Are Loughmore-Castleiney and Slaughtneil what all GAA clubs should strive to be?
Wake up, people: Here’s what the mainstream media don’t want you to know about Christmas
Chasing the Light review: This agreeable Irish documentary is all peace and healing. Then something disturbing happens
Your work questions answered: Can bonuses be deducted pro-rata during a maternity leave?
There is further evidence of the improving survival rate in a rise in the median age of death for all invasive cancers, up to 74 years from 72 in the 1990s. For all cancers, the median age at diagnosis remains at 69 years for men and 67 for women.
“These data tell a clear story of improvements in cancer survival rates over time,” according to Dr Jerome Coffey, chairman of the NCRI board.
Cancer accounts for about 30 per cent of deaths each year in Ireland – an average of 9,493 a year from invasive cancer, or 9,751 from all types of tumour, between 2018 and 2020.
Lung cancer is still the leading cause of cancer death, followed by breast and bowel cancer in females, and prostate and bowel cancer in males. Bowel cancer was the second most common cause of cancer death among men for many years but during 2018-2020 its ranking fell to third place, behind lung and prostate cancers.
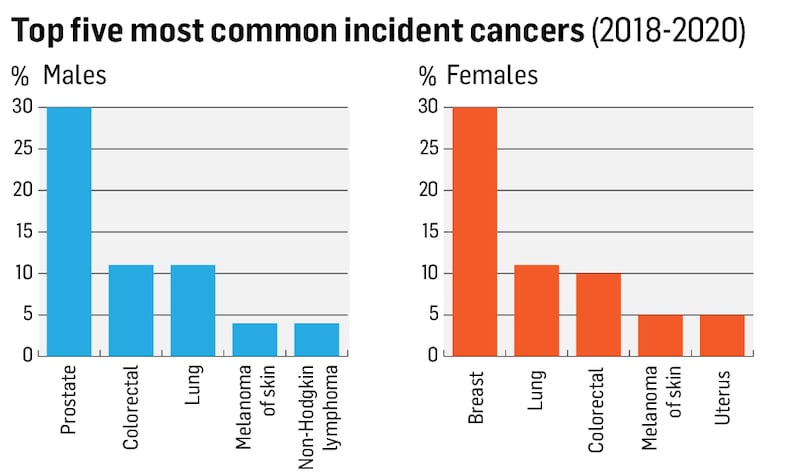
On average, 43,470 cancers or related tumours were diagnosed each year between 2018 and 2020. Excluding non-malignant skin cancers, there were 24,327 invasive cancers each year.
Prostate cancers account for 30 per cent of cancers in men, and breast cancers account for 30 per cent of cancers in women.
For invasive cancers, the five-year survival rate for patients diagnosed between 2014 and 2018 averaged 65 per cent; this compares with only 48 per cent for patients diagnosed in 1994-1998.
Survival rates still vary hugely for different types. In general, the cancers with the poorest prognosis remain lethal but have seen substantial relative improvements in survival rates. For example, the survival rate for oesophageal, pancreatic, liver and lung cancer have all doubled since the 1990s.
The biggest improvement is for multiple myeloma, up 37 percentage points, followed by prostate cancer with a 28 percentage-point improvement.
Five-year survival rates vary from over 90 per cent for cancers of the testis, prostate, melanoma skin and Hodgkin lymphoma down to 24 per cent for lung and oesophagus, 19 per cent for liver and 14 per cent for pancreas.
Cancer services were revamped and consolidated from 2005 on but, as NCRI director Prof Deirdre Murray said, the impact of investment in services could take years to become manifest at a population level.
“Our report this year highlights some key successes that have been achieved over the last decade. The question of the impact of Covid-19 remains a priority for the NCRI as we continue to research the extent and longer term sequelae of the pandemic.”





