In 2019, University College Cork (UCC) researchers noted - From isoniazid to psychobiotics: the gut microbiome as a new antidepressant target - that the first antidepressant discovered was an antibiotic: “Isoniazid was an antibacterial drug developed in the USA in the 1950s for treating tuberculosis”.
The observation that isoniazid improved mood was associated with inhibiting the action of monoamine oxidase enzymes, thus increasing the concentration of monoamines like serotonin in the brain. Subsequent development of antidepressants including selective serotonin-reuptake inhibitors (SSRIs) – that increase the availability of monoamine neurotransmitters – heralded the “chemical imbalance” hypothesis, which emerged in 1967, and asserts that antidepressants rebalance the wayward brain chemistry associated with depression.
However, a recent review in Molecular Psychiatry - The serotonin theory of depression - led by University College London’s Prof Joanna Moncrieff claims “there is no convincing evidence that depression is associated with, or caused by, lower serotonin concentrations or activity”.
What are the implications for psychiatry and patients? Gerard Clarke is professor of neurobehavioural science in the Department of Psychiatry and Neurobehavioural Science at UCC, and a principal investigator in APC Microbiome Ireland. Commenting on Prof Moncrieff’s review, Prof Clarke explained that the antidepressant drugs targeting neurotransmitters like serotonin preceded the chemical imbalance hypothesis: “The initial chemical imbalance hypothesis,” says Clarke, “prompted research into the underlying neurobiology, but the hypothesis was judged too simplistic with many limitations, including the caveat that there’s a delay in the onset of antidepressants’ action which is unexplained by its overly-simplistic early version.”
Prof Moncrieff’s review, adds Prof Clarke, mostly addresses evidence for this simple version of the chemical imbalance theory and – importantly – the efficacy or safety of antidepressant drugs is not evaluated: “We now realise that antidepressant action may involve multiple pathways following engagement of the antidepressants with neurotransmitters like serotonin.”
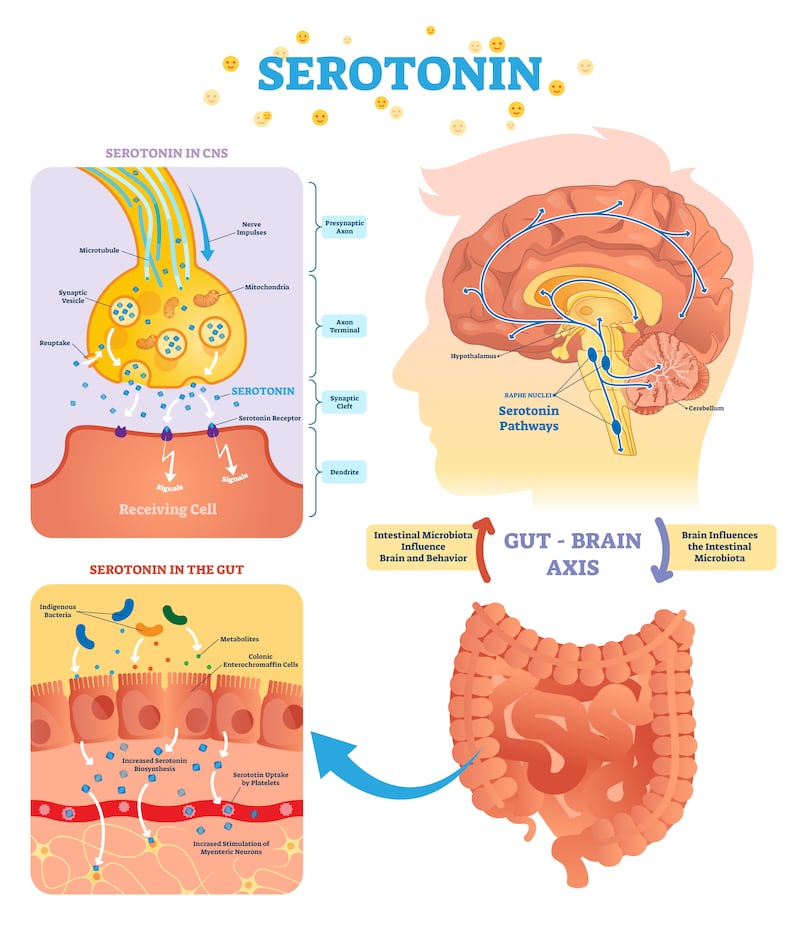
Clarke also explains that serotonin doesn’t cross the blood-brain barrier, “raising questions about using indirect measures like peripheral serotonin to road-test the chemical imbalance hypothesis”. Interestingly, most serotonin detected in blood plasma originates in the gut, and Prof Clarke’s research includes a focus on tryptophan, the precursor to serotonin and other neuroactive metabolites. Unlike serotonin, tryptophan is a building block that does cross the blood-brain barrier, and a systematic study co-authored by Prof Clarke – The kynurenine pathway in major depressive disorder, bipolar disorder, and schizophrenia: a meta-analysis of 101 studies – and, significantly, excluded from Prof Moncrieff’s review, found decreased tryptophan associated with depression: “Acute tryptophan depletion,” says Clarke, “a protocol used to challenge the serotonergic system, provokes re-emergence of depressive symptoms in previously depressed patients who’ve responded well to SSRI antidepressants.”
Further, Prof Clarke says that evidence supporting the efficacy and safety of SSRIs is not contradicted by Prof Moncrieff’s review. “But SSRI’s,” he adds, “aren’t necessarily the only option. Psychological therapy is valuable and an important part of current treatment guidelines, as are the benefits of exercise and diet. Major depression is complex, heterogenous, and a ‘one size fits all’ approach to its clinical management is unrealistic, but antidepressants like SSRIs are important parts of the clinician’s toolkit.”
Prof Clarke points to innovative drug discoveries in this area, and the possibility of drugs that focus on other pathways, with some – like ketamine – prompting a rapid antidepressant response.”
While Prof Clarke does not treat patients with depression, Prof Gautam Gulati does. Consultant forensic psychiatrist and adjunct professor at the University of Limerick, Prof Gulati reminds us that depression “is a serious illness which, like certain physical illnesses, can be severe and life-threatening. It would be reductionist to explain this solely through a single neurotransmitter hypothesis.”
As a practising clinician, Gulati observes that depression has complex underpinnings including, but not limited to, genetics, biology, social adversity, and psychological vulnerabilities. He acknowledges evidence of neurotransmitter abnormalities, “but this is only one piece of an elaborate enigma. As clinicians we aim to formulate causation on an individual basis for each patient, which provides important clues to the treatment approach most appropriate for that person.”
Is it helpful to discuss such topics as this in mainstream media? Prof Clarke welcomes responsible debate about the neurobiology of mental health disorders, “especially if it enhances discussion and enriches public understanding”.
Highlighting the importance of a debate reflecting our relatively poor understanding of certain disorders, while current research tries to bridge knowledge gaps, Prof Clarke cites as an example a commentary on Prof Moncrieff’s review in the academic website, the Conversation - Depression is probably not caused by a chemical imbalance in the brain - which states: “We conclude that it is impossible to say that taking SSRI antidepressants is worthwhile, or even completely safe.” This, says Prof Clarke, far exceeds what can be concluded from Prof Moncrieff’s review: “There’s value in assessing the evidence, but a need to communicate results responsibly.”
For patients, Prof Gulati stresses the importance of people with depression seeking help. “Ample evidence shows that antidepressants and talking therapies like Cognitive Behavioural Therapy can treat the illness effectively, particularly in combination with each other, and when the illness is moderate or severe. This can reduce suffering, improve quality of life, and often reduce the risk of suicide. In mild depression, a healthy diet, moderate exercise, and supportive counselling are helpful, and antidepressant medication is usually not prescribed.”
Understanding the lived experience of mental illness is central to the debate, says Prof Clarke, and this, he says, is now on the radar of many researchers and funding agencies, and a focus of UCC via Dr Emmy Racine, programme manager in the Public and Patient Involvement (PPI) Ignite network: “In that sense we’re already evolving, with researchers like me increasingly aware of the patient voice and how to have these conversations to enrich the quality of our studies, including disseminating our work to the public.”
As Prof Clarke notes: “More PPI involvement in the press release associated with Moncrieff’s review might have changed the nature and quality of the subsequent media debate.”




